Data Integration in Learning Health Care Systems for Traumatic Brain Injury: Proceedings of a Workshop (2024)
Chapter: 5 Examples of Learning Health Care Systems in Traumatic Brain Injury
5
Examples of Learning Health Care Systems in Traumatic Brain Injury
Key Points Highlighted by Individual Speakers1
- Comparing Treatment Approaches to Promote Inpatient Rehabilitation Effectiveness for Traumatic Brain Injury (CARE4TBI) is a therapist-driven effort to identify effective rehabilitation approaches through data analysis of clinical practice. (Bogner)
- CARE4TBI engaged clinicians in creating standardized data elements for documenting clinical care in the electronic health record that aligned with the priorities of rehabilitation services providers, while providing a format that is amenable to data extraction and analysis. (Bogner)
- A learning health system (LHS) should enable exploration of highly specific questions relevant to patients with traumatic brain injury (TBI). (Giacino)
- The Transforming Research and Clinical Knowledge in TBI study has led to advances in TBI assessment tools such as the Glasgow Outcome Scale-Extended, OsiriX common data elements software for evaluating MRI scans, and TBI blood biomarker rapid testing. (Giacino)
___________________
1 This list reflects the rapporteurs’ summary of points made by the identified speakers, and the statements have not been endorsed or verified by the National Academies of Sciences, Engineering, and Medicine. They are not intended to reflect a consensus among workshop participants.
- The Department of Defense TBI Center of Excellence has conducted surveillance and data analysis projects to identify military occupational specialties at higher risk for TBI and the prevalence of various comorbidities in the months before and after TBI. (Stout)
- Feedback loops enable systems to better meet the needs of patients and providers and should be implemented early in system design. (Giacino, Stout)
- LHS challenges include medical documentation that is not formatted to allow for outcome and program evaluation, as well as databases that lack interoperability and thus limit data aggregation. (Bogner, Evans, Stout)
- Payment models that support the implementation of identified effective practices are needed to enable provision of TBI care that leads to best outcomes. (Giacino, Harris, Manley)
- Refining how the severity of TBI is classified is a critical step to improving care and outcomes. Also critical are the consideration of factors affecting outcome beyond biology at the time of injury, such as social and environmental factors. (Bogner, Manley)
The fifth session of the workshop featured three traumatic brain injury (TBI) initiatives that are developing learning health systems (LHS) in an effort to improve TBI research, clinical practice, and clinical operations. Session examples highlighted how Comparing Treatment Approaches to Promote Inpatient Rehabilitation Effectiveness for TBI (CARE4TBI) and TRACK-TBI networks advance research on acute injury and longer-term recovery from TBI and seek to connect this knowledge to improved patient outcomes, while analyses of the Department of Defense’s TBI surveillance dataset provide insights to inform programs and policies for service members. Nsini Umoh, program director in the National Institute of Neurological Disorders and Stroke (NINDS) Division of Neuroscience repair and plasticity cluster, moderated the session.
CARE4TBI: COMPARING TREATMENT APPROACHES TO PROMOTE INPATIENT REHABILITATION EFFECTIVENESS FOR TRAUMATIC BRAIN INJURY
Jennifer Bogner, professor and Bert C. Wiley, M.D., Endowed Chair in the Department of Physical Medicine and Rehabilitation at the Ohio State University (OSU) Medical Center, provided an overview of CARE4TBI,
which is a comprehensive investigation of real-life rehabilitation approaches to identify interventions that are effective at various points in the recovery process.2 Interventions are based on lessons learned from more than a decade of preliminary studies, the infrastructure of the National Institute on Disability, Independent Living, and Rehabilitation Research (NIDILRR) TBI Model Systems program, and stakeholder engagement.3 The CARE4TBI study aims to develop standardized data elements within electronic health records (EHRs) across sites to enable data extraction for research purposes and clinical operations. The study has just begun its next phase, which uses causal inference methods to compare the effectiveness of various rehabilitation approaches. She noted that although CARE4TBI is creating an LHS foundation, the process of becoming a fully functioning LHS is still underway.
Drawing from practice-based data on TBI care, existing projects serve as key components for CARE4TBI, Bogner explained. A 1998 consensus conference on TBI held by the National Institutes of Health concluded that inpatient rehabilitation is effective, though not fully understood, and called for additional research to identify the interventions and other factors responsible for desired outcomes (NIH Panel, 1999). The TBI Practice-Based Evidence study in 10 North American sites provided insight on rehabilitation therapies, their variation, and association with outcomes (Horn et al., 2015). This study provided the preliminary data used to design the CARE4TBI study.
Therapists at each site designed data collection forms to detail the interventions they conducted. They completed these forms in addition to standard clinical documentation, resulting in data with few gaps. Bogner emphasized the value of engaging providers in designing data collection tools, as people are more willing to dedicate time to capturing data that they deem useful. The CARE4TBI study uses the infrastructure of the NIDILRR-funded TBI Model Systems, and 14 of the TBI Model Systems sites are participating in CARE4TBI.
