Improving Access to High-Quality Mental Health Care for Veterans: Proceedings of a Workshop (2023)
Chapter: 5 Opportunities for Improving Mental Health Care Through Partnerships
This chapter highlights examples from several health systems taking a population health approach to scaling mental and behavioral health care delivery and leveraging community-level partners for improved access to care as well as national-level industry partnerships and contracts.
POPULATION HEALTH APPROACHES
Dawn Zieger, vice president of psychiatry and behavioral health at Geisinger Health, a health system based in Pennsylvania, discussed how it has applied population health principles to creating partnerships to improve access. She saw a rapid increase to 18,000 patient referrals waiting for mental health care during the COVID-19 pandemic. Zieger described seeking out partners to rapidly scale behavioral health access, while also making plans to transform the system. After evaluating multiple groups, Geisinger selected Iris Telehealth to design an integrative health system approach; they were able to add 53 new providers in 2022, which helped tremendously to address the shortage. The new system enabled a referral from any community to any provider nationwide. However, the next steps as Geisinger continues to develop its mental health program are to localize virtual care, bring that to the national workforce that was hired, and enable better co-management and relationship-building between teams.
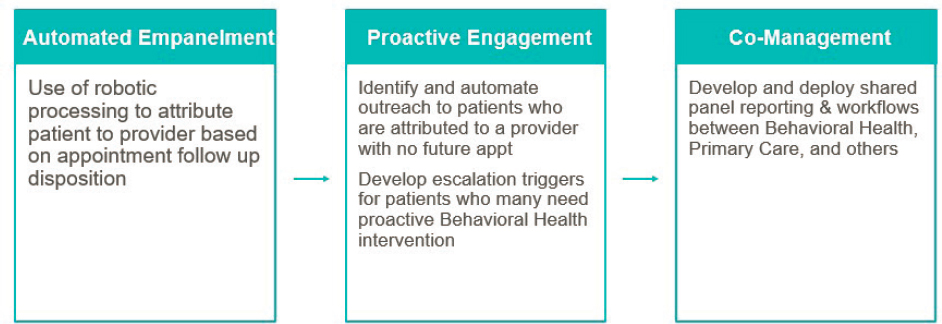
Zieger discussed Geisinger’s different approaches, starting with strong individualized care plans. It also plans to move toward panel-based care, which will help with assessing key metrics for patients in behavioral health to improve quality and decrease interprovider variability. At the population level, the system will be able to better identify patients not seen in behavioral health, including those who make repeat visits to the emergency department for substance use or underlying conditions. This will allow Geisinger to proactively identify when people are escalating and stabilize them more efficiently, she said. Zieger also described plans for a model that can add behavioral health providers to their own panel and leverage digital “workers” to create data linkages and track relationships over time (see Figure 5-1).
Zieger said Geisinger wants to be able to track impact, improve health outcomes, and decrease cost of care. She acknowledged that this would be a long journey—and it is just getting started with the data mechanics—but once the foundation is built, significant improvement is within reach.
Focusing on Underserved Populations
Wes Williams, vice president and chief information officer of WellPower, Denver’s community mental health center, emphasized some key points from his perspective as a behavioral health care specialty provider. WellPower was
SOURCE: Dawn Zieger presentation, April 21, 2023.
created to provide intensive case management and assertive community treatment for people with serious mental illness but also focuses on residential treatment and psychosocial rehabilitation programs. The workforce includes more case managers than any other profession, but it is expanding peer services. He explained that peers play a critical role in treatment and rehabilitation, and people who have successfully advocated their own lived experience with mental illness can be a comforting addition to a care team.
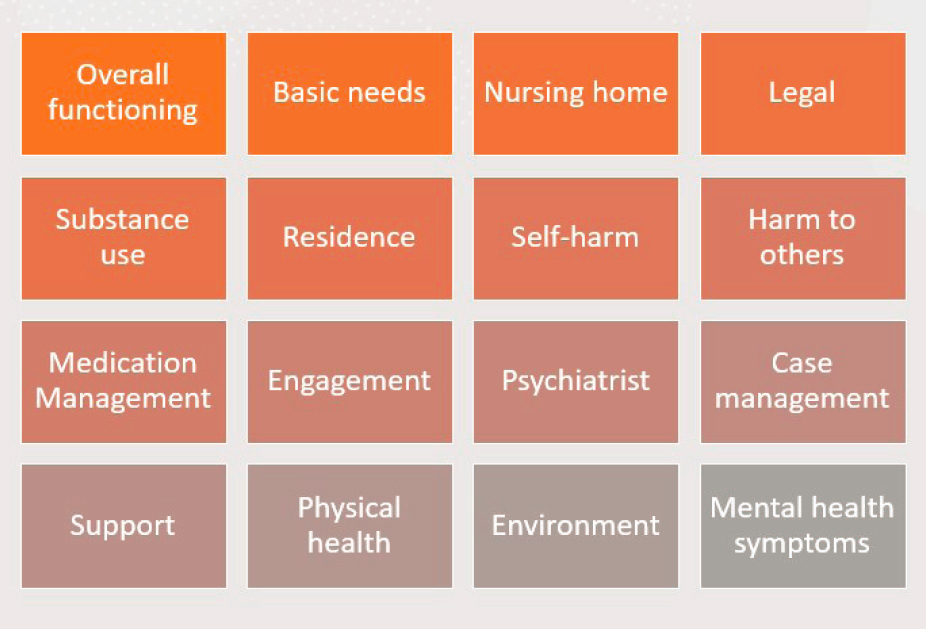
By the time patients arrive, said Williams, they already know they need treatment, so instead of using some of the standard screening tools, WellPower developed an instrument (Recovery Needs Level) to assign the right level of service intensity. This assesses someone’s need for care on 16 dimensions (see Figure 5-2) and compiles a risk score. WellPower also works proactively to partner with city organizations and implement telehealth kiosks across the community, such as in schools, homeless shelters, or dance companies.
