Fed Up!: Winning the War Against Childhood Obesity (2005)
Chapter: 5 Off the Couch and Away from the Screen
CHAPTER 5
Off the Couch and Away from the Screen
It’s time for Nancy Driscoll’s second-grade class to study language arts. Like second-graders in many U.S. schools, they are learning about synonyms and antonyms: words with similar meanings and with opposite meanings. But unlike kids in most other elementary schools, these students are not about to take their lesson sitting down. “Stand by your desks,” Driscoll orders the children. “If I say two words and they’re synonyms, jump and clap five times. If I say two words that are antonyms, do five lunges.” And if the words are homonyms—sounding the same but with different meanings—the students are instructed to touch their toes five times.
The children stand by their desks as the lesson begins. While the teacher calls out each pair of words, the kids rhythmically punch the air five times. Next, they snap their fingers five times in unison to mark their “think time” before jumping, lunging, or touching toes.
“Friend, enemy,” Driscoll calls out. Punch. Snap. Lunge.
“Sick, ill.” Punch. Snap. Everybody jumps and claps.
“Dear, deer.” Punch. Snap. Up and down the students bob, fingers stretching to toes.
The words keep coming and the kids keep moving, literally thinking on their feet as they figure out how to respond to each pair. The task requires concentration, and there’s no talking or laughing, just the steady beat of 15 second-graders jumping, clapping, or bouncing up and down.
After several minutes of this drill, Driscoll rewards them by picking each child in turn to choose and lead an exercise. Now the kids giggle as they follow the leader, twisting, pretending to jump rope, or briefly dropping to the floor to do push-ups. When they’ve been moving around for a total of 10 minutes, it’s back to their seats. Smiling and energized now, they’re ready for whatever Driscoll does next.
These students at Brookridge Elementary, part of the Shawnee Mission School District in suburban Kansas City, Kansas, are participating in an innovative three-year experiment, involving several thousand Kansas elementary school children, aimed at finding out whether building physical activity into academic lessons during the school day can help prevent children from becoming overweight. The Kansas project reflects a growing consensus among researchers and health experts that in order to turn back the childhood obesity epidemic, Americans will have to do more than just make sure their kids are taking a gym class. They will also have to find creative new ways to build more physical activity into their children’s daily routines—and into their own.
Efforts to reduce obesity levels by ramping up school physical education programs have so far failed. Even when students are given intensified P.E. classes, most studies have found that they do not get enough minutes per week of exercise during P.E. to make an impact. And around the nation, physical education time and even recess breaks are increasingly casualties of the pervasive pressure on schools to pack more academic lessons and test preparation into students’ days. Yet educators are beginning to acknowledge that schools must do their part in fighting the growing problem of childhood obesity.
That’s why University of Kansas researchers, with federal funding from the National Institutes of Health, embarked in the fall of 2003 on
a program called Physical Activity Across the Curriculum, or PAAC. Their hope is that PAAC will accomplish dual goals: prove it’s possible for classroom teachers to get kids moving and to help protect them from becoming overweight, and show that children’s activity levels can be increased during the school day without cutting into academic time. Unlike some previous programs, PAAC is specifically designed not to require teachers to schedule “exercise breaks” that are separate from instruction. “If it’s three minutes here and three minutes there, that’s fine,” says Janet May, PAAC project coordinator for Kansas City schools during the program’s first year. “We want them to incorporate it into learning.”
Researchers caution that it is still too soon to say whether such an approach can succeed, but if PAAC is effective, its concepts could ultimately influence the methods of teachers nationwide. In time PAAC and other programs like it could lead to a shift in classroom routines that makes learning a more physically active process. “The key concept here is that there is no loss of academic instruction time,” explains Joseph E. Donnelly, a professor of exercise science at the University of Kansas who is leading the project. “You take your existing lesson and instead of talking your way through it, you move your way through it.”
Teachers at the PAAC schools in the Kansas City area and in Topeka receive training and support, including myriad suggestions in a manual and on a Web site, for including physical activity in lessons about any subject—math, social studies, language arts, science. Janet May says much of the training is designed to help teachers realize how easy it is to do so, especially for students in the early elementary grades. “The best ideas come right from the teacher,” she notes.
At Briarwood Elementary, another PAAC school in the Shawnee Mission district, Susan Reichardt’s third-grade class has been studying the human body. “I want you to get up, push in your chair, and make your blood pump faster,” says Reichardt. Some students start doing jumping jacks, others jump up and down or run in place.
“Now move a hinge joint,” she orders. They flex their elbows.
“Move a ball joint.” They swing their arms around.
“Now do a pivot on a pivot joint.” They swivel their hips, pretending to swing a bat.
Incorporating activity becomes a greater challenge in the upper elementary grades, when students must master more complex subject matter, but teachers participating in PAAC are finding ways to do it. In another Briarwood classroom, Marsha Plese is teaching her fifth-graders how to form the possessive of plural nouns. She calls a student named Anna to the front of the class to demonstrate what she wants. To act out an apostrophe, Anna does a side stretch. To make an “s,” she does a deep knee bend. Plese explains to her class that plural nouns ending in “s,” like “doctors,” need only an apostrophe to make the possessive form: “doctors’.” But some other plural nouns, like “men,” require both an apostrophe and an “s”: “men’s.” As she calls out various words, her students act out the answers.
Teachers in the PAAC program are asked to include 100 minutes of physical activity each week in their academic lessons, deciding for themselves how to apportion the minutes. The project has enrolled 24 Kansas elementary schools, of which 14 are “intervention” schools (incorporating physical activity into lessons) and 10 are “control” schools (following their usual educational programs and serving as a comparison). Donnelly observes that school principals were not drawn to the program because of its potential health benefits. Researchers found that the most effective way to promote PAAC to school officials was by providing evidence that physical activity could improve academic performance, appeal to diverse learning styles, and make children calmer and more manageable. “We got nowhere when our rap was all about diabetes and obesity,” Donnelly recalls. “Everybody said, ‘That’s important, but what does it have to do with us?’”
In all of the schools, second- and third-graders were weighed and measured at the start of the program, and their BMIs were recorded. A subset of students in these grades have also undergone more detailed testing, including blood tests to measure levels of glucose, insulin, cholesterol, and other components, blood pressure testing, measurement of waist and hip circumference, measurement of skin-fold thicknesses to estimate fat stores, cognitive testing by psychologists, and a submaximal fitness test in which their heart rates are measured after they ride an exercise bicycle.
Throughout the program’s three-year life, observers will randomly
visit classrooms in intervention and control schools to assess students’ physical activity levels during the day. At the end of the study, all students will again have their BMIs measured to determine whether incorporating regular physical activity into lessons reduced obesity rates in the intervention schools. In addition, researchers will find out whether PAAC has an impact on students’ overall physical fitness, cognitive ability, blood pressure, cholesterol, or other health factors.
In a mobile clinic parked behind Prairie Elementary School, members of the PAAC research team are doing fitness tests on third-grade students. Assistant Greg McMillan buckles a heart-rate monitor around the chest of Jacob, a serious-looking boy whose T-shirt reads “Take me to your candy.” Greg asks him to start pedaling the exercise bike at a steady rate of 60 revolutions per minute. “We’ll do this for a couple of minutes to let your muscles warm up. Then I’m going to change the gear like you’re going up a steep hill.”
