Improving Systems of Follow-Up Care for Traumatic Brain Injury: Proceedings of a Workshop (2023)
Chapter: 3 Elements of a System of Follow-Up Care for Mild TBI
The second session of the workshop discussed the core components of transitional and multidisciplinary follow-up care for traumatic brain injury (TBI) patients, particularly at the milder end of the severity spectrum, as well as barriers to the implementation of these elements in care systems. Speakers shared overviews of several models and programs for transitional care and for TBI follow-up services to illustrate these ideas and help to identify common features and differences.
KEY COMPONENTS OF TRANSITIONAL CARE
Karen Hirschman, research professor, University of Pennsylvania School of Nursing, described the role of transitional care, which is a set of time-limited, evidence-based services designed to ensure continuity of care and prevent poor outcomes during care transitions, such as emergency department (ED) visits or hospital readmissions, explained Hirschman. She provided a foundation for the conversation by first describing common issues encountered during patient transitions between care settings, organizations, and/or providers (Hirschman and Hodgson, 2018). Poor continuity of care can occur when information is not transferred or adequately communicated between different providers or between providers and patients, she said. For example, hospitals sometimes provide patients and caregivers with complex treatment regimens at discharge without allowing sufficient time for them to process the information and ask questions. Maintaining continuity of care is less likely when a patient is discharged from the hospital without understanding appropriate next steps; this can be exacerbated by health literacy issues and language barriers. Similarly, she noted that lack of collaboration can undermine the continuity of care if providers fail to engage patients and caregivers in care plans or make treatment decisions without sufficiently assessing or including patient preferences and goals. Care transitions can also be complicated by comorbid health issues, such as chronic conditions, cognitive deficits, depression, or substance abuse, and social factors, such as inadequate housing and food insecurity.
Transitional care aims to minimize the occurrence of these issues, and its core components include engagement, education, well-being, complexity management, care continuity, and accountability. Engaging patients and caregivers involves identifying their priorities, goals, preferences, perspectives, needs, and capabilities. Furthermore, professionals need to foster shared decision making, promote shared accountability, and ensure trusting, reciprocal, and respectful relationships (Naylor et al., 2013).
Hirschman noted that effective education efforts begin with providers assessing what patients and caregivers already know, determining what they need to understand, and educating them to address relevant knowl-
edge gaps. Although transitional care is time limited, it generally features multiple interventions along a continuum of support toward independence. The process of assessing well-being in patients and family caregivers needs to acknowledge their current stressors, she said—for instance, the uncertainty of not knowing what to expect in the TBI healing process—and foster person-centered coping skills with a focus on quality of life. Managing complexity involves examining and, as appropriate, streamlining medication and care plans, and identifying any underlying causes for hospitalization. This component of transitional care is particularly relevant for older patients, Hirschman said, as they are more likely to have multiple chronic conditions.
Care continuity avoids breakdowns of care and can be accomplished by providing support to patients in navigating various health and community settings. Accountability is maintained when (1) clinicians are accountable to patients and family members, (2) the care team is responsible to one another in providing excellent interventions, and (3) the organizational structure supports the team and clinicians in successful implementation of transitional care.
A model for transitional care considers contextual factors, services, and needs, said Hirschman (Grembowski et al., 2014) (see Figure 3-1). For example, a needs assessment can be used to identify a patient’s social supports and caregivers; unmet needs identified through this process can be linked to additional health care and community services and resources. Ideally, transitional care improves the patient and family caregiver experience, health, and well-being while decreasing ED visits, hospitalizations, costs, and caregiver burden. Hirschman illustrated these points by describing a transitional care model from the University of Pennsylvania School of Nursing. During hospitalization, hospital staff identify patients requiring transitional care. The nurse serving as team lead engages with each identified patient and their family, conducts a comprehensive assessment, and initiates collaboration with the health care team. Within 24 hours of discharge, the team lead visits the patient at home or in the subsequent health facility to foster engagement, reassess needs, and identify goals. Interventions may involve additional home visits and are focused on collaborating, communicating, fostering coordination, promoting continuity with providers, managing symptoms, and educating patients and families to promote self-sufficiency. Hirschman noted that transitional care plans can be tailored to specific populations to prioritize beneficial interventions and provide holistic care while avoiding overburdening the medical system.
