Data Integration in Learning Health Care Systems for Traumatic Brain Injury: Proceedings of a Workshop (2024)
Chapter: 1 Introduction
1
Introduction1
Traumatic brain injury (TBI), in which an external force causes a disruption to normal brain physiology or function, affects millions of Americans each year. “Causes as diverse as falls, sports injuries, vehicle collisions, intimate partner violence, and military incidents can result in such injuries across a spectrum of severity and among every age group” (NASEM, 2022, p. 15) with symptoms that can be debilitating, long-lasting, and carry physical, cognitive, emotional, social, behavioral, and financial ramifications. The heterogeneity of TBI makes care and research challenging. The true prevalence of TBI is also not fully understood, given that most surveillance data come from hospital and patient health records, and many people who experience TBI, particularly at the milder end of the severity spectrum, do not seek hospital care. Individuals who do seek medical care often encounter challenges in navigating the stages of treatment and recovery after discharge from acute care. As several speakers noted during the workshop, the fragmented nature of the U.S. health care system and its siloed databases contribute to challenges in the patient experience and to knowledge gaps about TBI prevalence, comorbidities, risk factors, and longer-term outcomes. Learning health systems (LHSs) refer to research-partnered care networks that analyze data from patient care and other sources and use
___________________
1 The planning committee’s role was limited to planning the workshop, and the Proceedings of a Workshop was prepared by the workshop rapporteurs as a factual summary of what occurred at the workshop. Statements, recommendations, and opinions expressed are those of individual presenters and participants and are not necessarily endorsed or verified by the National Academies of Sciences, Engineering, and Medicine, and they should not be construed as reflecting any group consensus.
those insights to continuously improve their health services. Transforming TBI health systems and research networks into LHSs offers opportunities to expand the TBI knowledge base, accelerate advances in care, and address patient barriers to accessing effective treatment.
INTEGRATING THE LEARNING HEALTH SYSTEM CONCEPT AND THE TRAUMATIC BRAIN INJURY ROAD MAP
Odette Harris, professor of neurosurgery at Stanford University and deputy chief of staff for rehabilitation at the Veterans Affairs Palo Alto Health Care System, provided an overview of the development of the LHS concept and how this concept intersects with TBI needs and opportunities to advance research and improve care and recovery. In 2006, the Institute of Medicine convened the Roundtable on Evidence-Based Medicine in an effort to transform how evidence of clinical effectiveness is generated (IOM, 2007). The development of the LHS framework was born from that effort. The roundtable established the following priorities:
- Commitment to the right health care for each person;
- Putting the best evidence into practice;
- Establishing the effectiveness, efficiency, and safety of medical care delivered;
- Building constant measurement into our health care investments;
- Establishment of health care data as a public good;
- Shared responsibility distributed equitably across stakeholders, both public and private;
- Collaborative stakeholder involvement in setting priorities;
- Transparency in the execution of activities and reporting of results; and
- Subjugation of individual political or stakeholder perspectives in favor of the common good.
The roundtable focused on three dimensions of the challenge of creating a system that embodies these priorities: (1) fostering progress towards a long-term vision of an LHS, (2) advancing the discussion and activities necessary to meet the near-term need for expanded capacity to generate evidence to support medical care that is maximally effective and has the greatest value, and (3) improving a public understanding of the nature of evidence-based medicine. Although fully achieving these priorities would be impractical for all interventions, Harris said, discussions during a 2006 workshop and subsequent learning health system activities explored why “[t]he nation needs a healthcare system that learns” (IOM, 2007, p. 3).
The 2006 roundtable workshop highlighted challenges, uncertainties, and the compelling need for change, Harris continued. Aspects identified by workshop speakers within the need for change included adaptation to the pace of change, stronger synchrony of efforts, a culture of shared responsibility, a new clinical research paradigm, public engagement, incentives aligned for practice-based evidence, and leadership (IOM, 2007). Efforts to realize these goals included publication of The Learning Health System Series, which features numerous volumes on various LHS components.2 Volume topics of particular relevance to this workshop include data utility, data quality, evidence, effectiveness research, digital platforms, and research and practice integration. Harris also underscored the importance of emphasizing effectiveness research rather than only efficacy research to understand results in real-world settings.