Jacob’s heart rate reaches 122 beats per minute, a healthy response to moderate exercise in a child his age, while he pedals the bike “on the flat.” Greg then adjusts the bike to increase resistance. “He’s fairly fit, so he gets a higher wattage,” he explains. “Keep those legs pumping, Jacob. You’ve got to get up this hill. Come on, Jacob, you can do it. You’re getting close to the top now.” When Jacob’s heart rate hits 171 beats per minute, the monitor beeps, signaling the end of the test. Greg dials down the resistance. Breathing hard, Jacob pedals slowly to cool down.
Donnelly and his team are uncertain whether the amount of classroom activity provided in PAAC will be sufficient to make children more physically fit, but they hope it will boost daily calorie expenditure enough to effect a measurable impact on obesity levels. Equally important, they hope that the program will produce a lasting change in students’ attitudes about activity that might, over time, change norms in the U.S. population as a whole. After participating in PAAC, “we hope that when somebody is 30, they will think that they can be physically active any time, any place,” Donnelly says.
![]()
America’s children urgently need to get moving. Current national recommendations issued by the Institute of Medicine and by the National
Association for Sports and Physical Education call for children to accumulate a minimum of 60 minutes of moderate to vigorous physical activity each day. Yet surveys suggest that most children and teenagers in the United States don’t come close to that level of activity. The lifestyle of most U.S. children today is far more sedentary than that of kids who grew up a few decades ago. The reasons are many and include sprawling suburbs that force dependence on cars; traffic and neighborhood conditions that make it difficult, dangerous, or impossible for many children to walk to school or to play outside; cutbacks in school physical education programs; work schedules that prevent many parents from being available to supervise after-school play; the lure of the passive entertainment provided by television, computers, and video games; the demands of homework and academic schedules; and the inadequacy of after-school sports and recreation programs.
Experts are unsure how much each of these factors contributes to children’s inactivity and to rising obesity rates. They concur, however, that finding ways to make kids more physically active should be a central part of the strategy for turning back the obesity epidemic. Human bodies store fat whenever the calories they take in exceed the calories they burn. To restore balance to that equation and to prevent weight gain, a child (or an adult) must either eat fewer calories, expend more energy in physical activity, or both.
But what is physical activity? Most people would probably say it’s exercise: playing a sport, working out, taking a physical education class. The true definition is far broader, encompassing everything children or adults do with their muscles from the moment they wake up in the morning until they go to sleep at night. It includes walking or biking to school, playing outside, walking the dog, doing household chores, playing on an after-school sports team, going swimming, climbing stairs, carrying a book-filled backpack, dancing around the living room, even fidgeting in class—as well as participating in sports or P.E. All of these activities burn calories and contribute to the dynamic balance between food intake and energy use that determines body weight.
Many experimental programs aimed at preventing or reducing obesity in children have focused on improving just one component of physical activity by offering longer and more vigorous P.E. classes at
school or after-school sessions of group exercise or dance. So far, testing indicates that making a sizeable populationwide difference in children’s activity levels—a difference substantial enough to help slow or stop the epidemic—will require changing more than just one component of what kids do. A concerted effort will probably be needed to offer children all kinds of opportunities and incentives to become more active, both in school and at home. Some research findings suggest that a key initial goal for many families might be reducing the time kids (and adults) spend watching TV, sitting at the computer, and playing video games each week and substituting other, more active ways to have fun.
Parents, teachers, child-care providers, youth group leaders, coaches, and others responsible for the welfare of children should be encouraged to think creatively about what children do during the day and about how those patterns can be tweaked to incorporate more movement. Kids can be part of that process, brainstorming to come up with ideas and incentives. At home the answers might include getting rid of a television set or putting kids on a TV allowance, signing up for a community soccer program, buying a push lawn mower, taking a dance class, giving children a larger share of household chores, leaving the family car in the garage on some mornings. Schools are increasingly being expected to participate in this effort. Some state governments have recently passed new laws requiring an increase in the number of minutes students spend weekly being physically active at school. Texas, for example, recently legislated 135 minutes of activity a week, a statewide policy change that has forced some classroom teachers to schedule and lead daily workouts.
Just as encouraging kids to develop healthy eating habits is a familywide endeavor, getting them to become more active also involves changing everyone’s behavior patterns. Steven Gortmaker of Harvard has been tracking the pediatric obesity epidemic since the 1980s, as well as designing innovative school- and community-based strategies to combat it. He believes that Americans’ current unhealthy eating habits and sedentary lifestyles have been promoted by powerful economic forces, including the food industry, advertising, the television and motion picture industries, and the makers of computers and video games.
Nevertheless he remains refreshingly optimistic about the chances of improving the outlook, especially for children. “The epidemic is driven by [the equivalent of] less than a can of soda a day,” he says. “It’s so rooted in everyday behaviors that when you take them one at a time, there’s nothing wrong with them.” Added together, however, those behaviors are making more and more children and adults overweight each year.
Getting kids to move more should be the easiest part of the solution, Gortmaker predicts. “The physical activity is the part of this that I think is going to be solved a lot quicker. Kids really enjoy playing and running around…. All we need to do is return to where we were about 25 years ago.”
![]()
Precise information doesn’t exist to quantify how active children are today compared with children a quarter-century ago. Recently researchers have begun using devices such as accelerometers and pedometers—electronic devices that can be worn on the body—to measure kids’ activity levels. But until the past decade or so, almost all information on exercise and physical activity was self-reported, by people answering questionnaires—and most of it was collected on adults, not children.
National surveys of U.S. adults suggest that in spite of being urged in recent years to get more exercise, most Americans have not boosted their activity levels much during the past two decades. Between 1986 and 1997, the proportion of U.S. adults who reported no leisure-time physical activity (essentially synonymous, in those surveys, with exercise) stayed roughly constant at around one-third. A more recent national survey, conducted in 2000, was worded differently from previous ones but found no significant change in the percentage of adults who said they were physically active in their leisure time. It reported that men were more likely to be physically active than women and that whites more often engaged in high levels of physical activity than African Americans or Hispanics. People with incomes below the poverty level were three times more likely to be inactive than those in the highest income group. The most highly educated Americans were the group most likely to engage in regular vigorous activity.
In 2001 government researchers tried for the first time to measure how much physical activity Americans did as they went through their daily lives and added those figures to the activity totals that people reported from deliberate exercise. Preliminary results show that even with the addition of routine daily activities like stair climbing or walking around, more than half of American adults get less than 30 minutes of moderate exercise per day. (“Moderate” means enough to raise the heart rate and cause a little sweating, such as brisk walking.) About one-quarter of participants said they did no moderate physical activity.
If so many U.S. adults are couch potatoes, we shouldn’t be surprised that our children appear to follow a similar pattern. Data comparing the daily activity levels of American kids with those of children in other countries were recently collected by Brigham Young University researchers, who distributed pedometers to a sample of about 2,000 schoolchildren in the United States, Sweden, and Australia. The kids, between 6 and 12 years old, wore the pedometers for four consecutive days so that the instruments could record their daily step totals. Youngsters were also weighed and measured. Researchers then calculated the average number of steps taken daily by participating children in each country.