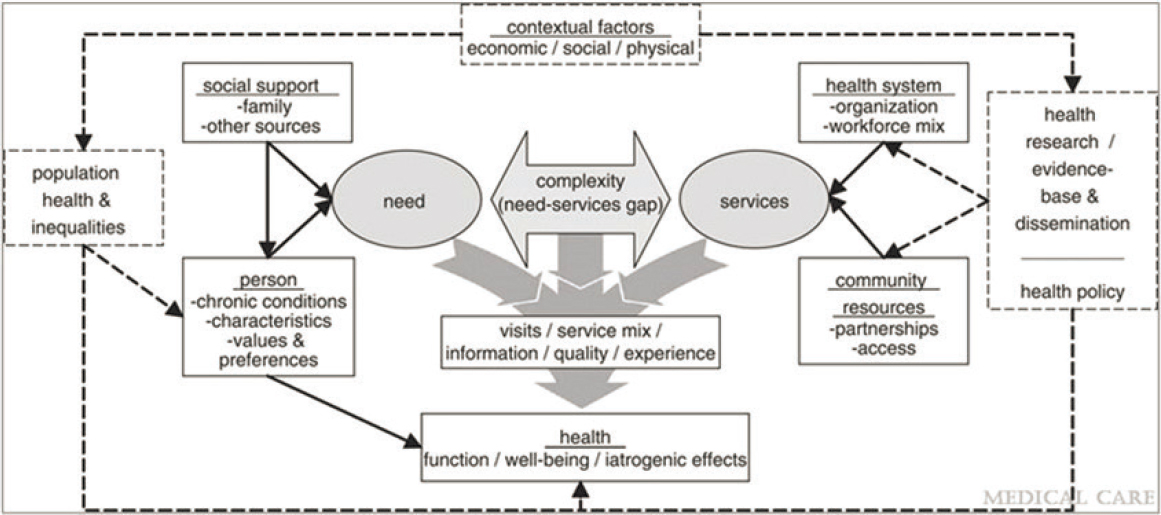
SOURCES: Grembowski et al., 2014; Adapted version presented by Karen Hirschman, University of Pennsylvania, May 9, 2023.
ELEMENTS FOR DISCHARGE PLANNING AND TRANSITIONAL CARE
Tolu Oyesanya, associate professor, Duke University School of Nursing, emphasized that over 6 million U.S. residents are living with TBI-related disabilities and contend with physical, cognitive, communication, behavioral, and/or emotional impairments. These challenges—which vary by individual according to factors including severity of the injury, time since injury, and age—can have substantial effects on TBI survivors and their families. As previously noted, less than half of people who sustain a mild TBI receive care; many of those who do seek treatment visit the ED and are discharged without hospital admission. Thus, the majority of mild TBI management occurs outside of the hospital via community-based primary and specialty care providers (Holm et al., 2005; Silverberg et al., 2020). The follow-up care a person may receive varies and is complicated by care continuity gaps and a limited number of providers with TBI expertise. She asserted that many providers treating patients with TBI do not have expertise in caring for this patient population.
Upon discharge, Oyesanya said, TBI patients and their families face a number of potential issues in self and family management of injury-induced impairments (Oyesanya et al., 2021a,b). Safety issues can arise when patients do not adhere to post-TBI activity restrictions or when they engage in unsafe behaviors attributable to TBI-caused impairments affecting judgment, decision making, and impulsivity. Medication management is often challenging for TBI patients and their families, who may have difficulty remembering to fill, pick up, or take medications appropriately. Impairments can make it difficult for patients to develop strategies for these activities in both the short and long term. Challenges in goal setting or adherence to plans are common for TBI survivors and can affect one’s ability to return to preinjury levels of activity at work, school, leisure, and exercise. Survivors may also face issues managing emotions, comorbidities, and disabilities. Some TBI patients experience depression, anxiety, frustration, and mood swings.
TBI can complicate the management of other conditions (e.g., diabetes, sleep apnea) and can exacerbate disorders such as attention-deficit/hyperactivity disorder and dyslexia. When patients have limited support in coping with TBI-related impairments, their quality of life can decrease and they may have substantial problems navigating their health and health care, including following up with providers of primary and specialty care as directed, adhering to care providers’ instructions, communicating with providers and retaining the information they offer, coordinating care, and accessing health care services and community-based resources postdischarge. She noted that TBI patients have expressed an overall desire
for more support from interdisciplinary providers during their recovery process.
Social determinants of health can affect health care transitions and influence well-documented disparities in TBI outcomes linked to race, ethnicity, sex, and age, Oyesanya noted. Care plans need to consider factors related to social determinants of health, she said—defined as “the conditions and the environment where people are born, live, learn, work, play, worship, and age that affect a wide range of health, functioning, and quality of life outcomes and risks”—including economics, education, health care, housing, and social supports (HHS, 2020). As described by Oyesanya, economic stability includes personal finances, health insurance status, housing, and food security, and it can influence an individual’s ability to adhere to care recommendations. Education access and quality can affect a patient’s health literacy, meaning the degree to which they can find and understand health-related information and apply this to decisions about their care. Health care access and quality involve the proximity of high-quality providers, health system resources, and any language barriers that might affect a patient’s ability to communicate with providers. Neighborhoods and built environments can promote or challenge an individual’s health and safety, while social and community contexts determine access to community-based resources and support from family and friends.
