Personal Protective Equipment for Influenza A(H5N1) in High-Risk Farm Settings: Proceedings of a Workshop (2026)
Chapter: 9 Optimizing Personal Protective Equipment for High-Risk Farm Settings
9
Optimizing Personal Protective Equipment for High-Risk Farm Settings
The eighth session of the workshop featured a roundtable discussion exploring multi-faceted aspects of Influenza A(H5N1) outbreaks from the perspectives of research, public health, Total Worker Health, and the broiler, layer, and dairy industries. The session highlighted the value of applying a One Health lens in addressing H5N1 and identifying research investments, infrastructure, and cross-sector collaboration in preparation for the next epidemic. Michael Payne, dairy outreach coordinator at the Western Institute for Food Safety and Security and director of the California Dairy Quality Assurance Program, moderated the session.
INDUSTRY STAKEHOLDERS
Broiler Farm H5N1 Response
Ashley Peterson, senior vice president of scientific and regulatory affairs at the National Chicken Council, outlined the ramifications of H5N1 within the broiler sector of the poultry industry. As a trade association, the National Chicken Council represents 30 U.S. broiler processing companies and approximately 25,000 family farms that raised a total of 9.4 billion chickens in 2024. With operations located nationwide from California to Delaware, much production takes place in the “broiler belt,” an area that stretches from Texas to the southeast and north toward Delaware. She described personal protective equipment (PPE) as an incredibly important tool that is used daily within food processing environments and on farms, regardless of whether an outbreak is active. Visitors to farms, such as
service technicians and veterinarians, typically wear extensive PPE, including Tyvek suits, plastic gloves, pull-on boots, hair nets, and respirators. She highlighted that outside of H5N1 outbreaks, these precautions are designed to protect commercial flocks by preventing the introduction of disease into chicken houses, including salmonella and numerous poultry diseases that pose a continual threat to avian health and food safety. Appropriate PPE is essential for professionals who travel to multiple farms in a day, she underscored. The advent of H5N1 has necessitated depopulation efforts, and this activity requires more robust PPE. She described how the ongoing outbreak that began in February 2022 has necessitated depopulation of about 14 million birds in the broiler industry, representing approximately 8 percent of the total 175 million birds depopulated due to H5N1. Underscoring the importance of PPE access, she noted that the total PPE needed for daily operations exceeded that utilized for depopulation efforts, given that the broiler industry has not been as severely affected as other sectors of the poultry industry.
Layer Farm H5N1 Response
Oscar Garrison, senior vice president for food and safety regulatory affairs at the United Egg Producer, outlined the layer farm response to H5N1. United Egg Producer represents about 90 percent of U.S. egg production by volume, which includes approximately 300 million laying hens nationwide. Noting the Animal and Plant Health Inspection Service biosecurity principles, he emphasized that PPE is an important component of standard daily operations. Protecting both workers and birds, PPE prevents the introduction of pathogens ranging from food pathogens like salmonella to foreign animal diseases to a variety of poultry diseases. In addition to PPE, monitoring flock health is of utmost importance to poultry farmers, said Garrison. In the layer industry, monitoring includes water consumption, feed consumption, mortality, as well as monitoring the surrounding area, as an increase in disease on nearby farms triggers changes to PPE protocol. In the event of a suspected disease outbreak, farms promptly take samples for testing and prioritize worker protection via PPE. Many farms have workers shower onsite before and after their shifts to add a higher level of protection. Standard operating procedures may require a dust mask, optional goggles or safety glasses, and a change of clothing. Once disease is suspected, farms may require workers to wear N95® respirators. Underscoring that weather conditions affect PPE use, he commented on the balance between protection and comfort in extreme temperatures and the ability to perform tasks. Science informs determinations regarding an appropriate balance, he added. Garrison explained that the introduction of a foreign animal disease to a poultry farm initiates rapid depopulation of
all animals at the facility. The ability to quickly depopulate the index house (i.e., the first house in which symptoms occur) limits the spread to birds in other areas of the farm. This benefits worker protection, given that fewer of the animals being depopulated are infected with the virus. Garrison stated that thorough depopulation efforts performed in a timely manner protect human health and prevent spread to nearby farms or other vectors.
Dairy Farm H5N1 Response
Anja Raudabaugh, chief executive officer of Western United Dairies (WUD), underscored the intensity of the 6-month H5N1 response and the hardship for dairy farmers of losing their cows, noting that 770 of the 786 dairies represented by WUD contracted H5N1. With approximately 1,000 dairies in California, this constitutes an infection rate above 75 percent. Some pockets of herds located north of Sacramento and toward the Pacific Coast remain unaffected, and daily milk samples continue to test negative for H5N1. Approximately 48 California farms are currently under quarantine, with reinfections occurring in Central Valley and new infections in San Jacinto and Ontario. Although H5N1 continues to affect California milk production, production is increasing. Raudabaugh noted the dairy industry’s efficacy in increasing milk production following such declines.
