Understanding the Introduction of Pathogens into Humans: Preventing Patient Zero: Proceedings of a Workshop (2026)
Chapter: 5 Interventions for Prevention and Mitigation
5
Interventions for Prevention and Mitigation
Highlights of Key Points Made by Individual Speakers*
- When you want to target a behavior, it is important to understand the incentives for the behavior. (Gurley)
- Rigorous studies are needed to assess whether a behavior can be changed and should allow determination of positive and negative effects. (Gurley)
- True point-of-care tests should be available to ensure people can get tested in their communities. (Agogo)
- If we are serious about being able to diagnose patient zero, we need to work on equity in diagnostics. (Agogo)
- People must be integrated into the concepts and executions of nature-based solutions and not just seen as the drivers and beneficiaries. (Reaser)
- Reducing infections and disease in animals also helps control transmission into humans, and focus should be on high-risk animals. (Swayne)
- Laboratory biosafety and biosecurity is an international problem, which should be reflected more in policies. (Gronvall)
- The conservation community needs to find ways to better integrate into health sciences and bring One Health from their discipline into other relevant disciplines. (Reaser)
* This list is the rapporteurs’ summary of points made by the individual speakers identified, and the statements have not been endorsed or verified by the National Academies of Sciences, Engineering, and Medicine. They are not intended to reflect a consensus among workshop participants.
The fourth session of the workshop focused on interventions for prevention and mitigation. The session was moderated by Andrew Clements, from the U.S. Agency for International Development (USAID).
SOCIETAL FRAMING FOR BEHAVIORAL INTERVENTIONS
To implement behavioral interventions to prevent spillover, said Emily Gurley, Johns Hopkins University, evidence that a behavioral target is amenable for intervention is an important starting point. Under the best-case scenario, she added, multiple investigations over different times and locations would demonstrate a causal relationship between that behavior and a spillover infection, and a mechanistic understanding of the spillover event. In reality, investigations are limited by sample size, and behavior can be ubiquitous in a community, making it challenging to identify a causal association. Gurley explained that the greater the specificity of the behavioral target and the strength of the association to an outcome, the better the chance of developing an intervention. Gurley presented a framework for behavioral interventions (Figure 5-1) drawing from examples of work focused on Nipah virus spillover in Bangladesh.
In 2004, date palm sap was suspected to be associated with spillovers of Nipah virus from bats to humans in Bangladesh. This sap, which is a local delicacy, is collected in a pot under a tap placed in a tree. A 2005 study later confirmed that date palm sap contaminated by Nipah virus–carrying bats that consume the sap during the collection process was the transmission pathway for Nipah virus infections in humans (Luby et al., 2006).
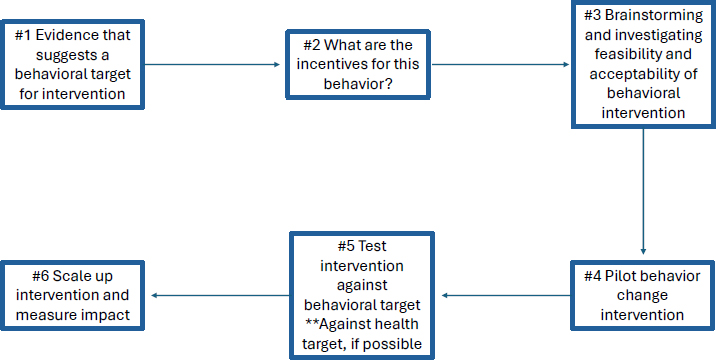
SOURCE: Presented by Emily Gurley, January 15, 2025.
In 2011, there was another large outbreak of Nipah virus infections driven by consumption of contaminated date palm sap. At this point, researchers and public health practitioners in Bangladesh have widely accepted that date palm sap collection was a behavior that should be targeted for intervention to prevent further Nipah virus infections (Hegde et al., 2016). When developing a behavioral intervention, Gurley noted, it is important to understand the economic incentives and the social importance of the targeted behavior. The research team conducted observations and in-depth interviews with local community members to evaluate potential causes for the outbreak (Khan et al., 2012). Researchers lived in villages for 3 months to get to know people and understand their context in order to develop interventions. This revealed that bats are considered a nuisance within the local communities, as they drink palm sap from the collection pots and sometimes defecate or drown in the pots, reducing the quality of the sap.