Transitional care models can address many TBI-related challenges by ensuring coordination and continuity of care as patients transfer between settings and levels of care, said Oyesanya (see Box 3-1). Oyesanya noted that in contrast to other conditions, such as stroke and heart failure, few TBI-specific transitional care programs have been established, perhaps owing to the lack of TBI-specific transitional care standards in the United States. She is currently involved in developing one such program, the Brain Injury Education, Training, and Therapy to Enhance Recovery (BETTER) TBI transitional care program for patients discharged directly from acute hospital care to home without inpatient rehabilitation (Oyesanya et al., 2022).
EXAMPLES OF FOLLOW-UP CARE MODELS AFTER MILD TBI
Hospital for Special Surgery Concussion Clinic Model
Teena Shetty, neurologist and director of the Concussion Program in Neurology, Hospital for Special Surgery (HSS), New York, outlined evidence indicating that patients who suffer significant symptoms from TBI benefit from care provided by multidisciplinary clinics. This comprehensive care requires teamwork, which has been shown to improve effectiveness in the health care field across disciplines (Schmutz et al., 2019). Team-based
care models improve patient outcomes and are associated with safer and higher-quality care (Jesmin et al., 2012; Rosen et al., 2018). Advantages of such models include quick verbal communication and situational awareness that streamline and improve care (Lim et al., 2021). Given the nuanced, heterogeneous, and individualized symptoms after concussion/mild TBI, high-quality care requires expertise and coordination among multiple providers (Kontos et al., 2019). The prevalence of both sports- and non-sports-related concussions calls for services for both populations that include education and management plans to effectively treat symptoms (Chang et al., 2011; Kutcher and Giza, 2014). The HSS multidisciplinary clinic model centralizes services, thereby maximizing efficiency of workflow and improving care coordination for patients, she reported.
Shetty founded the HSS Concussion Program in 2015 to define a new standard of care and influence the way that providers diagnose, treat, and
understand concussion.1 It is an active recovery program that strives for short latency after ED discharge or referral from an athletic trainer, sport coach, school, or other source. In this way, she said, HSS functions similarly to an urgent care model despite being a tertiary care outpatient setting. The model of care uses the latest research to inform diagnosis and early interventions. Developing individualized concussion management plans, the team considers baseline level of function and targets each patient’s goals. The program simultaneously offers patients access to experts with years of specialized training in concussion care. Moreover, the HSS Concussion Program model features a patient navigation component that allows providers to address the increasing complexity of TBI care. The program’s goal is to improve the patient’s experience by enhancing the coordination of visits, eliminating barriers to care, and offering timely service delivery. Weekly comprehensive team meetings serve as a mechanism for presenting patient cases and aligning multidisciplinary providers on cohesive, integrated care plans developed via roundtable contributions from all team members.
Concussion Care Team Roles
Shetty reported that the team features a neurologist, multiple physical therapists, sports performance trainers, a neuropsychologist, and a clinic coordinator/social worker. As a neurologist, Shetty serves as the point person of the HSS care team by developing targeted treatment plans, guiding modifications of vestibular and athletic training progressions for each patient, directing weekly care meetings, and helping the team determine decisions regarding the return to work, school, and play. Additionally, the neurologist performs comprehensive neurological evaluations to triage each patient to appropriate multidisciplinary providers and expedite care. The advanced practice provider is a physician assistant, nurse practitioner, or registered nurse who (1) oversees return-to-work/return-to-play paperwork; (2) updates clinical notes with outside consults, imaging, and medical documentation; (3) fields patient phone calls; and (4) triages incoming communications. Shetty reported that having an advanced practice provider on the team increases patient flow, assists the program in its goal of offering timely appointments, improves patient satisfaction, and likely improves multidisciplinary clinic provider satisfaction as well.
The clinic coordinator establishes relationships with patients and assists them with scheduling appointments, relaying their questions to the appropriate care team member, reviewing next steps, making referrals to other providers, and providing letters for schools and workplaces. Shetty noted
___________________
1 More information about the Concussion Program at Hospital for Special Surgery is available at https://www.hss.edu/neurology-concussion-program.asp (accessed June 22, 2023).
that a nonrevenue earning physician fills this role, and budgeting for a physician who does not perform procedures or exams can be challenging. However, HSS staffs this position because of the clinic coordinator’s ability to increase patient compliance with the treatment plan. Because confusion is often present in the early stages of TBI recovery, the clinic coordinator ensures that patients understand all steps in their treatment plans. A research coordinator works with the neurologist to identify potential candidates for ongoing research, assists in educational outreach, and ensures patient compliance with the research protocol window. Arguably an optional part of the program, Shetty contended that the coordinator position is critical for scientific advancement in concussion treatment and diagnosis.