Boys and girls from the United States were significantly less active and significantly heavier than those from the other two countries. The U.S. sample also showed a steeper increase in BMI with age than was seen in kids from Sweden or Australia. For example, average step counts for U.S. boys in the study ranged from 12,554 to 13,872, compared with average counts of 15,673 to 18,346 for the Swedish boys, the most active group. (The totals for Australian boys were intermediate.) One-third of the American boys in the study were classified as overweight, compared to about 16 percent of Swedish and Australian boys. The step counts for girls were lower than for boys, but the cross-country comparisons among girls revealed a similar pattern.
Judging by these step counts, American elementary school kids are considerably more active than American grownups: a recent survey found that U.S. adults average about 5,310 steps per day. Yet many children undoubtedly fail to meet even minimal recommendations on physical activity. A 1996 report of the U.S. Surgeon General recom-
mends that all Americans over the age of 2 should get “at least 30 minutes of endurance-type physical activity, of at least moderate intensity, on most preferably all days of the week.” Other expert bodies have concluded that 30 minutes is not enough, especially for kids. The National Association of Sport and Physical Education recommends that elementary school–age children spend at least 60 minutes a day doing moderate to vigorous physical activity. The Institute of Medicine recommends at least an hour of moderately intense activity daily for both children and adults.
Unlike kids a few decades ago, children in the United States today rarely walk or ride their bikes to school or to other destinations. Half are driven to school in cars and about one-third take buses. Less than one trip in seven is made on foot or by bicycle. In a recent survey long distances were most often cited as the reason why children went to school by car or bus, but traffic was a close second. Concerns about traffic danger prevent an estimated 20 million children in the United States from walking or biking to school.
Kids get between 20 percent and 40 percent of their total physical activity at school. School gym classes and recess periods provide the only strenuous exercise many U.S. children get during the week, yet studies suggest that at most schools the minutes children actually spend in vigorous activity are few indeed. Most children in grades 1 through 6 are enrolled in physical education, averaging about three class periods a week. But trained observers watching such classes as part of one research study found that students engaged in only about three minutes of moderate to vigorous exercise per class—less than 10 percent of total class time! Some experts have estimated that during the elementary grades children may average as little as 10 minutes per week of moderate to vigorous activity in school P.E. classes. Furthermore, most children are not taught by P.E. specialist teachers, and many school systems, strapped for funds, have severely cut their physical education budgets in recent years. In the Los Angeles Unified School District, California’s largest, some P.E. classes in middle schools have more than 70 students per teacher. National guidelines recommend no more than 25 students per P.E. teacher. Fields and courts are so crowded that students spend much of their class time waiting their turn to run wind sprints or shoot baskets.
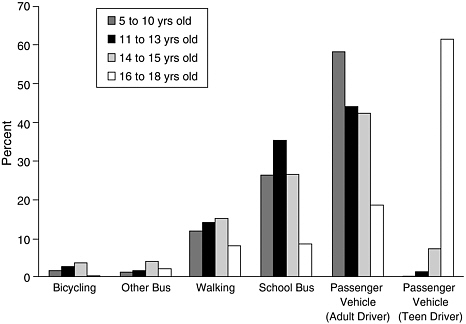
The percentage of trips during normal school travel hours. The majority of children arrive and leave school in automobiles, vans, trucks, and buses.
Source: See Notes.
When children are young, boys and girls are equally physically active, but as they move from childhood into adolescence, starting at about the age of 10, physical activity levels for both sexes—and especially for girls—begin to decline. Decreased emphasis on P.E. classes after elementary school probably contributes to part of the reduction. About half of U.S. schools require physical education for students in grades 1 through 5, but this percentage drops off steeply in the higher grades. Fewer than 10 percent of high schools require physical education for students in grades 10 through 12, even though P.E. programs have been shown to have a strong impact on activity levels in this age group. Higher family incomes, higher levels of maternal education, and access to a community recreation center are also linked to higher physical activity levels among adolescents, while those living in high-crime neighborhoods are less likely to be active.
Along with declining overall activity levels, adolescents of both sexes participate in fewer physically active leisure-time activities (such
as basketball, bicycling, softball, running, and aerobics) as they get older. Why so many teenagers stop participating is not known, but the reasons could be related to academic pressure, exclusion from competitive sports programs, transportation problems, lack of parental support, a need to earn money after school, or the lure of sedentary forms of entertainment such as television and computer games. James F. Sallis, a professor of psychology at San Diego State University, suggests that high school sports programs, with their emphasis on competition and athletic prowess, take money away from physical education programs and paradoxically discourage many teenagers from remaining active and physically fit. High schools often require only one or two years of P.E., and the demands of academic schedules and extracurricular activities often make it difficult or impossible for kids to take more. “There’s this pyramid, especially as kids get older,” Sallis says. “If they’re not the [athletic] elite, they are invited out. They are excluded. We think that this policy to pursue competition and winning, instead of promoting health in these kids, is actually contributing to the decline in activity with age…. The opportunities that are available to kids as they get older are diminished by design.”
Yet daily physical education classes for all students are recommended by federal health guidelines and by the American Academy of Pediatrics (AAP). Daily P.E. classes, lasting 30 to 60 minutes, are recommended in the Institute of Medicine’s 2005 report on preventing childhood obesity, which also urges schools to expand the array of physical activity choices, intramural sports, and clubs they offer, both during and after the regular school day, to meet the needs and interests of more students. The purpose of P.E., especially as children become adolescents, is not only to allow kids to exercise, but to give them the skills they need to play individual sports and develop personal fitness programs that they can continue to follow as adults. “It’s quite rare that that’s a focus in high school,” remarks Sallis.
For girls in particular, the remarkable drop in physical activity that often accompanies adolescence may also be caused in part by biological factors that affect both energy expenditure and behavior. Between the ages of 10 and 18, activity levels fall by 64 percent for white girls and by 100 percent for black girls. About half of high school girls re-
port that they get no vigorous exercise, compared with about one-quarter of high school boys. By the time students are in fifth grade, boys participate nearly twice as much as girls in moderate to vigorous physical activity. From age 6 to 16, boys also retain fairly constant levels of aerobic power relative to their body mass, while girls’ aerobic power declines unless they participate in physical training.
Researcher Michael I. Goran and colleagues at the Universities of Alabama and Vermont repeatedly measured energy expenditures, reported physical activity, and body composition among 11 boys and 11 girls, starting at age 5 and continuing until about age 10. He found that the boys increased their average total energy expenditure at each measurement year, while the girls’ average total energy expenditure declined significantly by age 10 and their reported level of physical activity fell by 50 percent between the ages of 8 and 10. The girls’ food intake (adjusted for their weight), however, did not decrease. These findings suggest that girls may be biologically programmed, perhaps through the effects of sex hormones, to reduce their activity level and to store excess energy in the form of fat as they enter puberty. Such a biological tendency might have evolved as an adaptation that prepares girls’ bodies for eventual childbearing, but it seems maladaptive in our modern environment. The findings on girls’ activity patterns underscore the need to find strategies that will encourage girls to continue to be physically active throughout childhood and adolescence.
Sallis suggests that girls’ decline in physical activity at around the time of puberty could also be socially motivated. Girls at this age worry about looking good and often become self-conscious. “As their bodies develop, they feel like the boys out there are watching them,” he says. “And as girls spend more time fixing their hair, they become less interested in sweating.”