With this information in hand, Gurley and team investigated the feasibility and acceptability of behavioral interventions (Nahar et al., 2017). Community awareness and education are often used as interventions, and while this can be very important, Gurley noted that these strategies alone may not result in behavior change. Spillovers are rare, so people’s individual risk perception of a spillover is generally low. Therefore, there is no incentive to enact prevention measures, and there can be misalignment in who is expected to take up the desired behaviors and who benefits from the action. She noted that new regulations or media messages should be relied on as much as possible if they have the potential to lead to behavior change, since behavioral interventions are difficult to scale. However, individual and intensive interventions are usually the most effective in promoting changes in a target behavior, she said.
Gurley noted that policy interventions can potentially be effective, but success depends on context. In 2011, the government of Bangladesh changed its policy and local communications to warn local communities to abstain from drinking sap, but these warnings and guidance were ineffective in altering behavior. Gurley and team identified another possibly acceptable and feasible intervention for behavior change, in which the sap collection pots were covered with a bamboo skirt to prevent contamination by bats. Some of the communities engaged in sap collection were already using these to protect sap from being consumed by bats. Therefore, the intervention seemed feasible and acceptable. A pilot study was performed to determine whether use of bamboo skirts was acceptable and effective, and whether there were potential harms and risks of the intervention (Khan et al., 2012). This pilot study evaluated several factors to determine feasibility of using the skirts, including how disruptive the use of skirts was to the workflow of collecting sap and the economic and labor costs of making and installing
the skirts. Potential harms like stigma to the sap harvesters, overburdening of their workflow, and potential cobenefits were also assessed.
The testing phase then began after the pilot phase, Gurley explained. Ideally the intervention is tested in a way that could show whether it reduces spillovers. Rigorous studies are required to assess whether behavior was influenced by the intervention, and whether the intervention had a measurable effect. Further, the magnitude of the response needs to be measured, as these factors will drive decisions about whether an intervention will be used, she continued. Several trials were performed, which showed that the skirts kept the bats out of the pots, and people were twice as likely to report drinking sap that was harvested from a protected source (Khan et al., 2012).
The next step, Gurley said, is scaling up the intervention. There is a need to demonstrate changes in health outcomes, and the longevity of support and funding for an intervention should be tied to evidence. There also is a need to keep evaluating potential harm, she said. In the case of bamboo skirts, cost was prohibitive for a scale-up initiative. Therefore, the government considered implementing a cost-effective mass media campaign using posters and videos (Nahar et al., 2017). As this was not the intervention that was studied, it was unclear whether it would be effective in reducing disease transmission. In the end, no long-term funding was available as there was no government support. Overall, Gurley concluded the framework (Figure 5-1) shows a lot can be done at each stage to keep moving ahead with behavioral interventions, but that many challenges can preclude large-scale implementation.
DIAGNOSTICS FOR EARLY WARNING
The journey from patient zero to an outbreak is moderated by many factors, Emmanuel Agogo, Foundation for Innovative New Diagnostics (FIND), explained. These include cultural, social, and health system factors, in addition to unknown variables. He discussed factors such as diagnostic gaps within the systems in place for identifying an index patient. During the early days of the COVID-19 pandemic, he said, the World Health Organization (WHO) defined a threshold for how many patients should be tested in each country; after about 100 days, only three countries met this threshold, Agogo said (FIND, 2025). In low- and middle-income countries (LMICs), this threshold was never reached. He noted that faster diagnostic response is a key challenge in preventing disease spread.