Given that visual abnormalities can occur in concussion and necessitate visual rehabilitation, the HSS Concussion Program works closely with a neuro-ophthalmologist, noted Shetty. A neuropsychologist evaluates whether the TBI has caused any cognitive deficits. In cases where deficits in attention, processing, working memory, or other areas of cognition are identified, the neuropsychologist uses cognitive metrics to guide the recovery process and determines when the patient’s functioning has returned to baseline. Vestibular dysfunction is common in concussion, and a vestibular therapist works with patients to address dizziness, fogginess, nausea, and environmental sensitivity.
A physical therapist specializing in concussion provides neck physical therapy (PT) to patients experiencing whiplash symptoms or cervical pain or stiffness. Neck strengthening exercises have been found to improve concussion recovery and may even help to prevent TBI (Streifer et al., 2019). An athletic trainer identifies symptoms that are triggered by exercise and develops active exercise protocols individualized to patient goals, whether competitive or noncompetitive. Throughout a gradual progression of increasing exercise intensity, the athletic trainer assesses the patient, monitors patient heart rate, and provides feedback to the team until the patient is asymptomatic to maximum exertion. Return-to-play decisions rely on this feedback, and aerobic exercise can accelerate recovery and reduce prolonged symptoms, said Shetty.
The HSS Concussion Care Team does not currently include cognitive behavioral therapy (CBT) or cognitive remediation components, but Shetty stated her hope that these will be added in the future once resources can be allocated to provide these services. CBT may help facilitate recovery for mild TBI patients experiencing insomnia, depression, anxiety, psychosomatic symptoms, and headache (Al Sayegh et al., 2010). In addition, Shetty noted that CBT may help patients develop after-recovery plans. Cognitive remediation is a targeted psychotherapy, attention, and information processing exercise that may also improve postconcussion functioning.
Patient Outcomes
The HSS Concussion Care Team is working to improve outcome measurement, Shetty noted. Currently, each patient completes a postcare evaluation that is shared with the team during weekly meetings and translated into future action items. Patient recovery is measured in terms of progression toward patient-defined goals and by team member assessment. Team members can incorporate one another into the treatment plan via referrals, and the program guarantees PT appointments for each patient. The program features a “one-stop shopping model” in which the rehabilitation offices are downstairs from the neurology department, enabling patients to conveniently attend neurology appointments and PT/rehabilitation appointments in the same building. This proximity facilitates feedback between the departments about patient progress. The team works to prevent attrition and ensure compliance by addressing any barriers patients may be experiencing. Additionally, active recovery plans establish timelines for goals, and when dates are not met, the team works to identify potential barriers to goal achievement.
Next Steps
The HSS Concussion Program is also working to improve patient education and care supported by cognitive-based neuroscience, said Shetty. This involves educating patients about the sympathetic versus parasympathetic nervous system and the concept of graded exposure to activities patients may be avoiding because of predictions that they will cause pain. The team trains patients on breathing and mindfulness exercises, meditation, and using heart rate variability biofeedback to improve symptoms. HSS plans to use telehealth technology to expand care to parts of the country lacking access to multidisciplinary clinics. The team also intends to explore remote monitoring of wearable technology to aid in exercise rehabilitation.
University of Texas Southwest Medical Center Multidisciplinary Clinics
Surendra Barshikar, associate professor and vice chair of clinical operations, Department of Physical Medicine and Rehabilitation, University of Texas at Southwestern (UTSW) Medical Center, provided an overview of the parallel concussion care programs that UTSW operates at its university hospital and at Parkland Memorial Hospital, a county facility housing one of the busiest trauma centers in the nation. Before the establishment of these programs, concussion care was fragmented across various clinics and departments—such as neurosurgery, rehabilitation medicine, neurology, and psychology—operating independently and without coordination or
centralized referrals. A model system was in place for moderate to severe TBI, but not every TBI patient met the criteria for this care pathway. In 2015, the UTSW multidisciplinary concussion programs were created in concert with a standardized TBI referral process that allows self-referrals. Most of the concussion clinics in the area focus on sports injuries and provide brief assessments and return-to-play documentation; these clinics refer patients who require ongoing care to UTSW. Housed within the Peter O’Donnell Jr. Brain Institute,2 the Parkland program requires in-house referrals and has substantial exclusion criteria that limit eligibility to complicated mild, moderate, or severe TBI or noncomplicated TBI that failed primary care management. The volume of clients seen at this clinic has created long wait times for appointments, he said.