Multilevel stakeholder engagement is critical to the CARE4TBI process, said Bogner. For instance, the Ohio Valley Center Advisory Council (established in 1991) provides input on CARE4TBI and consists of individuals with TBI, advocates, and representatives from the rehabilitation field. Clinicians—including physicians; psychologists; and physical, occupational,
___________________
2 See https://care4tbi.tbindsc.org/default.aspx (accessed January 3, 2024).
3 Funded by NIDILRR, Bogner noted that the TBI Model Systems program is the world’s largest TBI longitudinal database, with over 19,000 participants. For over 3 decades, TBI Model Systems has collected lifetime data on individuals with moderate to severe TBI from 16 inpatient rehabilitation sites. The TBI Model System National Data and Statistical Center provides the infrastructure required to manage a national database of this magnitude and hosts affiliated studies—such as CARE4TBI—enabling linked databases.
speech, and recreation therapists—have redesigned EHR formats to enable their use in research as well as program evaluation. From the outset, the CARE4TBI has been therapist driven, with therapists determining the key elements to capture in the study. Information technology (IT) specialists and EHR platform vendors collaborate in the initiative. Administration, such as rehabilitation leaders and upper hospital management, have enabled the study to effect change by allowing considerable changes within their systems.
Data Capture Standardization
The first phase of CARE4TBI focused on the standardization of EHR data capture, which involved identifying, designing, and standardizing data elements to be collected in session notes and ensuring these are extractable for both research and clinical operations. Bogner emphasized that data from EHR flow sheets are not necessarily extractable, thus flow sheets must be designed for data extraction. The CARE4TBI design considers efficiency for clinical operations by eliminating redundancy in existing data fields, aligning with regulatory requirements, and necessitating as few mouse clicks as possible. Once standardized, each rehabilitation site integrated the data fields into its existing workflow to maximize documentation efficiency. This means that all sites capture the same data elements, although the locations of these elements within the EHR may vary.
The design process prioritized ongoing collaboration with therapists and rehabilitation team leaders to create data elements aligned with therapists’ priorities and a user-friendly data collection structure. IT professionals advised the design team on feasibility and ensured data extractability. The 2-year process of determining data elements and building templates concluded in August 2023. Fourteen sites integrated the templates into their workflow, trained clinical staff, and went live by September 2023. The data elements operate at various levels, with some fields completed at every session and others completed only when relevant. In accordance with medical record documentation standards, entries are limited to the content of sessions, and therapists are not prompted to indicate that an activity did not take place.
The standardization process faced numerous challenges, said Bogner. For example, hospital systems sometimes opt to share the cost of an EHR platform with other organizations. Although this method is effective in decreasing expenses, it reduces flexibility in customizing to a facility’s preferences. For this reason, one site was unable to update the EHR and therefore discontinued participation in the study. Wider adoption of the CARE4TBI data elements within the rehabilitation field would enhance future data collection efforts, she said. The 14 sites that completed the first phase use two
different EHR platforms—Epic and Cerner (major EHR vendors). Thus, the data elements design needed to accommodate both platforms as well as the various customizations that sites may select within each platform. To address this need, OSU built a template for the Epic platform that other sites using Epic could ingest. Each site using Cerner built its own template following CARE4TBI data elements guidance. The sites shared tips with one another to promote efficiency during this process. Additionally, some therapists prefer narrative notes to discrete fields such as dropdown menus. To facilitate the transition to structured, standardized fields, the design includes a comment section for each therapeutic activity. Terminology to describe the same activities varied between therapists. The study made efforts to reach consensus on terminology and allowed for customization at the entry level to the extent that extraction reports remained consistent.
Data Collection and Analysis
Bogner reported that the second phase of CARE4TBI began on September 1, 2023, and will last for 5 years. This phase compares the effectiveness of various rehabilitation approaches in terms of community participation and the functional independence of patients with TBI. Furthermore, the study will identify patient, provider, setting, and postdischarge factors that modify the effect of therapy on outcomes. Researchers will use causal inference methods to analyze data on approximately 1,600 participants over the course of 5 years. Community participation and functional independence outcomes will be collected at discharge, 6 months postinjury, and 1 year postinjury.
TRACK-TBI NETWORK AND NINDS COMMON DATA ELEMENTS
Joseph Giacino, director of rehabilitation neuropsychology at Spaulding Rehabilitation Hospital and professor of physical medicine and rehabilitation at Harvard Medical School, discussed the Transforming Research and Clinical Knowledge in TBI (TRACK-TBI) study in terms of its aims, achievements, and efforts toward becoming a functioning LHS.4 He began by identifying seven levels of care in the United States that—depending on the severity of the injury and length of the treatment course—may be appropriate for people with TBI.5 He described this system as highly fragmented,
___________________
4 More information about the TRACK-TBI network is available at https://tracktbinet.ucsf.edu/ (accessed November 30, 2023).
5 These seven locations and levels of care are the emergency department, intensive care unit, acute care ward, inpatient rehabilitation hospital or long-term acute care hospital, skilled nursing facility, nursing home or other long-term care facility, and community- and home-based care.
lacking centralized management, and requiring navigation to successfully transition between the levels and locations of care; consequently, many people do not receive adequate TBI care and services. The LHS model offers care integration guided by research.
Learning Health System Components
Giacino outlined several components of an LHS for TBI, building on the 2022 National Academies’ TBI report and 2006 IOM workshop. He highlighted the five areas of:
- Engaged Partnerships: Establishing an LHS requires engagement and close collaboration with diverse stakeholder groups, such as federal and state agencies that implement and regulate health service delivery, clinicians, payers, policy makers, individuals living with TBI, and caregivers. Partnerships with stakeholders identify common goals and well-defined roles.