After the acute phase of the COVID-19 pandemic, FIND led an evaluation to identify barriers to developing diagnostics. Primary barriers included slow access to samples and reference materials, lack of clear product requirements, and insufficient regulatory harmonization. Certain tests were
available but were not used as they could not pass the regulatory barriers in individual countries, Agogo noted. Policy gaps also hindered the use and supply of materials and diagnostics. Manufacturing issues and geopolitical dynamics introduced confusion as to where and how tests were available for purchase; some countries even changed their laws to reduce export of tests to other countries in order to increase availability to their residents. Despite the challenges, Agogo noted, diagnostic tests for COVID-19 were a great success considering they were developed from scratch and rapid diagnostics were available within the first 240 days of the COVID-19 pandemic (G7 United Kingdom, 2021). Further, there was cohesion around government, industry, and researchers to allow new technologies to be deployed quickly. This response changed the paradigm on thinking about testing, Agogo said. Before the pandemic, he said, testing was mostly considered in the context of a clinical laboratory; now, it is clear that these tests can be performed at home.
The International Pandemic Preparedness Secretariat of the G7 created the aspirational “100-day mission”—a target that accurate molecular tests and rapid diagnostic tests should be available within 100 days of the onset of a qualifying pandemic, he said (G7 United Kingdom, 2021). The Lancet Commission on Diagnostics showed that 47 percent of patients globally do not have access to diagnostics (Fleming et al., 2021). The report also showed that diagnostics were only available for a small proportion of health conditions, revealing a clear gap.
Agogo clarified that it is important to design the right test for the right location. He discussed the framework that FIND uses to assess which tests should be available and at what level of the health care system. WHO leads development of the target product profile by examining the intended use, intended user setting, and the intended type of tests. At the beginning of the COVID-19 pandemic only reference laboratories could perform diagnostic tests, but by the end of the pandemic self-testing was available. Many LMICs lack sophisticated diagnostic laboratories, which highlights the need for more accessible testing options. The use of the test is also important to consider, Agogo said. Different types of tests are needed for diagnostic or disease surveillance purposes. There is a need to consider the availability and the purpose of the tests.
Agogo suggested that molecular diagnostic availability at the point of care could fill critical gaps across different health care settings. Near point-of-care tests, he said, can be used very close to the patient within hospitals. True point-of-care tests do not require laboratory equipment and are portable and may be formulated as instrument-free test kits. Instrument-free point-of-care tests can be used at home, do not require any instruments or electrical power supply, and contain a fully automated testing process. Agogo noted that future efforts should focus on developing more
point-of-care tests while improving the performance of these tests to ensure that people can use these diagnostics close to their homes and within the local community settings, he said.
WHO recently developed a framework for pathogen prioritization based on families of known pathogens with pandemic potential (WHO, 2024a). Agogo said that this shift in strategy for pathogen prioritization will expand the scope for identifying new pathogens of pandemic potential. Further, he continued, it is important to engage the necessary partners to understand how to facilitate access and use of diagnostics for disease surveillance and testing. For example, technological innovation can be coupled with digital connectivity so that the right diagnostics are made available for people in the right place at the right time.
Finally, Agogo noted that there is a national diagnostics action plan for the United States that draws on lessons learned from COVID-19 to inform product research and development, regulatory approval, disease surveillance and community-based testing infrastructure, and financial incentives to sustain manufacturing for diagnostics. It addresses the intended user, intended use, intended setting, and the right type of tests, which makes it a comprehensive framework for guiding the development and implementation of diagnostics. He concluded that making the right technology available in the right setting will be critical for reaching patient zero.
NATURE-BASED SOLUTIONS
Jamie Reaser, Smithsonian Institution, discussed nature-based solutions as a framework for reducing disease spread. This framework is based on the concept of ecosystem services that assess the products and services that humans derive from the environment, she explained. Reaser said there is no single standard definition of nature-based solutions, but she described them as human actions that benefit natural systems and in turn benefit people. Nature-based solutions aimed at preventing zoonotic disease transmission can be framed as ecological countermeasures—highly targeted, landscape-based interventions to arrest the drivers of land-use–induced zoonotic spillover, said Reaser (Reaser et al., 2021b). Land-use–induced zoonotic spillover is the process by which infection and the shedding of pathogens from animals leads to spillover and spreads among people. Reaser, Plowright, and colleagues developed this term to complement the concepts of medical countermeasures and veterinary countermeasures, which are already accepted in practice and policy and founded in literature (Reaser et al., 2021b, 2022). The term ecological countermeasures reflects the value of ecological systems while applying a biosecurity lens, she continued.