The UTSW Concussion Program located in the university health system features eight brain injury-certified physiatrists; a brain injury fellow; three neuropsychologists; two rehabilitation counselors; providers of vestibular, neck, and spine PT; an occupational therapist who performs vision therapy; a speech language pathologist who provides cognitive therapies and remediation; and a social worker.3 Although it is not a revenue-generating position, said Barshikar, the social worker adds value by providing care coordination, patient navigation, accommodation letters for school and work, and various other forms of assistance to help patients return to their preinjury activities and lifestyle. These in-house providers refer to other UTSW specialists as needed, including the headache clinic, neuro-otology, neuro-ophthalmology, and psychiatry and psychology in cases warranting in-depth counseling or medication management.
Changes in Concussion Program Model
The initial model used at the UTSW Concussion Program’s inception was based on the theory that the timing of concussion care changes the outcome, with prompt care leading to better outcomes, Barshikar noted. The clinic prioritized patients whose TBIs had occurred within the previous month, scheduling their appointments with a physiatrist within 1 week of referral. These appointments focused on patient education and acute symptom management. Patients who had been injured 1–3 months prior to referral were seen by a physiatrist within 2 weeks. The team expected TBI psychosocial symptoms to be more common after 3 months postinjury. Therefore, individuals who were referred more than 3 months postinjury were scheduled for
___________________
2 More information about the Peter O’Donnell Jr. Brain Institute is available at https://www.utsouthwestern.edu/research/brain-injury/about (accessed June 22, 2023).
3 More information about the UTSW Concussion Program is available at https://utswmed.org/locations/aston/uh-pmr-clinic-concussion-program (accessed June 22, 2023).
a combined visit with a physiatrist and a neuropsychologist, who performed a brief neurobehavioral assessment. Unexpectedly, a majority of patients were referred to the clinic 3 or more months postinjury, largely because of delays related to insurance issues or navigating the medical system. With only three neuropsychologists, the clinic lacked the capacity to carry out the initial service model.
Such challenges are reflected in the clinic’s current operations, Barshikar noted. Presently, the hospital ED provides information about the clinic to TBI patients but makes automatic referrals to primary care providers. These providers may, in turn, refer these patients to the clinic, while some patients self-refer using the contact information they received in the ED. Patients with acute symptoms are generally seen within 2 weeks of referral, but other patients face longer wait times, and the wait time to see a neuropsychologist is long. The team holds biweekly meetings to discuss new patients, identify barriers to progress for existing patients, and generate potential solutions to improve outcomes. Formal outcome tracking is not yet standardized; currently, the team assesses whether the patient is better, worse, or the same at clinic discharge than at their first clinic appointment, and these data are kept in a registry of all patients.
Current Challenges
Wait times at the Parkland TBI clinic tend to exceed those at the university facility, with new patient appointments for mild TBI typically scheduled 6 months in advance, said Barshikar. This clinic has a smaller staff of two physiatrists, physical therapists, and a speech language pathologist. All other services must be referred out, and the clinic lacks a care coordinator. Emphasizing that delayed presentation for care is associated with poorer outcomes, he stated that the care patients receive at some so-called community concussion clinics does not meet standard of care and can delay patients receiving comprehensive treatment. For example, the UTSW program has treated patients who visited four or five small concussion clinics at the prodding of their attorneys before coming to the UTSW clinics. However, Barshikar noted that the UTSW clinics do not have capacity to fully meet the current need, particularly at the Parkland clinic, given its lack of neuropsychology services and the exclusion criteria in effect for services. As a result, patient access to quality care and education remains a substantial challenge. In addition, he noted that the COVID-19 pandemic generated a shift in demand for elective medical care that has presented additional demands on UTSW resources. Demand during the pandemic initially declined and in 2020, the volume of patients served at the UTSW TBI clinic decreased by 58 percent, down from 205 patients treated in 2019 to only 86. However, patients now contending with long-COVID—symptoms that continue or develop after the initial
COVID-19 infection—require many of the same components of care as TBI patients, presenting new capacity challenges from competition for limited care resources between these two patient populations.
Froedtert Hospital-Medical College of Wisconsin Brain Injury Program
Michael McCrea, Medical College of Wisconsin (MCW), introduced the Brain Injury Program established by the Froedtert Hospital and MCW almost three decades ago.4 Reflective of national averages, TBI causes approximately 1,500 deaths annually in Wisconsin, in addition to more than 12,000 ED visits and 4,000 hospitalizations each year.5 The statewide rate of TBI among older patients has increased, primarily because of falls. However, the number of older, active patients being treated at the Brain Injury Program caused by injuries while biking, skiing, or other physical activities has also increased over the past 20 years. Adolescents make up the majority of ED visits for TBI, many of which involve vehicle crashes and/or alcohol consumption. McCrea added that these statistics include state-reportable events and do not capture all TBIs treated in ambulatory care settings or those that go untreated.