- Harmonized Infrastructure: Harmonized infrastructure involves common data elements that apply to both research and clinical practice, EHR equipped with data capture, and data repositories with international interoperability.
- Standardized Data Acquisition: Standardized data acquisition features systematic, clinical data collection procedures that extend through all phases of recovery, particularly the postacute phase. Standardized outcome measures should be validated within specific contexts of use, such as diagnosis, prognosis, treatment efficacy, and patient stratification.
- Real-Tine Knowledge Access: Real-time access to curated knowledge can be made readily available to users via data visualization methods that facilitate interpretation (e.g., data dashboards) and decision support tools to guide care. Such tools should be easily accessible and meaningful to clinical practice.
- Continuous Learning Culture: A continuous learning culture is likely the defining feature of an LHS and is underdeveloped in the TBI field, he maintained. Such a culture requires LHS champions embedded in all sectors, sustainable education and training protocols, longitudinal assessment, and mechanisms to analyze and refine processes, such as feedback cycles.
These necessary—but not sufficient—LHS components enable a system that can answer questions related to diagnosis prognosis, and treatment, said Giacino. For example, a TBI LHS should be able to address diagnostic queries such as which performance-based TBI assessment measures can
accurately detect mild TBI in adults within 48 hours postinjury. To support prognostication of anticipated recovery trajectory, the system should have the capacity to determine which TBI endophenotypes (subtypes), identified 1 month postinjury, indicate that a person is more likely to remain permanently dependent on others for activities of daily living. Such issues are particularly salient for patients and families as they envision their recovery process. Additionally, a TBI LHS should answer treatment questions such as which treatment is most effective for post-traumatic fatigue persisting longer than 12 weeks after a mild or moderate TBI. These examples highlight the specificity and relevance to patients that a TBI LHS should achieve, he said.
TRACK-TBI as a Learning Health System
A clinical trial network of 19 academic centers, TRACK-TBI features some of the foundational components of an LHS connecting research to care, Giacino said. The project focuses on four aims: (1) the creation of a legacy database to promote collaboration and accelerate TBI research, (2) improved TBI diagnosis and classification/taxonomy, (3) improved TBI outcome assessment, and (4) identification of the health and economic impact of mild TBI. A key objective is moving from the Glasgow Coma Scale (GCS) and Glasgow Outcome Scale to the adoption of a precision neuroscience approach that determines the endophenotypes of individuals with TBI through a combination of symptom reporting, multidimensional clinical data, neuroimaging, and blood-based biomarkers that inform personalized treatment.
Conceived as a public–private partnership, TRACK-TBI has established a diversely populated ecosystem of partners from industry, government, academia, and philanthropy over the past decade and has forged close ties to Europe’s largest TBI study, the Collaborative European Neurotrauma Effectiveness Research in TBI (CENTER-TBI).6 From the start, both projects have harmonized efforts and are using the NINDS TBI Common Data Elements to enable data sharing and, in turn, generate more robust research findings.7 He noted that NINDS is creating a 3.0 version of the TBI Common Data Elements, and this version promises higher measurement precision than previous versions.
Given the variation in severity and symptom trajectory associated with TBI, TRACK-TBI needed a systematic assessment approach for a patient
___________________
6 More information on CENTER-TBI is available at https://www.center-tbi.eu/ (accessed January 12, 2024).
7 More information about the NINDS Common Data Elements is available at https://www.commondataelements.ninds.nih.gov/ (accessed November 30, 2023).
population with a level of function ranging from coma to uncomplicated mild TBI, said Giacino. Furthermore, the assessment must be able to accommodate the changes in level of function expected in the first year post-TBI. The study developed a flexible outcome assessment battery to systematically collect data on every participant at every time point regardless of the severity of impairment. TRACK-TBI has enrolled over 3,100 participants with TBI and more than 600 control participants, half of whom have orthopedic trauma and half of whom are friend controls. More than 3,000 data elements are collected per participant. The project has amassed over 3,200 adult MRI results taken at 2 weeks postinjury and 6 months postinjury to enable comparison. TRACK-TBI has acquired over 42,000 biospecimen samples (e.g., DNA, RNA, plasma, and serum) and performed over 3,200 follow-up exams with patients 2 to 8 years postinjury. This large dataset provides a critical foundation for analysis.
TBI Endpoints Development
Complementing TRACK-TBI and funded by the Department of Defense, the TBI Endpoint Development (TED) initiative created the TED metadataset by curating data from eight previous studies from the military, civilian, and sports sectors, Giacino explained.8 The establishment of this metadataset allows for retrospective data mining in advance of conducting prospective studies. The initiative also conducted studies to validate selected common data elements within their context of use and then conformed these elements to global standards to facilitate data sharing and drug development.