In 2020, the National Academies convened the Committee on Accelerating Progress in Traumatic Brain Injury Research and Care to develop a report that identifies major barriers and knowledge gaps impeding progress, highlights opportunities for collaborative action, and provides a road map to guide the TBI field, said Harris. The 18-member committee representing diverse disciplines used data from a literature review, public workshop and webinar sessions, and input from over 50 stakeholders in crafting the consensus report Traumatic Brain Injury: A Roadmap for Accelerating Progress (NASEM, 2022). The report considered the multiple stages of care after TBI: recognition, acute care, classification, rehabilitation, follow up, and recovery and reintegration (see Figure 1-1).
Recognition involves awareness of the signs and symptoms of TBI to properly identify individuals in need of medical treatment. Acute care provides the medical interventions needed to stabilize an individual after a TBI and mitigate ongoing damage resulting from the injury. Classification assesses the nature and severity of a TBI to inform diagnosis, prognosis, treatment, and reassessment as the condition evolves. Harris emphasized that classification is not a static diagnosis or assessment. To address the whole person, she said that rehabilitation interventions should be designed to improve physical, cognitive, and psychosocial functions and quality of life. Follow up involves continued engagement with the care system to identify and address ongoing and emerging needs, including provision of community-based support services. She also emphasized that follow up must be continuous and ongoing. Recovery and reintegration aim for recovery of function to the greatest extent possible, including return to family, community, work, or school.
___________________
2 More information about The Learning Health System Series, including links to the various volumes, is available at https://nam.edu/programs/value-science-driven-health-care/learning-health-system-series/ (accessed December 12, 2023).
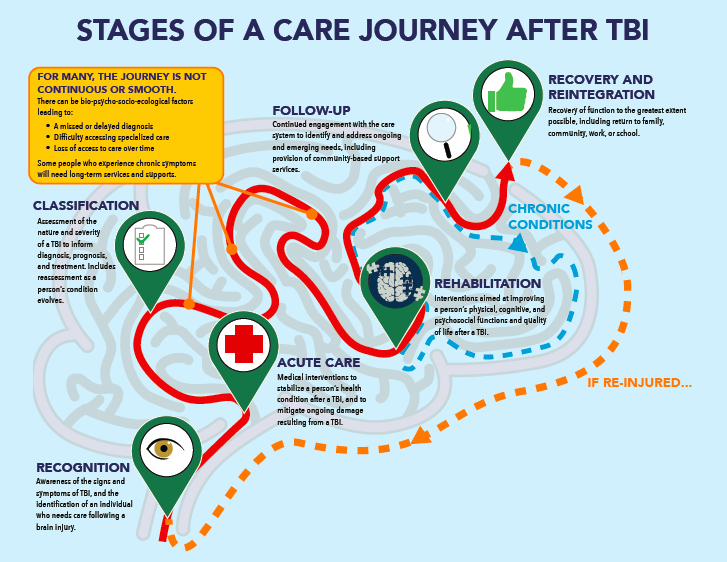
SOURCE: Presented by Odette Harris, October 12, 2023. NASEM, 2022.
As recognized in the report, navigating these stages is often not a continuous or smooth process, and biological, psychological, social, and ecological (bio-psycho-socio-ecological) factors can lead to missed or delayed diagnoses, difficulty accessing specialized care, and loss of access to care over time. Some individuals with TBI experience chronic symptoms and require long-term services and supports. Furthermore, re-injury can cause a person to restart the cycle-of-care stages, requiring consideration of the re-injury effects and stage-integration implications on a patient.
Harris highlighted several additional takeaways from the report:
- TBI is not an isolated, acute event and needs to be understood and managed as a condition influenced by numerous factors that can have long-term effects.
- An updated and more precise TBI classification system is needed to guide patient care and inform research.
- The United States lacks a comprehensive framework for the full continuum of care needed for individuals with TBI.
- An effective care system needs to anticipate, respond, and learn in a coordinated fashion.
- Progress has been made in TBI understanding and care, and opportunities for collaborative action could advance TBI awareness, prevention, treatment, and research (NASEM, 2022).
To help make progress in these and other areas, the report recommends better integrating TBI systems of care and TBI research into LHSs. Harris emphasized that these goals are aligned with the LHS core principles discussed at the 2006 IOM roundtable workshop, which explored how an LHS can be safe, effective, equitable, efficient, accessible, measurable, transparent, secure, and adaptive (described further in Chapter 2).