Froedtert-MCW provides a full continuum of neurotrauma care, including a Level 1 trauma center, a neurointensive care unit, an inpatient neurology unit, and a dedicated rehabilitation hospital featuring a specified inpatient accredited TBI program, said McCrea. The health system treats over 3,000 patients with head injuries each year in ED and urgent care visits. Approximately 15 years ago, the facility created separate, dedicated clinics for sport-related mild TBI and civilian or community-acquired TBI. The majority of referrals to the civilian clinic come from the ED, trauma service, and inpatient rehabilitation. The clinic strives to see patients within 2 weeks of discharge, during the acute or subacute recovery phase. Exclusion criteria extends to patients who are 2 or more years postinjury.
Featuring an interdisciplinary care model, the clinic provides physical medicine and rehabilitation (PM&R), neurosurgery, neuropsychology, primary care, and rehabilitation services. Patients in need of services not provided in-house—such as physical, speech, psychology, and occupational therapies—receive fast-track referrals to providers with whom the clinic has established relationships. A focus on restoring function and maximizing mobility guides the clinic’s practices.
___________________
4 More information about the Medical College of Wisconsin Brain Injury Program is available at https://www.mcw.edu/departments/neurosurgery/patient-care/adult-programs-and-specialties/brain-injury (accessed June 22, 2023).
5 More information about TBI burden in Wisconsin is available at https://www.dhs.wisconsin.gov/wish/injury/index.htm (accessed June 20, 2023).
McCrea highlighted that patient diversity in the clinic offers medical residents and fellows valuable learning opportunities in TBI care. For instance, within the same day a resident may see a patient experiencing a remarkable recovery despite a Glasgow Coma Scale (GCS) score of 4 at admission and a patient with a GCS of 15 who is struggling and unable to return to work.6 Such experiences demonstrate that recovery outcomes cannot be accurately predicted by GCS scores alone, he emphasized.
Remodeling Initiative
Historically, the multidisciplinary clinic has treated 14–16 patients per day, 2–3 days per week. Despite this high throughput, multiple pressures including the COVID-19 pandemic and physical relocation of the clinic led McCrea and his colleagues to question whether they could improve access and the patient-centered aspect of services. This led to efforts to remodel the program, which began with the assemblage of the Froedtert-MCW Post-Acute TBI Clinic Working Group, which contains representatives from neurosurgery, neurology, neuropsychology, PM&R, and service line administrators. The working group set goals of enhancing the best-practice system of care for postacute TBI and concussion and of achieving national recognition for a model of TBI care. Accepting patients from multiple points of entry—including ED, urgent care, physician offices, inpatient care, and self-referrals—necessitates a nuanced approach. A model that refers every ED discharge to a multidisciplinary clinic is not sustainable, McCrea noted, but data systems and automation can facilitate a high-volume triage process by identifying key metrics for efficacy. A patient’s primary clinical phenotype will affect the interventions from which they are most likely to derive benefit, McCrea added. For instance, a patient experiencing persistent vestibular symptoms, but no psychological health challenges, will likely receive more benefit from physical therapy than from cognitive behavioral therapy. In contrast, a patient with normal cognitive functioning who is experiencing post-traumatic stress disorder symptoms requires CBT.
A revised TBI care model revolves around a common point of entry, said McCrea. The majority of TBI patients who are later treated at a multidisciplinary clinic are first seen in an ED. However, provision of ED discharge instructions tends to be inconsistent. To increase subsequent connectivity with TBI patients initially seen in the ED, the Froedtert-MCW program is beginning to use an automated follow-up system to inform the TBI care team and to provide individuals with tips to facilitate recovery.
___________________
6 The Glasgow Coma Scale (GCS) rates eye, verbal, and motor response. GCS scores from 3–8 constitute severe injuries, scores 9–12 are considered moderate, and scores 13–15 are assessed as mild.
Interactive Online Symptom Tracking Tool
Numerous departments within the Froedtert-MCW health system use the GetWell Loop app to connect to patients. McCrea noted that the TBI team’s adoption of any app was contingent on its capability to link to the health system’s electronic health records system. The GetWell Loop has this capability and enables symptom tracking and patient education on recovery facilitation and indicators that multidisciplinary follow-up care is warranted. On days 4, 9, 14, and 28 postinjury, the interactive tool guides patients through brief sets of questions that results in a blue alert in the event of recovery and full resolution of symptoms or a yellow alert in the event that symptoms are problematic or worsening. These alerts are sent to a TBI care team registered nurse (RN) who manages incoming GetWell Loop data. The members of the TBI care team use these data to determine which patients are experiencing persistent symptoms and their predominant clinical phenotypes, which in turn informs care plans and referrals.