TRACK-TBI Achievements
Giacino reviewed TRACK-TBI research findings and innovations to date, noting how the network’s development of TBI-relevant clinical research tools, such as scoring and classification approaches, software modules, and data standards contribute to the underlying goal of linking research results to improved care through an LHS approach. Drawing on the network’s array of tools and data, TRACK-TBI studies have demonstrated that deficits persist for at least 12 months postinjury in more than 50 percent of people who experience mild TBI (Nelson et al., 2019). Additionally, the risk of persistent functional impairment is highest for those with complicated mild TBI, meaning a TBI featuring a detectable structural lesion. On the other hand, over half of people who sustain severe TBI and
___________________
8 More information about the TBI Endpoints Development initiative is available at https://tbiendpoints.ucsf.edu/ (accessed November 30, 2023).
remain severely disabled 2 weeks postinjury regain partial or full independence within 12 months (McCrea et al., 2021). He remarked that this finding undermines the pervasive nihilism about the prospects for recovery after severe TBI. Among the tools and technologies created via TRACK-TBI efforts, the Glasgow Outcome Scale-Extended (GOSE) is the outcome measure used most worldwide and is accepted by the U.S. Food and Drug Administration (FDA) for use in drug and device trials (Wilson et al., 2021).
This two-way scoring approach allows the investigator the flexibility to include peripheral injuries sustained by a patient in determining the disability rating or opt for a TBI-specific rating that discounts broken bones or other injuries that limit function. This differentiation is significant in determining disability severity, as a GOSE score that includes effects of peripheral injury will improve as peripheral injuries resolve. Although the studies launched at approximately the same time, TRACK-TBI uses the brain-specific outcome measure and CENTER-TBI uses the all-cause injury calculation. Without a mechanism to indicate the method being used, the CENTER-TBI outcomes would appear to be worse than those in TRACK-TBI. Thus, the integration of research was essential in delineating methods and understanding findings.
Additional TRACK-TBI developments include an evidence-based clinical outcome semiautomated Qualtrics platform that allows the validation of outcome measures within their specific context of use, said Giacino (Christoforou et al., 2020). The Clinical Data Interchange Standards Consortium incorporated the TRACK-TBI common data elements into the Therapeutic Area Data Standards in efforts to ensure global standardization (Clinical Data Interchange Standards Consortium, Inc., 2015). TRACK-TBI developed the OsiriX common data element software module, a standardized tool for evaluating MRI scans for TBI. This tool is used to identify imaging features associated with adverse outcomes after mild TBI and has been approved by the FDA for selecting mild TBI patients for clinical trials (FDA, 2019; Yuh et al., 2013, 2021). Most recently, a partnership with Abbott Labs, which developed the iStat Alinity point-of-care device, has enabled test results on TBI blood biomarkers within 15 minutes. Specifically, the glial fibrillary acidic protein (GFAP) and ubiquitin C-terminal hydrolase L1 (UCH-L1) proteins indicate whether a person has likely experienced a structural brain injury and therefore requires imaging (Yue et al., 2019).
TRACK-TBI Progress Toward LHS Realization
Giacino outlined a number of LHS components that TRACK-TBI has established, noting those that require additional efforts (see Figure 5-1).
In terms of engaged partnerships, he said, the project has brought together disparate stakeholder groups with common aims but needs to
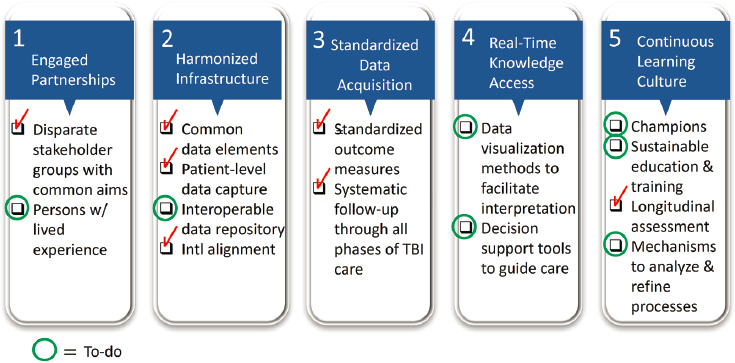
NOTE: Areas achieved so far within the TRACK-TBI network are marked with red checks; green circles indicate areas in which further progress is needed.
SOURCE: Presented by Joseph Giacino, October 12, 2023.
deepen and expand partnerships with individuals with lived expedience of TBI. In working toward harmonized infrastructure, TRACK-TBI has made use of common data elements, patient-level data capture, and international alignment but has yet to establish an interoperable data repository. The network has successfully put the components of standardized data acquisition into place by developing standardized outcome measures and establishing systematic follow up through all phases of TBI care. Real-time knowledge access is currently lacking, given that the project has yet to develop data visualization methods to facilitate interpretation or decision support tools to guide care. Regarding cultivating a continuous learning culture, TRACK-TBI has established longitudinal assessment but has yet to engage additional champions of the effort, develop sustainable education and training, and build mechanisms to analyze and refine processes.
Giacino noted that the LHS components TRACK-TBI has not yet put in place constitute the difference between a system that achieves scientific advances and one that demonstrates real-world benefit from these advances. The former, for example, is capable of determining that a drug strikes a specified target, whereas the latter has the capacity to ascertain who actually takes the drug and whether it improves their health.
TRAUMATIC BRAIN INJURY DATA AND LEARNING SYSTEMS
Katharine Stout, assistant division chief at the Department of Defense (DoD) TBI Center of Excellence (TBICoE) noted that since 2000, over
479,000 service members have been diagnosed with at least one TBI (Figure 5-2) (DoD, 2023). She outlined two examples of DoD surveillance efforts intended to better understand TBI and translate these insights into an improved LHS. Long-range goals arising from this work include the creation of real-time dashboards built into the EHR to aid operational and medical leadership in improving clinical decision making and planning.