Following publication of the TBI Roadmap report, the National Academies established the ongoing Forum on Traumatic Brain Injury, the convener of this workshop, to advance the implementation of the report’s recommendations and foster continued progress and innovation in TBI prevention, care, and recovery.3 This workshop was designed to bring together lessons from the TBI report and LHS principles to explore how LHS practices can be operationalized to integrate knowledge and advance TBI care and research. Ultimately, Harris concluded, an improved system of TBI care and research stands to aid in providing patients and families with more effective services.
WORKSHOP OBJECTIVES
Fragmented and siloed TBI treatment and data undercut the current health system’s ability to learn and improve (NASEM, 2022). LHSs are important contributors to progress in TBI, where much remains to be understood about prevalence, outcomes, and effective interventions. Achieving an integrated TBI system involves thorough surveillance efforts, standardization of patient-level data collection, and analysis of longitudinal data. To better understand the development of such a system, the Forum on Traumatic Brain Injury hosted a 1-day public workshop—Data Integration in Learning Health Care Systems for Traumatic Brain Injury—to explore needs, practices, and models for LHSs in the TBI field. Discussions did not focus on a specific type of TBI or sub-population that experiences it; rather, sessions aimed to introduce LHS concepts and illustrate their relevance to systems of care and research for this condition. The workshop, which was held virtually and in person on October 12, 2023, featured invited presentations and discussions to accomplish the following:
___________________
3 Information about the forum and its activities is available at https://www.nationalacademies.org/our-work/traumatic-brain-injury-forum (accessed January 3, 2024).
- Explore the variables affecting how TBI patient data are collected, standardized, harmonized, accessed, and analyzed—and the LHS implications for TBI care and research.
- Discuss a vision for how enhanced TBI data integration in LHSs could improve care and advance clinical and epidemiological research.
- Consider key questions and priority use cases that could be explored through integrated patient record databases and TBI registries.
- Spotlight ongoing efforts towards building integrated research platforms and datasets for TBI.
ORGANIZATION OF THE PROCEEDINGS OF THE WORKSHOP
This proceedings summarizes the presentations and discussions from the workshop Data Integration in Learning Health Care Systems for Traumatic Brain Injury. The workshop highlighted selected opportunities, challenges, and strategies for fostering learning health systems, moving from the LHS concept and its applicability to unmet TBI care and research needs to the types of data, infrastructure, and partnerships needed to establish such systems. It featured examples of LHSs being created by health care organizations, federal agencies, and research networks, and illustrated how enhanced data integration and analysis could support learning and improvement. The workshop thus aimed to introduce how LHSs can help address unmet priorities and inform further efforts in this area but did not aim to cover all aspects comprehensively.
Following Chapter 1—which introduces the LHS framework and its relevance to advancing TBI care and research—Chapter 2 provides a personal account of the lived experienced of TBI, including effects of the condition, difficulty in navigating care systems, and barriers in accessing effective treatment. The chapter highlights the challenges that arise from fragmented and uncoordinated care and underscores the benefit of health information systems that enable provider collaboration and improve the patient navigation experience. Chapter 3 outlines the development of the LHS concept, the definition and core principles of an LHS, current and anticipated efforts to transform the health care landscape through the integration of these principles, and opportunities specific to TBI that such a transformation could seize upon.
Chapter 4 features stakeholder perspectives on using LHS principles to address priority research questions and care needs. The chapter highlights elements including payment models, sociotechnical infrastructure, feedback loops, and outcome comparisons as mechanisms to identify gaps and barriers to effective TBI treatment and to develop strategies to create systems that better meet patient and institutional needs. Chapter 5 offers illustrative
examples of current TBI initiatives that employ LHS principles to support care delivery, improve health outcomes, and expand research opportunities. The chapter spotlights advances in TBI interventions, innovative tools, surveillance, and the knowledge base achieved via LHS practices. Chapter 6 examines efforts by federal and state agencies to capture data, conduct surveillance, and support long-term care needs associated with TBI. The chapter underscores the value of interoperability and data standardization in deepening the understanding of TBI, particularly in terms of prevalence, comorbidity, and outcomes data.
Chapter 7 explores the use of LHSs to build and enhance the TBI response capacity of community systems to combat inequitable TBI outcomes within vulnerable populations and geographic locations. Appendix A contains the reference list. See Appendixes B and C for the workshop statement of task and agenda and Appendix D for brief biographies of speakers, moderators, and planning committee members.
This page intentionally left blank.