![]()
A variety of ambitious projects have been mounted to gauge the health effects of providing kids with better, more vigorous physical education programs at school. The outcome from such studies is that children unquestionably benefit from having more and better school P.E. time, as measured by increases in their cardiovascular fitness, strength, en-
durance, and even academic performance. However, the track record of most such programs in preventing obesity has been disappointing. One of the most intensive P.E. programs tested so far, as part of the large, federally funded Child and Adolescent Trial for Cardiovascular Health (CATCH), failed to reduce obesity rates in children. CATCH researchers enrolled more than 5,000 third-graders from four areas of the country as participants in an ambitious three-year program to improve diet and boost activity levels. Designed primarily as an effort to reduce children’s blood cholesterol levels and other heart disease risk factors, its effects were assessed in intervention schools and control schools. (The CATCH study is described in more detail in Chapter 7.)
In the P.E. component, classroom and P.E. teachers received special training on providing fun activities geared toward getting kids to spend at least 40 percent of their P.E. class time in moderate to vigorous activity. The CATCH trial succeeded admirably in getting children to play harder: kids in the intervention schools spent more than 50 percent of their P.E. class time in moderate to vigorous activity (compared with 37 percent of class time for kids in the control schools, already a respectable percentage). Kids in CATCH intervention schools also spent more time outside school hours in vigorous physical activity and made healthier food choices. Yet surprisingly, the program did not show evidence of preventing obesity. The body fat content of children in the program, as measured by BMI and skin-fold thickness, did not differ from that of children in control schools. The federally sponsored program Pathways, a similar large, school-based intervention designed specifically to reduce obesity in American Indian children in grades 3 through 5, also did not reduce BMIs.
James Sallis led a two-year California study of an intensified P.E. program called SPARK (Sports, Play and Active Recreation for Kids), in which fourth- and fifth-graders received physical education classes incorporating aerobic dance, jogging, jump rope, basketball, Frisbee, and other games intended to promote high levels of activity. Just as in the CATCH intervention, the goal in SPARK was to minimize the amount of time that any student was not moving. One group of kids took classes with P.E. specialists; one group received SPARK classes led by classroom teachers who had received special training; a third group
served as the control. In both the specialist- and teacher-led groups, children in SPARK significantly increased their in-class activity levels and energy expenditures. Girls in the program showed marked improvement in two fitness measures: their time for running a mile and the number of sit-ups they could do in a minute. (Boys’ fitness scores did not differ from those of the control group—perhaps because, as mentioned previously, boys already tend to be more physically active than girls at this age.) There was also some evidence that SPARK increased students’ enjoyment of physical education and even enhanced their academic performance, and its P.E. program has since been widely adopted for children from preschool to middle school. But SPARK participants did not increase their activity levels outside school, nor could the study document an impact on fatness as measured by BMI or skinfold tests.
Sallis’s conclusion, as he expressed it at a medical conference recently: “School P.E., no matter how good, is not going to fix the problem” of childhood obesity. In practical terms, there is simply not likely to be enough time during the regular school day for children to get all the physical activity that they need. Sallis is now focusing on finding ways to expand physical activity opportunities at other times, especially after school, which he considers the most critical time to get kids moving. “If they’re not active after school, then they’re not active,” he says.
Still, it’s worth noting that a few school-based physical activity programs have had an impact on body fat. An especially intensive P.E. program was tested on fifth-graders in seven schools in Adelaide, Australia. Ten-year-old children in an intervention group received 1 hour and 15 minutes per day of endurance training. Kids in the control group received the schools’ standard 30-minute P.E. classes. At the end of 14 weeks, those in the endurance group were not only fitter but showed a significant reduction in fatness, as measured by skin-fold thickness, compared with children in the control group. The schools in the study adopted the intensive daily P.E. program, and two years later, fifth-graders in the participating schools had less body fat and a lower percentage of obesity than fifth-graders in the same schools prior to the introduction of the intensive program. Despite this positive out-
come, given the heavy academic demands on today’s students and teachers, few health experts or educators are optimistic about the chances of getting U.S. school systems to offer students five hours per week of intensive P.E. classes.
A California pilot program, Dance for Health, provided a small but promising field test of an “alternative” form of P.E. A Stanford medical student devised an innovative dance-based program and tested it among 81 African American and Latino children. The program, led by trained Stanford students, consisted of three 50-minute classes each week during the regular school day in which seventh-graders did dance and aerobics to hip-hop music. Children in the study were randomly divided into two groups, with one group attending the dance classes and the other attending regular P.E. classes, which also met for 50 minutes three times a week. No differences were seen among boys, but girls in the Dance for Health classes significantly lowered their BMIs and their resting heart rates compared with girls in the regular P.E. classes, indicating that they lost body fat and became fitter.
The lesson of Dance for Health was not lost on Tom Robinson, a Stanford University pediatrician who once intended to be a primary care doctor in an underserved area but who instead has devoted his career to figuring out how to get people to adopt healthier habits. After years of studying human behavior, Robinson has learned a key lesson: preaching and punishment don’t work. People, especially kids, do things because they want to, not because someone has told them it’s healthy. The secret is to make people want to do things that are good for them. Dance has become Robinson’s stealth weapon in the battle to get kids to be more active. Hip-hop, African dance, Mexican ballet folklorico, Hawaiian hula, even Black Panther step chants from the 1960s—instructors are teaching all of these styles to elementary and middle school girls as part of various studies Robinson and his team are currently conducting on obesity prevention. “I’ve yet to find an 8-to 10-year-old girl who doesn’t like to dance,” he says.
A friendly man with salt-and-pepper hair and a ready smile, Robinson moves nimbly around his cluttered Palo Alto office, hopping over stacks of papers and journals piled on the floor. His own scientific publications span many of the more important preventive medicine
themes of the past 20 years—smoking, exercise, alcohol abuse, seatbelt use—but in recent years he has focused almost exclusively on preventing obesity. “That has become, to me, the public health challenge of the next century and where we can make the biggest impact,” he says. By testing obesity prevention programs in schools and communities, “I feel I can do more, achieve more and learn more than I could if I were only treating patients as a pediatrician.”
Like a number of other researchers, Robinson has been investigating multicomponent efforts to prevent obesity: encouraging children to exercise, trying to reduce the time they spend watching television or sitting at a computer, and teaching them to make healthier food choices. Although program activities often take place at a school or community center, researchers are trying to involve parents and to influence how entire families behave. For example, the Stanford Adolescent Heart Health Program focused on tenth-graders in four ethnically diverse high schools and offered 20 lessons about diet, physical activity, and the health risks of smoking. It also taught teenagers specific skills for resisting peer pressure to smoke or adopt other unhealthy habits. Compared with students outside the program, tenth-graders in participating schools improved their diets, activity levels, and physical fitness and showed reductions in BMI and body fat.
As part of the Girls’ Health Enrichment Multi-site Studies (GEMS), a federally funded study currently testing strategies to prevent obesity in African American girls, Stanford researchers and members of the local community are conducting a multipart program in Oakland, California. More than 290 girls between the ages of 8 and 10 have been recruited to Stanford GEMS, which started in 2003 and is to run for two years. Those assigned to an intervention group receive after-school classes about their cultural heritage as well as African American dance. Because African American girls have high rates of obesity and also rank high in hours of television watched per week (an established risk factor for becoming overweight), GEMS participants also get regular home visits from staff members during which they are coached and given incentives to reduce TV watching time. The program aims to maximize family and community involvement. Family members regularly flock to GEMS “jamborees” to see their girls per-
form. When planning such celebrations, girls and parents are urged to reconsider the role that certain foods traditionally play. “If someone asks can they bring in a cake for a birthday, we say, ‘Think about whether the dance instructors can come up with a special chant instead,’” Robinson explains.