To inform awareness and measurement of TBI experienced by service members, DoD established a dataset of TBI occurrences, ICD codes, and approximations of when injuries occurred. Stout noted that DoD currently lacks the capability to track multiple TBIs experienced by a service member because of the International Classification of Diseases (ICD) coding structure used,9 a barrier the department is working to address with partners across other agencies.
Stout shared several examples of how DoD TBI data have been used to inform medical monitoring, training, education. Leadership requested the
___________________
9 The International Classification of Diseases is a system for classifying medical conditions and used for such purposes as clinical record keeping, reimbursement of medical claims, and epidemiological surveillance. https://www.cdc.gov/nchs/icd/index.htm (accessed February 5, 2024).
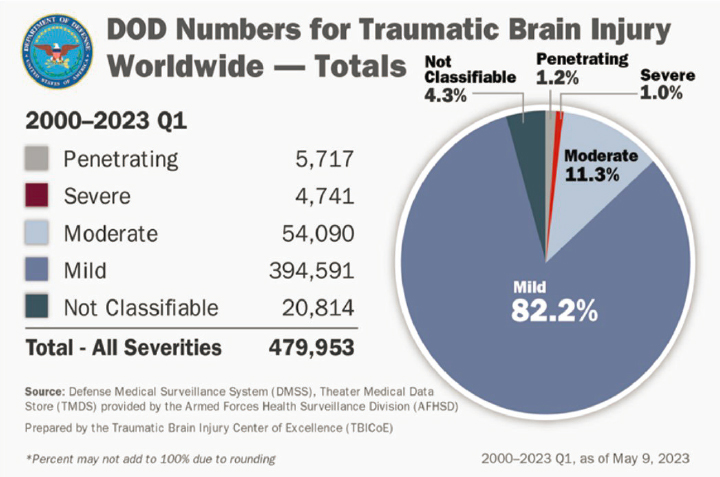
NOTE: Percentages may not add to 100 percent because of rounding.
SOURCE: Presented by Katharine Stout, October 12, 2023. Department of Defense (https://health.mil/Military-Health-Topics/Centers-of-Excellence/Traumatic-Brain-Injury-Center-of-Excellence/DOD-TBI-Worldwide-Numbers).
identification of military occupational specialties at higher risk for TBI. The analysis team cross-referenced service members identified with a first lifetime TBI between 2012 and 2019—numbering over 170,000—with DoD data systems containing occupation codes. Results indicated that Special Forces, Explosive Ordinance Devices units, and some artillery units were at a higher risk for TBI than other occupational specialties. The DoD regional educational coordinator network then targeted leadership in high-risk military occupational specialties to provide Warfighter Brain Health training to improve capacity for early TBI detection.10
Given that the DoD TBI case definition includes an “incidence rule” whereby service members only have one TBI counted per lifetime, Stout emphasized the need, and current efforts to establish, DoD surveillance methodologies to capture service members’ subsequent TBIs. Additional areas to address include identifying service members who have already sustained multiple TBIs and creating management and treatment guidelines for such individuals. Within DoD, emergency medicine providers, first-line responders, rehabilitation providers, and nonmedical leadership have expressed interest and dedication in improving TBI treatment.
Constituting approximately 82 percent of service members diagnosed with TBI since 2000, individuals identified as having mild TBI demonstrate substantial variability in symptom presentation and trajectory, she said. The variety in TBI patterns, conditions, and symptoms poses challenges in triaging and triangulating care. Stout explained that this finding generated interest in improving the ability to identify patients with mild TBI and better predict their outcome trajectories. Both DoD and the Department of Veterans Affairs (VA) are currently working to introduce new data systems that connect to one another to improve the usefulness of the EHR for providers. TBICoE is examining how data from the system can be made actionable by prompting recommendations, treatment plans, and fact sheets for providers and making information available for patients with the aim of helping service members efficiently navigate treatment to return to their jobs and families to the greatest extent possible.
The surveillance team analyzes TBI data and reports on incidence, comorbidities, trends, and other results to inform military leadership (e.g., Agimi et al., 2018; Hai et al., 2023). A recent analysis described by Stout looked at comorbidities in military-sustained mild TBI by first identifying over 42,000 service members who experienced a first lifetime TBI between 2016 and 2019. Conducting a review of literature and TBI expert consensus, the surveillance team identified 18 conditions that often co-occur with mild
___________________
10 More information at the Warfighter Brain Health Initiative is available at https://media.defense.gov/2022/Aug/24/2003063181/-1/-1/0/DOD-WARFIGHTER-BRAIN-HEALTH-INITIATIVE-STRATEGY-AND-ACTION-PLAN.PDF (accessed December 1, 2023).