The goal for ecological countermeasures is to foster landscape immunity through ecological protection and restoration, she said. Landscape
immunity is defined as the ecological factors that in combination maintain the immune function of wildlife species and reduce stressors within a particular ecosystem (Plowright et al., 2021). Ecological countermeasures would prevent elevated pathogen prevalence and pathogen shedding into the environment, Reaser said. Land-use changes can trigger the cascade leading to infection, shedding, spillover, and spread of disease (Reaser et al., 2021a,b).1 She said that climate change can be considered a driver of the process and an extension of the land-use changes themselves.
She continued by saying natural systems and ecological countermeasures can be compared to a game of dominoes. When landscape immunity is being well fostered, the dominoes are stable and will not fall and trigger the cascade of events leading to spillover. However, a disruption in the ecosystem, such as land-use change, can trigger the cascade of events leading to infection, shedding, spillover, and spread of pathogens, potentially resulting in an epidemic or pandemic scenario. Conceptually, ecological countermeasures can be applied to intervene in this game of dominoes, she said.
Fostering landscape immunity through the protection of various areas from a conservation perspective or restoring human-altered landscapes can stabilize these dominoes, explained Reaser. Actions such as removing invasive species that serve as hosts or facilitators to pathogens can also reduce the risk of a triggering event. Ecological countermeasures can be used to create barriers to prevent a spillover event, she said. This could include preventing bats from moving into agricultural landscapes, for example. Overall, these ecological countermeasures fall within the construct referred to as “prevention at the source.”
Reaser noted that it is important to recognize that the ecological countermeasures toolbox can be very diverse. Multiple ecological countermeasures might be feasible depending on the dynamics of the particular system. A system may be characterized by several contexts, such as natural habitats, natural–rural interface, and suburban or urban environments. Context is important to consider when designing ecological countermeasures, she added (Plowright et al., 2024).
Nature-based solutions, and ecological countermeasures in particular, for infectious disease prevention have yet to be commonly used in policy and practice, she said. However, any policy or practice that facilitates ecological protection or the restoration of ecosystems is fostering landscape immunity. Some practices in the general conservation community could be considered as ecological countermeasures, but these are not necessarily conceived from a human health perspective, she noted. Reaser concluded by providing three options to consider for future spillover prevention
___________________
1 Land-use change can refer to human-induced alteration of landscapes for a particular purpose.
efforts: (1) adopt landscape immunity and ecological countermeasures terms and concepts in science and policy; (2) engage with relevant sectors, such as those working in agricultural biocontrol, for lessons learned and cross-application; and (3) promote landscape immunity and ecological countermeasures as aspects of national biosecurity. She noted that it is important to recognize that humans are one aspect of ecological systems and do not live in isolation from other species. Therefore, people are important to incorporate into the concepts and execution of nature-based solutions and not just be seen as the drivers of change and the beneficiaries of ecosystems.
MITIGATION OF RISKS IN AGRICULTURAL SETTINGS
David Swayne, Birdflu Veterinarian LLC, discussed avian influenza as an emergent zoonosis. Swayne noted that highly pathogenic avian influenza (HPAI) is a very complex issue because it can infect many different animal species. Predictability with the virus is a challenge as the influenza A virus can undergo mutational reassortment events with other influenza viruses, he said.
Agriculture and control programs are focusing more on the risk of infections, he said. Reducing infections and the spread of disease among animals also helps control transmission into humans. For this reason, Swayne stated that high-risk animals and their resulting contaminants are a focal point of risk assessment. Globally, prevention and control of HPAI in the agricultural sector did not become a major global disease control program until the early 2000s. In 2007, the World Organisation for Animal Health (WOAH) and the Food and Agriculture Organization developed a global strategy for HPAI prevention and control, which has been revised in recent years (WOAH, 2024).