Multidisciplinary Care Plans
At 4 weeks postinjury, described McCrea, a multidisciplinary board of brain injury medicine providers reviews patient data gleaned from the RN and the GetWell Loop app and to determine appropriate care plans. The team’s patient-centered treatment features various care tracks to meet different needs. A “physician-only” track is designed for patients whose needs can be met by a PM&R provider. Other patients require care from both the PM&R physician and the neuropsychologist. A patient’s primary symptom profile may warrant referrals to CBT, PT, occupational therapy (OT), and/or speech services. The team works to provide each patient with the specific care they need to have the best chance at full recovery, restoration of function, and a return to normal life activities.
DISCUSSION
Javier Cárdenas, professor and chief, Division of Sports Neurology, Rockefeller Neuroscience Institute at West Virginia University, moderated the discussion and asked about the role of non-revenue-generating positions on multidisciplinary TBI teams. Subsequent topics arose in response to comments and questions from participants.
Non-Revenue-Generating Positions
Cárdenas noted that non-revenue-generating staff positions, such as care coordinators, can support effective program functioning but asked
about the challenge of justifying their value since such roles do not directly generate institutional revenue. Shetty replied that funding these fundamental positions is a continual challenge. In addition to philanthropy, she uses program funds for this purpose with the justification that these positions result in downstream revenue. Every new patient appointment at the clinic results in multiple referrals, ranging from radiology to vestibular therapy to PT and OT. Barshikar remarked that his team has approached funding these positions as a mechanism for addressing physician well-being and burnout, noting that care coordination, accommodations and return-to-work documentation, and paperwork required for short-term and long-term disability insurance are time consuming. Removing these tasks from providers’ workloads enables them to spend more time on direct patient care, he noted. Patients report on the usefulness of being able to contact the clinic social worker. Emphasizing the benefits that non-revenue-generating positions add to the clinic, Barshikar acknowledged that many settings focus on reimbursement and can be unwilling to fund ancillary positions.
McCrea stated that his program uses metrics such as reductions in hospital readmissions and return ED visits to demonstrate how non-revenue-generating positions add value. Philanthropy funds some of the cost of these positions. Acknowledging that multidisciplinary care is expensive, he highlighted an inherent, growing conflict between what health systems want and what patients indicate they want. McCrea questioned whether a model that is economically profitable but inconsistent with what patients want and need fulfills the mission of providing good health care. The challenge of building a world-class, best-practice, inpatient or ambulatory TBI program that is economically viable requires constant consideration.
TBI Center Accreditation Designation
Ramon Diaz-Arrastia, University of Pennsylvania, remarked that 25 years ago the stroke field faced similar challenges in funding comprehensive stroke care. Stroke can cause long-term debilitation, and comprehensive postacute care was prohibitively expensive. This challenge shifted with the development of accredited comprehensive stroke centers, which generated competition among hospitals and fueled investment in attaining The Joint Commission’s stroke center designation.7 In turn, this led to a stronger negotiation position with insurance companies. When substantial resources were invested in multidisciplinary stroke care systems, insurance coverage expanded to include these centers. Diaz-Arrastia contended that the estab-
___________________
7 For further information on Joint Commission stroke certification programs, see https://www.jointcommission.org/what-we-offer/certification/certifications-by-setting/hospital-certifications/stroke-certification (accessed June 20, 2023).
lishment of designated or accredited TBI centers could similarly result in increased health care quality and hospital competition and investment.
Oyesanya noted a severe deficit in currently available follow-up care pathways for TBI. Services across a treatment continuum are needed to improve TBI outcomes, and these outcomes have wider implications for families and businesses, she said. The creation of a TBI center designation could encourage the expanded availability of needed comprehensive services. Hirschman commented on the apparent disconnection McCrea noted between what health systems value in TBI care and what patients and family caregivers feel is important. Policy changes can shift the metrics used to evaluate services, which in turn can influence investment decisions. Barshikar contended that consensus remains lacking on eligibility criteria for TBI services, thus such criteria need to be defined before the pursuit of accreditation designations.
David Okonkwo, University of Pittsburgh, maintained that the diagnosis-related group (DRG) classification for care compensation was a critical driver of the profitability of designated stroke centers. Attaining the status of designated stroke center creates a spillover effect, as the ability to treat acute stroke suggests the capacity to treat other conditions. The combination of center accreditation and DRG assignment to the episode of care creates an economic model that supports comprehensive care, he said.
Informing Care Plans with Phenotypic Data
Kathy Lee, Department of Defense, asked how phenotypic data from patients are translated into multidisciplinary models of care. McCrea noted that the data the GetWell Loop app collects between days 14 and 28 postinjury move beyond symptom tracking to the characterization of primary domains of symptoms, such as vestibular, cognitive, psychological, or headache or other somatic symptoms. In addition to indicating their symptoms and the effects these have on functioning, patients are asked to rate their top three areas of difficulty. The Froedtert-MCW TBI board uses these data to determine appropriate services and then uses their network of referral outlets to facilitate quick access to PT, OT, CBT, and other therapies. Acknowledging that these data are not as extensive as those provided by a detailed neuropsychological or multidisciplinary evaluation, McCrea remarked that the app enables high throughput and high volume in the early postinjury phase. He highlighted the variance in the needs of TBI patients; not all TBI survivors require extensive multidisciplinary care, nor do all those who need specialty care require every modality of therapy. Shetty added that the HSS Concussion Program uses an informal algorithm for patient risk stratification, and providers evaluate this information on a weekly basis through longitudinal visits to ensure that patients are triaged
appropriately. Similar to the GetWell Loop app, this process involves asking patients to rate their primary complaints. She highlighted the need for a more standardized process of determining TBI recovery phenotype.