TBI: alcohol and substance use disorders, anxiety disorders, cervicogenic disorders (e.g., perception of pain or dizziness arising from the neck), cognitive disorders, depression and other related conditions, headache and related conditions, hearing conditions, nausea/vomiting, neuroendocrine disorders, other neurological conditions, post-traumatic stress disorder (PTSD), other psychiatric conditions, psychological conditions, seizure-related conditions, sleep, suicidal and homicidal ideation, vestibular conditions, and visual disturbances. Stout highlighted the painstaking work involved in reviewing ICD codes and categorizing conditions. Researchers analyzed service member data records for conditions that were present 180 days prior to TBI diagnosis and those that appeared within the first 180 days postdiagnosis. She reported that over 77 percent of service members with mild TBI had at least one co-occurring condition, noting that 81 percent of the analyzed population were male, 64 percent were white, and 74 percent were younger than 34 years old. During the 180 days prior to TBI, the most frequently reported conditions were sleep-related conditions (21.7 percent), headache (19.4 percent), PTSD (17.8 percent), anxiety (11.3 percent), cervicogenic disorders (10.9 percent), and nausea/vomiting (7.7 percent). During the 180 days following mild TBI diagnosis, the prevalence of diagnosed conditions increased significantly, with visual disturbances and cognitive conditions increasing by over 300 percent, vestibular conditions increasing by 193 percent, headaches by 152 percent, and hearing-related conditions by 73 percent. Sleep-related conditions and anxiety disorders were moderately positively correlated with mild TBI. The period prevalence estimates of PTSD (30.1 percent) and depression and relation conditions (11.9 percent) among service members with mild TBI were higher than the 5 percent prevalence among nondeployed service members and 8 percent among combat deployment.
The findings confirmed anecdotal reports from providers, Stout said, and can aid in refining clinical recommendations and provider and patient education efforts. Given the busy schedules of care providers, information that offers clinicians specific symptoms to look for makes implementation of recommendations more manageable.
Stout also outlined several limitations to the findings. For example, conditions such as PTSD and suicidal ideation are likely underreported by service members because of associated stigma, and the presence of undiagnosed mild TBIs or other undiagnosed conditions could also contribute to underestimation of co-occurring conditions, particularly given that repeat TBIs are omitted by current DoD surveillance methodologies. Furthermore, assessment of service members with newly diagnosed mild TBI may uncover existing comorbid conditions not related to TBI. Additional efforts are needed to further understand the interplay of comorbid conditions to enhance provider ability to triage, treat, and move patients through the appropriate trajectory of care.
DISCUSSION
Developments in Care, Research, and Learning Integration
Umoh asked about advances that have been achieved in TBI treatment and recovery through integrated linkages between care, research, and continuous learning. Bogner replied that foundational work for CARE4TBI identified some approaches most likely to effectively improve outcomes. Implementing these approaches does not necessitate changes to the natural rehabilitation environment, she said, but rather a shift in emphasis. For example, when therapists perform activities relevant to daily life with patients during inpatient sessions, patients are more likely to resume normal activities outside of the home 1 year postinjury than when therapists focus on clinic-based activities. She stated her hope that CARE4TBI will generate more nuanced guidance as the project moves forward.
Giacino noted two initiatives underway that can contribute to the further development of TBI LHSs. He noted the TBI forum’s ongoing action collaborative on TBI care. Members of the action collaborative are currently focused on fostering and disseminating best practices, care models, and more integrated care systems for people with suspected TBI who are released from the emergency department (ED). These individuals may not be connected to any follow up care, although many experience ongoing symptoms. Additionally, the Biomedical Advanced Research and Development Authority is conducting an aid-in-diagnosis trial to validate the use of blood-based biomarkers for TBI detection. How to establish LHS feedback loops and iterative learning as these and other advances move into clinical application will require future consideration, he noted. Beth McQuiston, neurologist, dietitian, and medical director of diagnostics at Abbott Laboratories, noted that this aid-in-diagnosis trial is being conducted in partnership with Abbott to study TBI biomarkers used on a core laboratory platform, which would also integrate into a system’s EHR for use in assessing TBI severity level.
Stout described a DoD instruction that represents a paradigm shift for service members with acute concussion or potentially concussive events who are being discharged from the ED or from “sick call,” the military equivalent of urgent care. Rather than instructing patients to follow up for care if certain symptoms present, the policy specifies a follow-up visit within 72 hours. This practice enables early identification of TBI patients who become symptomatic after the initial care visit. Aligning with the Military Acute Concussion Evaluation 2 and Progressive Return to Activity Following Acute Concussion tools,11 this policy represents a substantial change
___________________
11 For these tools, see https://health.mil/Reference-Center/Publications/2020/07/30/Military-Acute-Concussion-Evaluation-MACE-2 and https://health.mil/Reference-Center/Publications/2023/01/23/Progressive-Return-to-Activity-Primary-Care-for-Acute-Concussion-Management (accessed January 12, 2023).
in practice and has met some challenges in implementation. For instance, clinic schedules require flexibility to allow for follow-up visits within 3 days. TBICoE is working closely with medical affairs at the Defense Health Agency to refine the policy and its metrics.
Another forthcoming paradigm shift involves moving from a predeployment mandate for neurocognitive assessment testing to assessment over the lifetime of a service member. This shift is expected to improve assessment accuracy and collect objective measures on service members that generate real-time data. In developing the capacity to rapidly use findings to aid service members in returning to full duty to the greatest extent possible after TBI, this development can move the system toward full realization as an LHS.