Examining the implementation of this plan has revealed successes and challenges with the initial strategy. Rapid diagnostic tests, training, and the deployment of real-time polymerase chain reaction tests proved to be effective measures for early detection of infections, said Swayne. The revised strategy is a high-level strategic direction for global and regional coordination. This version places greater emphasis on engaging communities through a participatory process that is not prescriptive or top down. The systematic approach aims to induce long-term transformative change in the poultry sectors, with a strong focus on the One Health approach to integrate public health, wildlife, and environmental sectors, he said (WOAH, 2024).
Swayne then outlined nine basic principles in global prevention and control of HPAI, which are translatable to many other zoonotic pathogens:
- Integrate risk-based monitoring and disease surveillance of wild and domestic animals.
- Improve laboratory diagnostic capacity for the early detection of HPAI and to differentiate from other pathogens.
- Establish One Health collaborations on preparedness and response capacities to control HPAI outbreaks in agriculture.
- Promote and share learned biosecurity approaches (structural and operational) along poultry value chains and at the poultry–wildlife–human interface.
- Increase the use of vaccination with emphasis on HPAI vaccine stewardship and international standards for vaccine development and production.
- Promote guidance, training, and tools for the production of infection-free value chains and safe trade.
- Promote One Health, private–public partnerships, policy and legal frameworks, and responsible investments in safe and resilient value chains.
- Share specific context knowledge on risk management.
- Support transformative research to inform development of evidence-based policy.
Swayne explained that poultry vaccination is a valuable tool that has been underused, especially in high-income countries. Vaccination in poultry can increase resistance to avian influenza infection, he said. Multiple studies have shown that it takes higher challenge doses of the virus to infect properly vaccinated birds. Vaccinated birds exposed to HPAI virus have expressed reduced influenza viral replication and shedding from the gastrointestinal and respiratory tracts, which reduces spread and environmental contamination. This helps maintain the livelihood of growers and the food security of customers, and it improves animal welfare, he said. Finally, poultry vaccination can prevent human infections, as was shown in studies in China and Vietnam, where human HPAI cases dropped rapidly after poultry vaccination was implemented.
A WOAH policy brief on HPAI vaccination noted that stricter biosecurity measures and the mass culling of poultry may no longer be sufficient to control the disease, he said (WOAH, 2023). Swayne said that vaccinations are an additional layer of protection on top of biosecurity measures, but they do not replace these measures. He noted that risk-based vaccination to the most susceptible species and in risk-prone geographic areas would be most effective and feasible.
There is no one-size-fits-all approach to HPAI prevention owing to differences in such factors as the type of poultry production, type of species,
country context, and funding, Swayne emphasized. He said that the most successful initiatives have indemnity programs that compensate owners for economic losses caused by HPAI infection. In countries without compensation, he said, there is resistance to reporting HPAI cases. Regardless of the risk, funding is necessary for developing agriculture prevention and control programs, as well as the research that is needed to support such programs. There is also disparity in funding between public health, agriculture, wildlife, and environmental sectors, particularly in LMICs. Legal frameworks of agricultural regulatory actions are also critical in determining responses and would benefit from improvement, said Swayne. When influenza A virus subtype H5N1 broke out in U.S. poultry in 2022, existing movement control policies for poultry guided mitigation efforts. When H5N1 unexpectedly spread to dairy cattle, there was no federal legal framework for cattle movement, which led to confusion and delayed response, continued Swayne. Finally, there is a need for education and communication programs for farmers, growers, and other stakeholders on why and how to contribute to prevention and control, he said.
Swayne discussed laboratory and field studies that demonstrated that HPAI virus can be spread to humans during the process of slaughtering infected poultry. Based on the data, FAO and USAID funded a program in Egypt to develop and implement a mitigation strategy at the household level. Researchers received input from Egyptian women’s focus groups in local villages to inform culturally appropriate risk mitigation processes and developed posters with the help of a medical illustrator to develop educational materials for communicating a new home-based poultry slaughter process that reached 7 million households, said Swayne (Clark et al., 2022). An important lesson from this project is that local partnership is crucial to inform behavioral change, Swayne concluded.