Describing tri-agency coordination between WUD, the California Department of Public Health (CDPH), and the California Division of Occupational Safety and Health as the California dairy industry’s “secret weapon” in responding to H5N1, Raudabaugh recalled that the agencies communicated several times a week at the height of the severity of the emergency. This partnership enabled distribution and tracking of 4.6 million units of PPE, which was available in such large quantities due to CDPH stockpiling after the shortages of the COVID-19 pandemic. The collaboration established a small warehouse in the Central Valley to facilitate rapid distribution to southern California. Data were collected on the quantity of PPE delivered to each farm, the number of workers that received PPE, the number of farmworkers that used the PPE they received, and the length of time the PPE was used, which was measured by the amount of time between resupply requests. In October 2024, many dairies put forth makeshift biosecurity efforts, such as creating barricades around their properties with hay bales to discourage unauthorized visitors, such as delivery people, from entering their farms. As the winter proceeded, farm owners realized that the outbreak required higher levels of biosecurity, said Raudabaugh.
Raudabaugh stated that making testing tools available at local health and occupational health departments as a part of worker support during an animal health emergency is critical. She recalled that at the height of infection in October 2024, local health departments, emergency departments,
and occupational health departments did not have testing capability for the active strain. Thus, farmworkers sent to these locations were unable to receive H5N1 testing. During educational efforts to raise H5N1 awareness, the questions farmworkers asked indicated that protecting their families and communities was top of mind. For example, they asked about how to prevent H5N1 from affecting people outside of the farm. Raudabaugh underscored the challenge of providing community protection during times when Tamiflu, other antiviral medications, and testing were unavailable. She recalled that some farmworkers were reluctant to be tested out of fear of retaliation at their workplace. Despite overcoming this reluctance, some farmworkers were turned away without being tested due to lack of testing supplies. Human H5N1 often presents as conjunctivitis, and eye symptoms are not uncommon in dairy farm settings where workers can get dust or hay in their eyes. Raudabaugh communicated to farmers the importance of getting any eye symptoms diagnosed by a health professional, and the unavailability of testing for all farmworkers who followed this guidance constituted a gap in response capability.
Extensive coordination between WUD and CDPH enabled in-person educational sessions presented in English, Spanish, and various dialects, such as Mixtec, said Raudabaugh. They also created training videos to expand the reach of educational information about H5N1. Much of the training for herdsmen focused on identifying H5N1 in cows and in milk. Given that infected cows can present as healthy, the trainings emphasized the difficulty in detecting H5N1 from visual cues and the associated importance of wearing PPE consistently. Currently, viral infections continue, as does collaboration between WUD and CDPH to address the evolving H5N1 situation. Uncertainty remains about the cycle threshold (CT) score that necessitates quarantine. Noting that quarantine can last 6–9 months, she remarked that farmworkers can become frustrated with daily PPE safety meetings. A long-term solution will entail a dairy cow vaccine to reduce viral load, she contended, noting the possibility that H5N1 will be endemic. Raudabaugh stated that protecting nearby poultry farms and naïve cows coming into herds ultimately requires vaccine development.
RESEARCH PERSPECTIVE
Edie Marshall, branch chief of Antimicrobial Use and Stewardship at the California Department of Food and Agriculture, acknowledged that some California dairy producers were unable to prevent the introduction of H5N1 to their farms despite executing numerous biosecurity measures, highlighting the role of risk prioritization. Currently, redetections on chronically infected dairy farms are occurring, yet no human cases have been identified in California since January 2025. Positing that the risk has
shifted, she reported that fewer herds are currently infected than during the height of the outbreak, and CT counts are now higher, indicating lower viral load. In this context, Marshall submitted that instructing farmworkers to use the same level of PPE that they used in October 2024 could result in compliance fatigue and wasted time and PPE.
Marshall suggested using a research-informed approach in directing available resources to addressing greatest H5N1 risks to humans. For instance, data indicate that aerosols are one of the mechanisms driving infection, and risk of aerosol transmissions varies in different areas of a farm (Campbell et al., 2025b). Additionally, CT scores indicating low viral load are common on farms with redetection of H5N1, and thus reinfected herds may not pose the same risk as naïve herds with high viral load, she maintained. Marshall cautioned that issuing the same PPE recommendations for all levels of detected viral load can erode credibility and trust with producers. Researchers described H5N1 transmission as multifactorial and discussed ongoing efforts to better characterize transmission mechanisms, associated risk levels, and corresponding PPE considerations. Marshall also discussed research related to the development and evaluation of new and alternative technologies, alongside data used to tailor PPE approaches to specific contexts.
PUBLIC HEALTH PERSPECTIVE
Jennifer Nuzzo, professor and director of the Pandemic Center at the Brown University School of Public Health, outlined three general dimensions of any public health intervention: (1) epidemiological; (2) logistical feasibility; and (3) sociopolitical or adherence. Public health emergencies can change, particularly when addressing a virus. She maintained that recommendations or assurances based on the past or on the current moment are inadequate, and response efforts should allow for the possibility of change. She stated that much remains uncertain about this virus and its potential. Hopes that H5N1 would disappear within a few months of initial detection on farms have not materialized; the virus continues to circulate and remains somewhat unpredictable in its timing. Additionally, susceptible animals continue to be born and/or are transported between farms. Nuzzo stated that H5N1 is likely to remain a viral threat for the foreseeable future.