Challenges in Establishing a Learning Health System
Two substantial challenges in shifting DoD toward becoming an LHS are behavior change and adoption of new tools, Stout asserted. The department is using feedback loops to address these challenges. For example, practitioners in the field expressed the desire for greater accessibility of the tools than the current PDF format. TBICoE is working with IT to house the tools within a mobile application and make it possible to download the tools onto mobile devices to use when wireless Internet service is unavailable. This format will increase ease of use within the clinical setting. Additionally, efforts are underway to integrate the tools into the EHR to increase adoption in the clinic and enable data capture. This change will move away from text paragraph fields to radio buttons to allow providers to indicate a patient’s symptoms and functional levels without typing. This development is intended to decrease provider time spent on documentation and increase data capture fidelity. She emphasized that soliciting and acting upon feedback from stakeholders improves practice, generates better data, and opens communication. Bogner noted a past challenge in assessing implementation, as CARE4TBI issued recommendations to therapists but lacked data on adoption. Use of the standard data fields generates practice data that inform implementation assessment. Establishing the ability to rapidly receive data and translate it into a visual format that clinical providers can use in decision making is a current challenge.
Lessons Learned
Highlighting the complexity of large systems, Bogner noted her surprise at the heterogeneity in electronic health record platforms across different sites. Additionally, much of the documentation that providers enter into the EHR is aimed at supporting clinical use but is not provided in a format that can be evaluated to improve clinical operations and outcomes across
an organization and system. Current data at most rehabilitation facilities are merely a record of the treatment that occurred and cannot be used for program evaluation or examining outcomes, she said. Many sites have done little more than transfer paper forms into electronic systems, and thus most electronic health systems have yet to collect data in a format that can be used to improve patient outcomes. Stout noted the challenge of creating systems that effectively capture outcomes, aggregate data from multiple datasets, and provide real-time data to clinicians in a format that improves care. Current data are disjointed and do not offer providers a clear navigation path. Using a football analogy, she said that improving the TBI “playbook” for providers would increase their ability to become “star quarterbacks” who help patients navigate to best possible outcomes.
Giacino remarked that building improved infrastructure will enable access to better care. The knowledge gained over the past decade eclipses that of the 30 years prior, he said, and technology and data sharing between large networks can accelerate the learning process. He emphasized the importance of including all stakeholders as LHS initiatives are designed. Describing TRACK-TBI as slower to incorporate patients up front in development, he underscored the critical value of lived experience and also stated that engagement of payers is key in LHS discussions and the creation of new payment models.
TBI Prevention
Kristine Yaffe, director of the Center for Population Brain Health at the University of California, San Francisco, asked how an LHS can improve prevention efforts, given the high rates of PTSD and sleep impairment prior to TBI and that a prior TBI constitutes the biggest risk factor for experiencing another TBI. For example, a data dashboard could potentially assess TBI risk similar to fall-risk calculations for older adults. Bogner stated that prevention is critically important and must start with primary care providers. Stout remarked that TBI prevention efforts should extend within medical operations and beyond the health care system to the education system. Work conducted on exposure risk via section 734 of the National Defense Authorization Act for Fiscal Year 2018 led the military operational and safety communities to issue a safety memorandum regarding the TBI risk posed by blast exposure.12 Efforts are underway to determine a definitive marker for TBI on blast gauges.
In the meantime, the safety memo states that service members with exposure to pressure greater than 4 pounds per square inch should be con-
___________________
12 National Defense Authorization Act for Fiscal Year 2018, Public Law 115-91, 115th Cong., 1st sess., (December 12, 2017).
sidered at high risk for a potentially concussive event. She emphasized that this guidance was an operational initiative, rather than a medical one. Prevention efforts for TBI could resemble those for diabetes, in which standard annual physical exams include the hemoglobin A1C test—an early marker for diabetes—and a certain A1C level triggers diabetes education efforts. Given the broad nature of TBI as a medical condition and its intersections with, for example, occupational safety issues, TBI prevention necessitates participation of communities beyond medical and rehabilitation professionals, said Stout.
Culture Change
Corinne Peek-Asa, vice chancellor for research at University of California, San Diego, asked about opportunities and challenges involved in structural and cultural change. Giacino remarked on the difficulty of shifting culture and noted he is beginning a grant-funded implementation project focused on culture change. Identifying what constitutes an LHS champion, who these champions are, and how they will function is important to cultural transformation, he said. This change process requires a mechanism to ensure that change efforts are ongoing and sustained. Such a mechanism involves human resources, which come at a cost. However, his review of literature indicates that efforts that do not aim for culture change from an initiative’s start are likely to fail. Focus groups can be used within the TBI field to better understand the barriers and facilitators to care encountered by patients and caregivers. Incorporating the perspective of end users into the system design can shift culture to better meet the needs of individuals with TBI.
Emergency Medical Services TBI Data
Bruce Evans, immediate past president of the National Association of Emergency Medical Technicians, remarked that the National Emergency Medical Services Information System database is not relational to other health care databases. Thus, data collected by emergency medical services (EMS) on TBI patient encounters are not connected to Epic or other EHR databases and undermine the ability to perform longitudinal assessments. Moreover, EMS can directly affect the cost of TBI care, particularly if EMS providers deliver a patient to the wrong level of trauma care, discharge the patient, or allow a patient to become hypotensive, hypothermic, or hypoxic. He asked how databases can be better connected to improve longitudinal assessment. Bogner replied that the TBI Model Systems program performs lifetime tracking of TBI patients who receive inpatient rehabilitation services.