After two years, the effects of the intervention will be measured by comparing the changes in the BMIs of GEMS participants with those in a comparison group of girls who are receiving nutrition education materials and newsletters. The members of this control group also attend periodic family nights and health events, but they do not receive dance and cultural heritage classes or the TV reduction component. A parallel GEMS study, using a different intervention design, is being carried out by a research team at the University of Memphis in Tennessee.
Robinson says that girls in the Oakland program have responded enthusiastically, practicing their dances at home and eagerly helping to choose music for classes and performances. In an earlier pilot study for the program, researchers noted a reduction in girls’ weight concerns, an improvement in their grades, and fewer symptoms of depression—“things that may be even more important” to the girls themselves than being overweight, Robinson notes.
GEMS and similar prevention programs currently being evaluated are complex interventions rather than simple tests of the impact of boosting children’s physical activity levels. Robinson acknowledges that if GEMS is found to reduce girls’ obesity risk, researchers will have to tease out the relative contributions of the dance sessions versus the television intervention or the cultural heritage classes. “We’ll be able to look at the dose of each,” Robinson says. “It’ll give us some idea of what are the mediators of change.”
![]()
Most of the scientific research that I’ve been describing has focused on trying to get kids to be physically active by making them do something specific: play harder in P.E., for example, or take a hip-hop dance class. But some of the most promising findings on preventing obesity have come from studies that asked a different question: Is it possible to re-
duce obesity in children simply by getting them to cut down on the time they spend being inactive? The answer seems to be yes—and so far, the results of such research suggest that one of the most effective things a parent can do is get children to reduce the amount of time they spend watching TV.
One of the strongest pieces of evidence supporting this strategy comes from Tom Robinson’s work. In 1999 he published the results of an intervention that focused solely on television watching, a study that other researchers often cite as a landmark advance in obesity prevention. In a clinical trial involving 198 third- and fourth-grade students, he showed that simply getting kids to cut down the time they spend watching TV and playing video games—without changing anything else—reduces their chances of becoming fat. The study, published in the Journal of the American Medical Association, represented the first time anyone had tested the effect of reducing TV watching on obesity without at the same time trying to influence what children were eating or how much they exercised. Despite ample earlier epidemiological data that linked time spent watching television with obesity risk, many in the research community and the public were still stunned to discover that just getting kids to watch less TV seemed to help protect them from unhealthy weight gain. To Robinson, such a strategy had cried out to be tested. “It was obvious to me that somebody had to do an experiment,” he recalls.
Two northern California schools participated in the study. In a randomly chosen intervention school, children in the third and fourth grades were taught a series of lessons to motivate them to reduce TV and video time to a maximum of seven hours per week, while kids in those grades at the other school served as the control group. Families of children in the intervention group received electronic television allowance meters that could be locked onto the power plug of a TV set to aid them in budgeting their kids’ viewing time. The device could be set to turn off the TV when the weekly allowance was used up. Participants, families, and teachers were not told that the study’s purpose was to assess the intervention’s impact on obesity. At various points near the beginning and end of the eight-month study, participants from both schools were asked how much time they had spent the previous
day and the previous Saturday watching television or videos and playing video games. They also reported information on their food intake, physical activity, and other sedentary behavior. At the beginning and end of the study, researchers calculated the participants’ BMIs, performed other measurements to assess their body fat content, and tested their cardiovascular fitness.
As expected, children in the intervention group significantly decreased their TV viewing time (by about one-third from baseline level). They also reported meaningful decreases in video game use. This change in behavior was reflected in their bodies. Compared with children in the control group, those in the intervention group showed smaller increases in their BMIs and other measurements reflecting body fat. Although the kids in both the intervention and control groups showed an increase in BMIs and other body measurements during the school year (as is normal for growing children in this age group), the ones in the intervention group gained an average of about 2 pounds less and nearly an inch less in their waist circumferences. These effects occurred in the entire intervention group, but the impact of the intervention was greatest in children who had higher levels of body fatness at the start of the study.
Susan Yanovski, a government scientist who administers funding for obesity research at the National Institutes of Health, remembers being elated by Robinson’s findings and was almost immediately inspired to put them into practice in her home.
“A couple of days after that study came out in JAMA, my kids announced that they had saved all their money and were about to purchase a Nintendo,” she recalls. “I said, ‘OK, but we’re putting in a TV allowance meter.’” Yanovski’s children complained at first, but now the TV meter—the same type Robinson used in his study—has become part of their lives. She sets it to give each of her three children an allowance of four hours of TV time per week. They are allowed to pool their time for a maximum of 12 hours. There’s also a meter on the family computer to monitor the kids’ nonhomework use.
“They budget their time like they would their allowance,” Yanovski says. “If they’re in the middle of a show or a game and they run out of time, it turns off. I think it’s fabulous.” But Yanovski adds that she has
been surprised and disappointed by the reaction she gets when she tells other parents about the device. Only a couple of her friends have followed her example. “Most people say, ‘That’s a great idea, but my kids would never stand for it,’” she reports.
Americans of all ages spend more of their leisure time watching television than engaging in any other activity. In 1997, using data gathered by Nielsen Media Research, Robinson estimated that between the ages of 2 and 17, children in the United States spend an average of more than three years of their waking lives watching TV. Their relationship with the small screen begins early—long before they can read and, in some cases, even before they can walk or talk. In 2003 a survey of a national sample of parents conducted by the Kaiser Family Foundation revealed some startling information about infants’ and toddlers’ exposure to technology: two-thirds of children under the age of 2 are exposed to television, a DVD player, or a computer on a typical day, for an average of two hours. One-quarter of children in this age group have a television in their bedrooms.
As they get older, today’s children rely increasingly on television and videos to fill their leisure time. Between the ages of 2 and 7, kids in the United States spend an average of 2.5 hours per day watching TV, DVDs, videotapes, or playing video games. Between the ages of 8 and 18, the average time spent in such pursuits rises to 4.5 hours per day. More than 40 percent of the third- and fourth-grade children in Robinson’s California TV intervention study had a television set in their bedrooms. By the time kids are in middle school, a Boston study found, more than half sleep in a room with a TV.
The link between time spent in TV viewing and obesity rates in children and adolescents was first detected 20 years ago. In 1985 William Dietz and Steven Gortmaker identified TV watching as a risk factor for childhood obesity by analyzing data from a national health and behavior survey, and this association has since been documented repeatedly in other epidemiological studies. To be sure, most such studies have had the drawback of being cross-sectional, looking at a group of children at a particular point, rather than being prospective (assessing kids’ viewing habits and monitoring the change in their BMIs over time). It’s impossible to tell with certainty from cross-sectional studies

Daily media use among children, including television, video games, radios, cassette tape players, VCRs, compact disc players, and computers.
Source: See Notes.
whether a factor is a cause or a result—for instance, whether television watching makes a child overweight or whether being overweight prompts a child to watch a lot of TV.
However, a 1996 study by Gortmaker suggested that a “dose-response relationship” exists between hours of television watched and the likelihood of being overweight. And Dietz and Gortmaker’s original 1985 study did contain some prospective evidence indicating that TV watching was a contributing factor to weight gain: it found that in a national sample of more than 2,000 children, those who had watched more hours of television when they were between 6 and 11 years old had higher rates of obesity later when they were between 12 and 17.