Patients with the greatest needs participate in assertive community treatment. For this level of care, each case manager has a caseload of about 14 people that they meet with every week, though a majority of their time is spent out in the community. When individuals improve, they are stepped down to intensive case management, which yields some financial savings, Williams explained. He said the Recovery Needs Level tool is useful because they can repeat the assessment and see what level of care is really needed. As people improve, there are different titrated levels of care, he said (see Box 5-1). Williams suggested VA would benefit from these principles on staffing a behavioral health population with complex needs and extend it to partnerships with community providers to reach more people.
SOURCE: Wes Williams presentation, April 21, 2023.
LEVERAGING INDUSTRY PARTNERSHIPS
Taft Parsons III, chief psychiatric officer at Aetna/CVS Health, described some of the initiatives CVS Health established over the past few years to address a specific high-needs population. Given the shift of many providers to virtual spaces, he said, it has been working to integrate that care with what most are familiar with in person. The whole of CVS conducted fewer than 200,000 visits virtually in 2019 but 30 million virtual visits nationwide since then. This is great for mental health, he added, as it increases access to telepsychiatry and allows for more integration with primary care. Parsons noted that although creating telehealth infrastructure allows for a better distribution of providers, especially for people in rural areas, it does not create new providers. Workforce problems will persist because of the estimated increase in demand but decrease in adult psychiatrists (HRSA, 2020).
Another challenge, Parsons discussed, is that a lot of the recent venture capital investments into health care have incentivized growth but not always quality of care. He explained that this means it becomes even more important to vet and be aware of the quality of care in emerging programs and companies. To maintain strong oversight for this, Parsons described CVS Minute Clinic’s work to build in-person locations and virtual behavioral therapy infrastructure. Patients can go in person to receive care in 14 states and have virtual visits for both therapy and psychiatry in all 50 states. CVS Health has found that people are often willing to forgo immediate access in favor of choosing the provider they want to see at a convenient time. Parsons said that Minute Clinics also ensure their providers are trained in evidence-based practices such as trauma-informed care, stress management, substance abuse, and group therapy.
Bringing this together for a specialty population, Parsons reviewed a recent CVS goal to reduce members’ suicide attempts by 20 percent by 2025. Using various streams of data and multiple variables, it worked to develop a self-harm predictive model. For those identified as high risk, CVS worked with community partners to provide more intensive harm-reduction care and educate behavioral health providers on suicide prevention. It has also developed ancillary programs. One of these, “Caring Contacts,” reaches out to patients if they have been to the emergency department or admitted to the hospital for a suicide attempt to ensure they are connected to services. The rest of the strategy centers on developing targeted public education tools and programs, working with community advocacy groups, and creating resources for youth, parents, and teachers. CVS first started collecting Caring Contacts program data in 2022, and Parsons said it has made progress among the adult population with its specific interventions but has not yet seen the same progress among adolescents.
Williams added that his team has also been working on a zero-suicide quality improvement initiative that similarly uses Caring Contacts and a screening protocol. They leverage data across systems to trigger the care team and flag records as high risk. But the challenge is being able to remove that flag once a person is no longer high risk, he added. Zieger added that Geisinger has uncovered related findings regarding the child and adolescent population, so it is also working to create a more on-demand response system for when someone is in crisis.
DISCUSSION
The presenters discussed ways to identify veterans who may not be in the system, veterans who may be using other community providers, the best ways to leverage partners for veterans, and the potential for optimizing data and technology to improve access.