Currently, the program is monitoring individuals 35 years postinjury. In the past, TBI Model Systems datasets included EMS data; however, this was ended because of the issues Evans raised. She described the disconnection between EMS data and other medical system databases as problematic, disrupting the ability to conduct long-term follow up on all TBI patients who receive EMS care. Stout commented on the variety of data systems across DoD environments and roles of care. An effort is currently underway to aggregate data, but legacy systems present challenges with variance in data fields and data fidelity. Giacino noted that probabilistic matching techniques can be used to match identical patients within two separate databases that do not communicate. The National Traumatic Databank and TBI Model Systems conducted probabilistic matching with some success, he said.
Payment Models for TBI Care
Giacino underscored the challenge of integrating an LHS with payment models. Many people in the United States receive excellent acute care for TBI and then encounter a care gap after discharge. Many people with a moderate-to-severe TBI do not receive comprehensive inpatient rehabilitation services, he said. Those who do receive this care are typically limited to 19 days of inpatient rehabilitation, and many people are discharged in an acute state of confusion. Noting the programs for postacute care in Massachusetts that have been shut down because of lack of funding, he emphasized that best practice will only be implemented if supported by payment models.
Donald Berwick, president emeritus and senior fellow of the Institute for Healthcare Improvement, raised the possibility of constructing payer structures to propose to the payer community that would outline needed changes, the patients’ needs that such changes would meet, and cost. He asked about the feasibility of this approach. Giacino remarked that rehabilitation services are limited by a “3-hour rule” from the Centers for Medicare and Medicaid Services (CMS). This rule limits the authorization of admission to inpatient rehabilitation to individuals who are able to actively participate in rehabilitation services for 3 hours per day. However, the neurobiology of severe TBI often does not allow that level of activity. Commercial payers often impose the limits set by CMS. He noted that his institution abides by this rule because of payment ramifications, and that it impedes access to care for many TBI patients, particularly those who require inpatient rehabilitation after discharge from the acute care hospital. Addressing such barriers could increase access to needed care.
Bogner commented that little to no evidence supports the 3-hour rule. Research indicates that the content of the therapy and extent to which the
participant engages is responsible for improved TBI outcomes, rather than a specified time spent participating. Giacino commented that talks with commercial payers about the benefits of even limited participation in inpatient rehabilitation for TBI patients have stalled once cost entered the discussion.
Odette Harris, professor of neurosurgery at Stanford University and deputy chief of staff for rehabilitation at the Veterans Affairs Palo Alto Health Care System, stated that cost is central in treatment coverage. Given that VA is not bound by the restrictions set by CMS, the requirement of 3 hours active participation has been lowered at some VA polytrauma sites because of the lack of evidence supporting clinical relevance of this threshold on outcomes. However, when cost implications come into play, blame is often attributed to those who made the determination to offer the rehabilitation services. She added that a comparison of patients who meet the threshold for the 3-hour rule and those who do not failed to reveal any differences in outcome. Geoffrey Manley, chief of neurosurgery at San Francisco General Hospital and vice chair of neurological surgery at University of California, San Francisco, emphasized that many patients will be unable to access the interventions they need to fully return to their families and jobs without changes to this 3-hour rule.
John Corrigan, director of the Ohio Valley Center for Brain Injury Prevention and Rehabilitation, commented that the Forum on Traumatic Brain Injury should address insurance-related barriers and could look to other countries in doing so. For example, Australia and New Zealand do not rely solely on health insurance to cover costs and have spread financial responsibility to accident insurance. Payment model reform would benefit government sources, given that individuals with poor TBI outcomes are more likely to require government assistance in the forms of Medicaid and Medicare.
TBI Classification
Berwick noted that the National Academies of Sciences, Engineering, and Medicine’s 2022 TBI report indicated that categorizing TBIs as mild, moderate, and severe could impede insights to progress (NASEM, 2022). He asked whether efforts to move away from this categorization method are still deemed necessary. Bogner replied that the current classification system does a disservice to individuals who sustain TBI. Regardless of whether the terms mild, moderate, and severe are used, an improved TBI classification system could extend beyond a medical model to incorporate the effects of environment and community on a patient’s ability to recover. This shift would acknowledge that outcomes are not only affected by the extent of injury, but also by the supports an individual can access during recovery.
Manley remarked that during patient interviews across the country, patients and families shared that they do not want the “mild, moderate, and severe” labels used. Some family members refused early withdrawal of life-sustaining therapies for their loved ones with severe TBI, and now those patients have not only survived, but have returned to work. Others were labeled by the ED as having mild TBI and have since been unable to work. Thus, this terminology can create bias in expected outcomes. In January 2024, NINDS hosted a workshop on TBI classification and nomenclature that examined the current classification system and considered factors beyond the biology on the day of injury—reflected in GCS score, blood-based biomarker level, and computerized tomography scans—to factors in the biological, psychological, social, and environmental model. Echoing Bogner, he noted that biology at injury does not dictate outcome trajectory. Rather, factors including social setting, environment, treatment interventions, and qualification for rehabilitation services form a complex web that affects outcome and thereby requires a comprehensive approach to TBI care and recovery.



