A television set in the bedroom appears to be an especially strong risk factor for kids. Barbara A. Dennison of Columbia University reported in 2002 that preschoolers with a TV set in their bedrooms were 31 percent more likely than those who did not to have BMIs above the 85th percentile for their age (the category termed “at risk of over-
weight” in official health guidelines). Gortmaker estimates that having a television in the bedroom automatically adds an average of an hour per day to a child’s TV viewing time. “Never put a TV set in the room where a kid sleeps,” he advises parents. “You sort of lose control of your kid in a whole range of ways.”
It seems like common sense to assume that people who watch a lot of television are likely to be fatter than those who don’t because they spend less time moving their muscles. (Such thinking is probably the logic behind the term “couch potato.”) Although scientific evidence certainly supports the assumption that TV and related technologies contribute to obesity risk by making children more sedentary, this is apparently not the entire explanation. Tom Robinson notes that when TV was introduced into small communities in Canada and Scotland, children’s participation in physical activities decreased. On the other hand, in Robinson’s own study testing the effect of reducing kids’ TV viewing time, he found, surprisingly, that children in the group who cut down on TV time did not significantly increase their levels of moderate or vigorous physical activity, nor did they become more fit. Nevertheless, they were less likely to become overweight than the control group who did not reduce their television viewing.
In addition to making kids inactive, TV watching may also influence what and how much children eat. Food and drink consumed while watching television contribute about 18 percent of the average child’s total daily caloric intake on weekdays and as much as 26 percent on weekends. Some studies indicate that children eat more high-fat and high-calorie foods when they eat while watching TV, perhaps partly in response to commercials for such foods. The average child sees more than 40,000 television commercials each year. Children’s programming is replete with advertising for snack foods, sweetened breakfast cereals, soda, and other foods high in fat, sugars, and total calories. Companies buy commercial time on children’s shows because they know that such ads work: experiments have shown that children respond to food advertising by tending to choose and consume the advertised products. Child development research has shown that children younger than 7 or 8 do not understand that commercials are different from other program content.
Fruits, vegetables, and other unprocessed foods high in fiber and low in calories are almost never advertised, since they are difficult to brand and turn into profitable products. A 2001 study found that in families that watched television during two or more meals per day, children reported consuming significantly fewer fruits and vegetables and more red meat, pizza, sodas, and salty snacks than did children from families that did not watch TV during meals. Even the fact that many kids eat and watch television lying down may also help to boost their total food intake. A recent Australian study found that people who eat lying down take longer to feel full than those who eat sitting up, possibly because less food is retained in the stomach of a reclining person.
In addition, watching TV may consume even less energy than other sedentary activities children engage in, such as reading or drawing or talking on the telephone. In laboratory studies of kids between the ages of 8 and 12, one research group found that children’s resting metabolic rates (reflecting calories burned by their bodies) were significantly lower while they watched TV than when they sat still with the television turned off. Some researchers hypothesize that kids’ metabolic rates drop while watching television because they fidget less. Other scientists have failed, so far, to confirm this finding.
![]()
Tom Robinson’s 1999 intervention trial on the effect of reducing TV and video time was a relatively small pilot study. He has since replicated the findings in a larger, 12-school trial; the results of that project are still being analyzed and have not yet been published. However, additional evidence supports the idea that reducing the time children spend watching TV and videos helps prevent or treat obesity. In studying obese children aged 8 to 12 in his treatment program, Leonard Epstein, a psychologist and professor of pediatrics at the State University of New York at Buffalo, found that those who were rewarded for decreasing sedentary activity lost more weight after one year than groups who were rewarded for increasing physical activity. Television watching was among the sedentary activities targeted, along with computer games, board games, talking on the telephone, and imaginative play.
Steven Gortmaker also tested the effect of targeting children’s TV viewing time as part of a study of Planet Health, a comprehensive obesity prevention program for middle school children that also aimed to cut intake of high-fat foods, increase fruit and vegetable consumption, and boost kids’ levels of physical activity. (Planet Health is described in more detail in Chapter 7.) Children in the schools where Planet Health was introduced significantly reduced the time they spent watching TV, and that behavior change correlated with reduced rates of obesity in the girls, although not in the boys. Gortmaker credits Planet Health’s TV reduction message—absent from most other school-based obesity prevention curricula—for producing much of the program’s favorable effect on children’s BMIs. “My sense is that this is a very important variable that everybody has been ignoring,” he says.
Similarly, researchers conducting the Growing Up Today Study, an ongoing cohort study of almost 12,000 children, found that among girls, those who increased the time they spent watching TV and videos or playing video games over a one-year period showed a corresponding increase in BMI levels. Girls and overweight boys in the study who increased their physical activity level during the same period showed a drop in BMIs. Together, these findings “all suggest that control of TV time has an impact on weight,” says William Dietz of the federal Centers for Disease Control and Prevention. “The other thing about control of television time is that there’s no negative. There is no adverse effect of reduced TV time.” Children’s TV and video time should be limited to no more than one to two hours a day, Dietz argues. That is also the official position of the American Academy of Pediatrics, which further recommends that programs watched by kids should be educational and nonviolent. The academy opposes allowing children under 2 to watch any television at all because of the activity’s potential for interfering with learning to talk and play with others during a period of rapid brain development.
“Parents need to be in charge of television,” Dietz says. “It’s not as though that is a harmless machine in their house. If there were a guest for dinner who would make your child fat or teach them about alcohol, sex, and violence, would you actually invite [that person]? Television has that impact on children.”
![]()
Television and video technology are a pervasive part of American culture, and in many families they function as a cheap and convenient electronic babysitter, especially when adults are busy, stressed out, exhausted, or absent. Small wonder, then, that so many parents assume that their kids would never stand for having their TV watching time cut back. But Steven Gortmaker’s research with children suggests that kids are less enamored of television than their parents might think. In testing the Planet Health program and in other studies, Gortmaker and his colleagues found that it is not difficult to persuade students in middle school and elementary school to watch less TV. “Most of the time that kids watch TV, they’re not having a good time,” he says. “They’re just filling time—killing time.”
An early lesson in the Planet Health curriculum is entitled “What Could You Do Instead of Watching TV?” The teacher explains to students that watching too much television can prevent kids from doing physical activities and can make them lose muscle strength, flexibility, and cardiovascular endurance as well as increase their risk of becoming overweight. Students make a pie chart of how they spend their time, and add up the number of hours of TV that they watch during the week. They learn that doctors recommend that they watch a total of no more than two hours of TV a day. “Watch only shows you like,” the students are advised. “Take note of the times when you watch TV but aren’t really interested—when you channel surf or watch reruns—and use that time to be physically active instead.” Kids are asked to set goals for cutting back their TV time and replacing it with other activities. Suggestions are provided on classroom posters and on a Planet Health Web site. “They write about what else they think they can do,” Gortmaker says. “They interview a grandparent about what people used to do before TV. Kids are very creative, and they can think of lots of alternatives. The key is replacing it with something they would rather be doing—and the great thing about TV is, just about anything else is more active.”
Susan Yanovski suggests that parents who want to set limits on children’s TV time should consider not hooking up their homes to cable television or should think about getting rid of it if they’re already
connected. “We don’t have cable,” she says. “Not only do we save the money, but there’s very little on TV that our children want to watch.” She also enforces a simple household rule for everyone in the family: no eating in front of the television set.