Identifying Veterans and Coordinating Across Systems
Parsons referred to the Perfect Depression Care1 program within the Henry Ford Health System in Detroit, saying that during his work there, it found that most patients who attempted suicide had visited their primary care provider within the past 30 days. The interventions were delivered in primary care settings, not in behavioral health, which could be applied to the veteran population. Williams added that the assessment at WellPower asks about veteran status, but one of the tensions in the community is that state regulations mandate collecting a 19-point psychosocial assessment for everyone at intake, and in the context of a provider shortage, it is a lot of time and work that could be spent directly with the patient. Williams mentioned trying to find areas of compromise and solutions. For example, people who have a scheduled visit for a briefer intervention may not need the full history workup—but it is a balance to find the right levels of assessment and intervention.
Another question highlighted the challenge of dual users of the VA system and other care delivery systems and how best to coordinate their care. Zieger said that Geisinger has the end-to-end service delivery structure in many markets, which is helpful for maintaining awareness, and if it is not the primary provider, it has a health information exchange (HIE) that can be leveraged to do some assessment across multiple organizations. But data sharing at the system level is foundational to integrate effectively, she emphasized. Williams
___________________
1 See https://pubmed.ncbi.nlm.nih.gov/17441556/ for more information on the Perfect Depression Care program (accessed June 12, 2023).
said he wished that data exchange could solve the problem; unfortunately, it has not been that impactful at WellPower. Working with care teams on the ground has been more effective. Another idea is to create shared registries, so all organizations may be able to know the 1,500 or so people who are common to both organizations and help determine which people have the greatest need. Parsons added that data sharing between providers and payers has been difficult to do in his experience working across three large health care organizations (CVS Health, Molina Healthcare, and Humana), with a lot of variation across the country. HIEs are helpful, but even those have variability.
Partnerships to Improve Access to Mental and Behavioral Health
Zieger said that Geisinger is aiming to engage partners to improve access to mental health care, but it will not be achieved overnight. Zieger said it onboards contracted providers; they know they are part of an integrated delivery system, but the nuance of understanding culture and language of the system is the next step in terms of localization of telehealth delivery. It will be important for providers, even if delivering care virtually, to know what the local culture is like. For example, they can understand their patients by visiting an aging coal town to see its dynamics or reading the local newspaper to learn about the environment and community. Zieger added that Geisinger tries to reduce the lag between hiring and start dates by paying for this onboarding time. Williams said WellPower provides “hope” training to clinicians at the beginning of employment to teach that people can successfully recover from mental illness. He also described its partnership with the Denver Department of Public Safety, which dispatches clinical social workers to 911 calls with police officers. This program has grown from eight clinicians at its inception to around 50, though it has more room for growth. It does take time, Williams acknowledged, and it may take at least 5 years to really see a cultural shift in a community partner. Parsons added that appropriately matching providers with patients has been challenging, as many new providers will check every box to say they are familiar and proficient in all topics; but if veterans are really looking for someone well versed in the military experience and relevant issues, they need a provider who can truly match that.
Optimizing the Use of Data and Technology
In response to how to define and measure access to treatment, Williams said that in practice, it is usually easier to step someone down to a less restrictive level of care. When people’s lives are falling apart, it generally does not happen at clean 6-month intervals, which makes data messier and makes it
difficult to define how a person is functioning or what kind of additional treatment or care they might be receiving from a case manager. Williams explained that WellPower measures how many people can get an appointment within 7 days of making a request and how many are seen within 7 days after discharge from a psychiatric hospitalization, but he noted several limitations. Several same-day appointments are available, but they fill up by 8:45 am every day. Zieger noted a lot of complexity in process metrics. Geisinger is making a fundamental shift that feels like an outcome metric, asking patients if they received care when they needed it. Parsons said that Aetna and CVS Health have a very incomplete dataset—the larger virtual providers they work with track the timelines of people securing appointments, but challenges across different states exist even within the two companies. He noted the lack of a good line of sight in general therapist shops that are part of the network but that do not require a referral, so a timestamp is typically unavailable on how long it took patients to get into them.
Presenters also discussed the AI and other technology tools they are using to identify patients at risk or who may need certain services. Williams described three AI initiatives under consideration: (1) using smartphone passive monitoring, where people leverage their own data; (2) NLP joining telehealth sessions so that the AI can produce the therapy note to save time; and (3) structuring narrative data in charts and mining clinical progress notes. With this third initiative, he said, they are hoping to develop more robust models for identifying who should be on that zero-suicide pathway. Parsons agreed AI has a lot of potential right now but viewed it still as the wild west for the next few years, as many of the tools still cannot distinguish good information from bad. At this point, Aetna and CVS Health are going to stay conservative on how to roll these tools out, he said, because consequences for someone in crisis can be severe. In closing, Zieger shared that Geisinger is taking a more tactical approach, because in addition to the clinician shortage, front desk staff and other support staff are also limited. To leverage technology for this gap, Geisinger has been using robotic processing for things such as no-show communications, appointment updates, and other administrative communication.