TBI Program Sustainability
A participant asked about the role of economic analysis and standardized outcome datasets in program sustainability. Barshikar replied that UTSW has recently completed a quality improvement data collection project for the purpose of developing standardized datasets. Currently, the center is using an online survey to collect standardized data elements on all TBI patients, in addition to the data collected during patient intake. These efforts generate copious data, but given the numerous factors that can affect TBI outcomes—including comorbidities—the team has not yet developed a clearly defined outcome measure. He remarked that Texas state policy bolsters the sustainability of the UTSW program via an insurance code that prohibits health benefit plans from denying coverage of treatment for brain injury. This enables the UTSW programs to provide rehabilitation and therapies beyond what is afforded by plans in some other states.
Computerized Cognitive Testing
Given the shortage of neuropsychologists, a participant asked about the use of electronic tools for cognitive testing. Noting decades of use of computerized neurocognitive testing in sports and military settings, McCrea stated that the reliability, validity, and sensitivity of this technology is still inconsistent. He added that computerized cognitive testing functions as a data collection tool. As is the case with other data collection tools such as radiologic imaging, effective use of computerized testing requires meaningful interpretation of data to inform diagnosis and treatment planning. Thus, cognitive testing tools can increase the throughput of a neuropsychologist, but they do not replace the need for a provider who can interpret these findings and oversee treatment administration.
Common Data Elements
Noting his prior participation in the National Institute of Neurological Disorders and Stroke (NINDS) Common Data Elements initiative,8 James Kelly, professor of neurology, University of Colorado, asked about the usefulness of combining patient-reported outcomes with data from diagnostic
___________________
8 More information about the Common Data Elements initiative is available at https://www.commondataelements.ninds.nih.gov/Traumatic%20Brain%20Injury (accessed June 22, 2023).
and prognostic assessments, perhaps from the Federal Interagency TBI Research (FITBIR) informatics system. Okonkwo explained that the initial funding for the Transforming Research and Clinical Knowledge in TBI study (known as TRACK-TBI) specified implementation of the TBI common data elements into research practice. At that point, FITBIR became a designated repository for federally funded TBI research, and federal grants stipulate that data must be submitted into FITBIR. The adoption of this concept into the clinical realm could enable the creation of a common language and drive advancements in the field. For example, consensus about molecular signatures of TBI and the terminology used to define this condition could enhance commonality in clinical designation and, in turn, could create more effective clinical care pathways.
Geoffrey Manley, University of California San Francisco, described the common data elements in FITBIR as iterative, noting the system is currently on a 3.0 version. Numbering at over 9,000, the common data elements must be pared down in order to identify those most useful for the clinical arena and for routine research. Standardization also enables improved demonstration of outcomes, and while the research required to develop standardization is expensive, so too are ED revisits, he contended. In parallel, health economics research can help determine the cost of hospital readmissions and ED revisits after TBI, which can then be used to justify the expense of routine TBI follow-up care. He drew a parallel to diabetes, which is expensive to manage, yet disease management reduces the long-term care costs over time. McCrea added that MCW has rebuilt its TBI clinic database to use common data elements for front-end demographics, acute injury characteristics, and outcome measures.
Early Steps in Establishing a Multidisciplinary TBI Clinic
Cárdenas asked about the components required in the initial stages of opening a multidisciplinary TBI clinic that could translate to other parts of the country lacking these services. Shetty replied that she began her program by networking with local schools, athletic trainers, coaches, athletic organizations, and other community groups. Giving talks about sports injury and TBI, she spread awareness about the need for care, and this awareness fostered the growth of the HSS Concussion Program. Barshikar emphasized the importance of connecting silos in TBI care and noted that the further development of standardization and outcome measures could support defragmentation efforts. Additionally, knowledge regarding moderate and severe TBI can be applied to injuries classified as mild. His clinic was part of a model system that was tracking outcomes for moderate and severe TBI, and he and his colleagues were able to extend the services in place for more severe cases to mild injuries. McCrea spotlighted the role
of TBI care leaders at MCW who helped champion the need for systematic follow-up of patients discharged from the hospital and applied their expertise to meeting this need.



