Leonard Epstein agrees that children readily find alternatives when their TV watching time is cut back. The key, he believes, is focusing on reducing the sedentary activity and letting the child choose what to do instead. He suggests that reducing the time that children spend watching TV and videos by 50 percent is a reasonable initial goal for many families. “If you just reduce access to sedentary behaviors, then kids will fill that time up,” he notes. “You don’t even have to talk about physical activity. They’ll automatically do it.” Epstein is currently using electronic TV allowance monitors successfully as part of programs both for treating and preventing childhood obesity. In one ongoing prevention study in children between the ages of 4 and 7, he says, “We’re trying just to reduce TV watching and prevent excessive weight gain.”
But like Yanovski, Epstein acknowledges that fundamentally changing children’s relationship with television also requires changing the attitudes and behavior of the adults in the family toward the technology. So far, he has found that to be a discouragingly difficult task. “We’ve not had any success when we talk about getting TVs out of kids’ bedrooms,” he admits. “We’ve had absolutely no success in reducing the number of TVs in homes. We tell parents, turn the TV toward the wall, or put hard-backed chairs in front of the TV. My perception is, people just don’t want to do that. They’ve invested the money in getting the living room just right. Now we’re telling them to change, and they’re not going to do it.”
Steven Gortmaker finds, much to his alarm, that the majority of the parents with whom he talks are unconcerned about how much TV their children watch. “It’s not on their radar screen,” he says. He believes that a fundamental change in parents’ attitudes will require a shift in the norms of American culture similar to the shift that has occurred in recent decades in attitudes about smoking. He tells parents: “You don’t put a gun in a room where a kid sleeps. You don’t put a refrigerator in a room where a kid sleeps. You don’t put a TV in a room where a kid sleeps.”
![]()
When obesity researcher Bob Kuczmarski moved with his young family to Columbia, Maryland, more than a decade ago, one of the things that attracted him to the area was the bike paths. Unlike most American suburbs, Columbia was designed as a planned community. Almost 100 miles of paved pathways for walkers and bikers connect the neighborhoods to one another, to open areas with woods, streams, and playgrounds, and to a town center with inviting shops. When the two Kuczmarski boys were small, their parents would wheel them down the path to the town center in strollers. Later the parents rode their bicycles and the boys followed along on tricycles or small bikes with training wheels. Now, at 13 and 10, the boys regularly walk or bicycle to the playground or to friends’ houses. Often the whole family walks to the center, which offers sporting goods, toys, videos, crafts supplies, a Target store, and a deli. They frequently go hiking or camping together on weekends.
Life in Columbia is far from perfect, Kuczmarski admits. His property taxes are high. He commutes 30 miles each way, through heavy traffic, to and from his Bethesda office, and his wife’s commute is more than twice that distance. The community, located near I-95, the highway that links Washington, D.C., and Baltimore, has its share of burglaries and drug problems. Once, Kucmarski recalls, while biking with his youngest child during the middle of the day, he came upon some teenagers on the bike path selling marijuana. Like other parents he worries about his boys’ safety and does not allow them to bike or walk on the wooded paths after dark. But Kuczmarski, who grew up loving the outdoors, knows that studies have shown that the amount of time children spend outside is the strongest predictor of their overall activity level. Even though he chose an environment that offers his family the best chance he can give them of maintaining a physically active lifestyle, he wishes that he could offer his sons the same degree of freedom his parents gave him as a child in rural Ohio. “I would leave home in the summer early in the morning and as long as I was home for dinner, that’s all they cared about,” he says. “I was out in the woods, fishing.”
Recent findings suggest that modern America’s sprawling suburbs,
designed in a way that forces people to rely on cars, are contributing to the obesity epidemic in children and adults. Many communities lack sidewalks and are laid out with schools and shops on the periphery, too far to make walking practical. A national study ranked the population density of 448 U.S. counties and compared the rankings with survey data on residents’ weight and blood pressure. It found that people who lived in the most densely populated areas, such as New York City, weighed as much as 6 pounds less than those in the most sprawling ones. The authors speculated that the daily walking done by city dwellers made the difference. A smaller study by San Diego State University’s James Sallis comparing two San Diego neighborhoods found that people living in the one close to shops and public buildings walked or biked significantly more often than those in the more sprawling neighborhood. Findings from these and similar studies are prompting policymakers and urban planners to call for changes in the way new developments are laid out and to urge “retrofitting” of some existing communities to make them more convenient, safe, and inviting for walking.
As a government researcher with the National Center for Health Statistics, Kuczmarski coauthored the landmark 1994 study that alerted doctors and the public to the existence of an obesity epidemic in U.S. adults. He later worked on other studies documenting a parallel epidemic in children. Now his job is to administer federal grants to other researchers seeking ways to combat the epidemic. Although he must spend long hours sitting at his computer, he does all he can to ensure that physical activity is part of his and his family’s routine. He never takes the elevator, climbing six flights of stairs to his office each morning. Whenever he goes to the restroom, he climbs three more flights rather than use the one on his own floor. At home, he and his wife share in doing the laundry, carrying hampers up and down stairs. He mows his own lawn. His boys are required to help with housework and yardwork. He limits their television time to about half an hour a day and allows them to watch only if all their homework is done. Everyone takes turns walking the dog.
At the office, he and other experts working on obesity prevention at the National Institutes of Health sometimes trade tips about ways
they have found to build a little more physical activity into their families’ household routines—small things like choosing not to put in extra telephone extensions or getting rid of the TV remote control. Says colleague Susan Yanovski, “We all tend to look for ways to make things easier—but sometimes you need to look for ways to make things a little harder.”
Thanks to the Kuczmarski family’s active lifestyle, the boys love sports and playing outdoors. “One of their biggest frustrations is that they don’t get enough physical activity at school,” Kuczmarski says. Kids, he believes, have a natural tendency to maintain a balance between work and active play. “I think we sort of breed it out of our children.” Research supports the view that children are happiest when physically active and suggests that parents can strongly influence their kids’ chances of remaining active as they grow up. Steve Gortmaker cites research by psychologists who contacted kids as they went through their daily routines and asked them how they were feeling. Parks and recreational areas were among the places where children reported feeling best, he says. “Kids really enjoy playing and running around.”
Undoubtedly, some of the influence parents exert on their kids’ physical activity levels is genetic. Children of athletes are likely to inherit a variety of traits that boost their chances of being athletically talented. But parents also teach their children habits regarding physical activity by their example, by their attitudes, and by what they make available. Kids whose parents are physically active are almost six times as likely to be active themselves as are the children of inactive parents. At least one study suggests that parental activity levels are more closely correlated with exercise frequency among girls than among boys.
Parents can start early to give their children the message that moving around is both fun and valuable. Dancing around the living room with a toddler, playing catch or hide and seek, taking family walks or bike rides, making active outdoor games a regular part of holidays and celebrations—these and other simple activities help children grow up enjoying play that uses their hearts, lungs, and muscles. Early exposure to swimming, running, climbing, and ball throwing helps children acquire physical skills and confidence in their bodies, which might, in turn, lead to an increase in physical activity undertaken. Positive new
experiences increase a child’s self-efficacy, the sense that he or she is capable of facing a new challenge and succeeding. At the same time, play and sports should be tailored to a child’s developmental level. Preschoolers, for example, can’t be expected to concentrate on structured activities lasting longer than 15 or 20 minutes; most of their exercise should be free play.