LABORATORY BIOSAFETY AND BIOSECURITY
Gigi Gronvall, Johns Hopkins University, discussed technical and social interventions to prevent and mitigate laboratory accidents and biosecurity risks. The first level of mitigation is to support the people working in laboratories with appropriate personal protection equipment and high-quality training; this requires established systems that provide this training and support, she said. Those systems take effort, time, and care to nurture, and it is important to ensure a safety culture in the laboratory where people can report accidents and appropriate actions are taken. There is also a need for better and faster attribution of responsibility for biological incidents, which includes scientific support to determine origins of disease (Warmbrod and and Gronvall, 2023). Gronvall added that there is a need for better communication of uncertainty, which includes the knowns and unknowns
regarding progression of an outbreak. SARS-CoV-2 variant Omicron is an example, she said. Many experts concluded that the variant’s unique sequence was an early indicator that it would lead to worse outcomes; however, the public health impact was unknown until more data were available.
Finally, Gronvall highlighted that biosafety and biosecurity issues are inherently international, which should be reflected in policy. She highlighted the Biological Threat Reduction Program of the U.S. Department of Defense as an example that helps establish biosafety and biosecurity norms on a global level (Kharaishvili et al., 2021). Gronvall concluded by referencing the National Academies report A Strategic Vision for Biological Threat Reduction: The U.S. Department of Defense and Beyond (NASEM, 2020), which supports the idea that global engagements resulting from relationships of respect and trust between and among professionals are needed now more than ever.
DISCUSSION
Funding Research for Interventions
Clements asked the panel about how to fund new interventions and support research that assesses effects on mitigation. Gurley answered that investigating spillovers is a crucial step, as there is still significant uncertainty as to how spillovers occur. Agogo and Swayne noted that WHO and the United Kingdom have developed lists of priority pathogens, which serve as a good starting point for identifying research and funding priorities. Gronvall added that there is a need to have people in leadership positions who understand the issues surrounding research and funding priorities so that they can ask the right questions to inform mitigation strategies. Reaser suggested that funding strategies need to be context specific and should consider such factors as geography and stakeholder engagement. Further, it is important to determine which priorities are already being funded and how other topics fit within the existing flow of resources, she said.
Unintended Consequences
Sleeman said that he thinks nature-based solutions have great potential, but in his experience, ecological manipulations can have unintended consequences. Reaser answered that it is important to collect data and understand the systems before taking action, which may require a lot of work, time, and resources. Environmental impact assessments can help ensure that the benefits and potential adverse effects of the intervention are weighed, she said.
An audience member asked the panel how to deter bad actors. Gronvall replied that understanding the motivations of potential bad actors is
an important area of research. There is a need to have a multipronged strategy, she said, and the National Academies put forward a framework in 2018 that described how to adjust risk assessments as technology advances (NASEM, 2018). When assessing the potential for misuse, Gronvall said, researchers can evaluate the costs, accessibility, and effects of the technologies that could be misused. She noted that there is no simple answer to this real problem.
One Health
In response to a question about the overlap between indigenous knowledge and ecological countermeasures, Reaser said that indigenous knowledge and ecological countermeasures are interrelated, as both are people-driven, systemic approaches to benefit natural systems in a way that ultimately benefits people
A member of the audience noted that there is plenty of research showing that most drivers of emerging infectious disease are related to ecological degradation, and economists have shown the benefit of primary prevention measures from a financial standpoint. Yet, there are major challenges for getting the health sector engaged to support primary prevention, such as including these measures in the pandemic agreement. Reaser replied that the conservation community needs to move more actively into a relationship with the health sector. She noted that there is an opportunity to examine how biologists, conservation practitioners, ecologists, and social scientists working in conservation can better integrate into health sciences and health policy, she said.