Organized team sports can develop athletic skill and team loyalty but should not become a child’s exclusive focus. Children also benefit from learning the skills used in individual sports—such as swimming, bicycling, tennis, running—that they may be more likely to continue to do as adults. Parents who emphasize competition, hold unrealistic expectations, and criticize a child’s performance run the risk of souring their children’s attitude about sports and physical activity. According to the AAP, the factors that foster a positive attitude toward sports in kids are “fun, success, variety, freedom, family participation, peer support, and enthusiastic leadership.” Experiences likely to prejudice children against continuing to participate in sports are “failure, embarrassment, competition, boredom, regimentation, and injuries.”
Besides encouraging physical activity at home, parents can play a vital role in advocating opportunities for kids to be active at school and in the community. Physical education is an important and often neglected component of the school curriculum. “I think we need to get parents to put pressure on the school districts to reallocate more funds away from [organized sports] and more for physical education,” says James Sallis. Afternoons are a time when parents—regardless of their own schedules and where their children go after school—should try to make sure their kids have a chance to move around and burn energy, he advises. If a child does not come home after school, parents can try to ensure that active play is encouraged at the after-school program or child-care setting. They can also see that balls, jump ropes, and other sports equipment are available to kids and can link up with other families to research local sports opportunities, organize games and activities, or form carpools. “Let them be active first, either around the neighborhood or around the after-school program,” Sallis recommends. “We like for kids to be active before doing homework, because they can do the homework after dark. It takes two things: it takes the
community making those opportunities available, and it takes the parent taking advantage of those opportunities.”
![]()
James O. Hill considers himself a realist: in tackling the obesity epidemic, he believes in asking people to make small changes. As director of the Center for Human Nutrition at the University of Colorado Health Sciences Center and as an expert in obesity treatment and weight management, he knows firsthand from years of research how hard it is for overweight people to keep pounds off once they’ve lost them. Nevertheless, he believes that slowing or stopping the obesity epidemic in children and adults could happen if a large percentage of the U.S. population would be willing to make a small, conscious, permanent change in how much they eat and how much they move each day.
Hill’s research shows that among formerly overweight people who have successfully reduced their body weight, keeping the excess pounds from coming back typically requires a high level of activity—about an hour a day. “That’s the one thing that’s causing most of the failures out in the real world, and people don’t understand that,” he says. But considerably less activity—about 15 or 20 minutes a day—is sufficient to prevent weight gain from occurring in the first place. Thus, Hill reasons that the best strategy for reversing the obesity epidemic is to target the entire population and get people to modestly increase their activity levels. “I think the future is, we have to stop weight gain,” he says. “If we did that, in a couple of generations we would be out of the epidemic.”
That principle prompted Hill to develop Colorado on the Move, an initiative launched in his home state in 2002. The program’s goal was to get Coloradans—young or old, fat or thin—to walk an additional 2,000 steps per day, which amounts to about a mile. Hill reasoned that trying to get program participants to reach 10,000 steps per day—a level of activity that health experts consider desirable for adults—was too ambitious, considering the sedentary, car-dependent lifestyles of many people. The program offered participants belt-mounted pedometers and asked them to find out how many steps they
took daily and then boost that total by 2,000. It combined a media campaign with local efforts and special events in schools, workplaces, and communities. People were also given alternatives to walking through guidelines for converting other activities, such as biking or swimming, into an equivalent number of steps. Posters and advertisements provided an array of suggestions for ways to boost the daily step count: Get off the bus earlier and walk to work. Park farther from the grocery store, and always return the shopping cart to the storage area after unloading groceries. Take the stairs instead of the elevator. Take after-dinner family walks.
In surveys of participants around the state, Hill and his colleagues were able to show that people using the pedometers did increase their daily step counts—often by even more than 2,000 steps a day. Now he’s trying to document the same result in a larger statewide survey and to do studies that determine whether a small daily increase in activity has a measurable impact on a population’s obesity rates. Hill says that 200,000 people in Colorado have participated in the program and that at least seven other states have set up similar initiatives. A national version, America on the Move, was launched in 2003, with plans to expand to all 50 states during the next few years.
Meanwhile, James Hill is working on perhaps the biggest challenge inherent in this and similar communitywide campaigns: trying to ensure that participants continue to maintain their new, healthier level of activity. “If you just give people a stepcounter, they’ll get excited about it for a while and then they won’t do it,” Hill says. “Sustainability of the program depends on giving people a continued reason to do it and to monitor their steps.”
The original idea behind the Colorado on the Move program was to shift people’s energy balance by getting them to adopt at least one behavior per day that eliminates 100 calories. The average American adult gains about 2 pounds a year as a result of taking in more energy (in the form of food) than is burned by resting metabolism and physical activity. For most adults, Hill calculates, weight gain can be completely avoided if people can shift their energy balance to prevent them from storing about 50 calories per day as fat. Since excess calories ingested are not stored by the body with 100 percent efficiency, he esti-
mated that most adults could avoid gaining weight if they shifted their energy balance by about 100 calories a day, through some combination of increasing their physical activity and reducing their food intake. Walking an extra 2,000 steps daily will accomplish that goal. So will going without a chocolate chip cookie for dessert. The program’s designers would prefer that participants try to do both, although counting steps with a pedometer is far easier than tightly monitoring daily food intake. People need not count their daily calories, Hill emphasizes. “Counting calories is too hard, too cumbersome. What we are doing is those two simple messages: walk 2,000 [extra] steps and eat 100 calories less.”
The goals are the same for children participating in Colorado on the Move. Hill cites preliminary data indicating that the approach can prevent weight gain, at least in girls and in women. In one study, researchers enrolled families who had at least one overweight child and encouraged them to do two things: walk 2,000 extra steps each day and eat a healthful cereal for breakfast. (The latter goal was chosen because research indicates that people who eat breakfast reduce their risk of becoming overweight.) Hill said that in the family study, girls who participated in the program had lower rates of becoming overweight than girls in a control group, and mothers who participated in the program actually lost weight. No significant effects were seen in the boys or their fathers. Another study conducted in middle school students found that participating in Colorado on the Move increased children’s physical activity, but Hill says he does not yet have data showing whether it reduces their BMIs.
Colorado on the Move is expanding into schools and is enrolling increasing numbers of children. Hill aims to keep the program’s message simple. He adds that he chooses his battles carefully. For instance, the program does not seek to reduce TV watching because Hill does not believe it’s possible to get large numbers of people to make that change. “Even though I totally think TV viewing is related to inactivity and obesity, I’m not going to expend my effort getting people to watch less TV,” he says.
Many food and beverage manufacturers and fast food restaurant chains have responded to publicity about the obesity epidemic by es-
tablishing initiatives to promote physical activity, so Colorado on the Move has attracted plenty of corporate sponsors. Its national parent program, America on the Move, is sponsored primarily by food and beverage companies—Pepsico, Cargill, and Masterfoods USA, according to information provided by a link on the program’s Web site. Hill says that in order to promote physical activity he is quite willing to work with companies that many people might view as contributors to the obesity epidemic. “We would be very happy to partner with McDonald’s,” Hill states. “Our approach is, the McDonald’s of the world aren’t going to go away…. People are going to eat at McDonald’s. If they can go into McDonald’s and come out having eaten 100 calories less than they would have, or with a physical activity message, then I think we’ve made progress.”