Thus far, relatively few H5N1 infections have been in humans, said Nuzzo. Although U.S. human infections have generally been mild, she cautioned against inferring that H5N1 is a mild disease from a very limited number of observations. Worldwide, approximately 40 percent of human cases of H5N1 reported since January 2025 have been fatal. She emphasized that the difference in severity between U.S. and worldwide cases has not been explained, and therefore H5N1 should be considered a deadly
disease. While some U.S. mild human infections are inevitably escaping detection, serologic studies in high-risk populations do not indicate a large number of undetected infections. However, if the true number of human cases is not much higher than what has been detected, this suggests that the case count is still too low to ease concerns about H5N1’s deadliness in humans in the United States, Nuzzo maintained.
Evidence currently does not indicate that H5N1 is spreading between humans in a sustained fashion, but Nuzzo emphasized that viral transmission can change over time and the capability to detect if or when such a change occurs is lacking. She stated that PPE decisions should factor in the degree of error that can be tolerated, given that determinations are based on current data about a virus that has the potential to become more severe. Additionally, much of what is known about H5N1 is based on voluntary testing among symptomatic individuals. While this may be adequate for now, she argued that it could eventually fall short, particularly in the absence of a rapid response mechanism to detect and investigate emerging changes. Nuzzo highlighted that researchers have a general idea of potential transmission factors, such as migratory birds, but the virus’s movement is not fully understood. For instance, infections have been detected on farms with good adherence to biosecurity measures. She noted a study that indicated that wind could play a role. If researchers determine that wind is a mechanism of transmission, said Nuzzo, the context for PPE recommendations is substantially different than that of a biosecurity-controlled disease in which exposure occurs within facility walls.
The approach to mitigating human H5N1 infection thus far has involved protecting farmworkers with PPE, detecting infections on farms, and administering post-exposure prophylaxis, Nuzzo outlined. She maintained that this strategy may be sufficient for the virus in its current form, but this approach would be inadequate should the virus become more easily transmissible or result in deadlier infection. Describing the window of opportunity to intervene as incredibly narrow, she emphasized the lack of systems capable of reacting quickly to potential changes. Nuzzo said that in determining the circumstances that require various levels of PPE, potential viral changes should be considered. Moreover, additional epidemiological research was discussed in relation to the development of more robust PPE strategies. Numerous questions remain, such as how H5N1 spreads, the minimum PPE required to protect farm workers, whether specific types of PPE are necessary, and the circumstances and locations that necessitate PPE use. She described how, in some conditions, wearing PPE may actually increase the risk of health issues, such as in extremely hot temperatures. Nuzzo added that PPE is an important tool, but it may not be sufficient for all circumstances.
In considering logistical aspects of H5N1 response, Nuzzo remarked that this virus warrants a long-term strategy rather than an episodic response, which raises the issue of funding. For example, long-term strategies involve determinations about the parties responsible for providing and paying for PPE and the duration of time this responsibility holds. Thus far, responses to H5N1 events have been developed within the context of a limited set of circumstances. The mobility of many farmworkers between farms may require a harmonized approach that considers varied policies across different farms, implementation challenges, and worker protection issues, said Nuzzo. Fortunately, resources are available, she noted. Organizations are actively working to educate farmworkers about H5N1 risk and the benefits and proper use of PPE, and they are using data-driven approaches to formulate effective communications strategies. She pointed out that viral changes and corresponding shifts in assessing risk and developing recommendations could pose communications challenges, and planning for dynamic communication (i.e., messaging that evolves in relation to context) could be helpful. Nuzzo stated that priming the audience to expect such changes could facilitate future communications.
Recent public health emergencies have provided many learning opportunities about the social and political aspects of public health response, Nuzzo remarked. For instance, the limitations of mandates and penalties reveal the continued relevance of harm reduction approaches. Providing resources to people fosters their ability to make choices that increase safety. Environment affects adherence to PPE, and public health advocates should consider the level of discomfort that people are willing to tolerate as well as the circumstances that influence tolerance, she maintained. Simultaneously, efforts to improve the comfort of PPE continue. Emphasizing that human behavior can trump policies, Nuzzo cautioned against strategies that farmworkers may perceive as penalties; in past outbreaks of other diseases, such strategies had the counterproductive effect of driving farmworkers to conceal their infections.
ONE HEALTH PERSPECTIVE
Meghan F. Davis, associate professor and director of the Johns Hopkins P.O.E. Total Worker Health® Center in Mental Health at Johns Hopkins University, explained that the Total Worker Health (TWH) field takes a holistic approach to worker protection. Built on core occupational safety and health principles, TWH adds health promotion and illness management components to address individual health and psychosocial factors. Moreover, TWH considers enterprise outcomes, such as worker productivity, presenteeism or absenteeism, and turnover. Davis highlighted that TWH has a hierarchy of controls similar to that of the National Institute
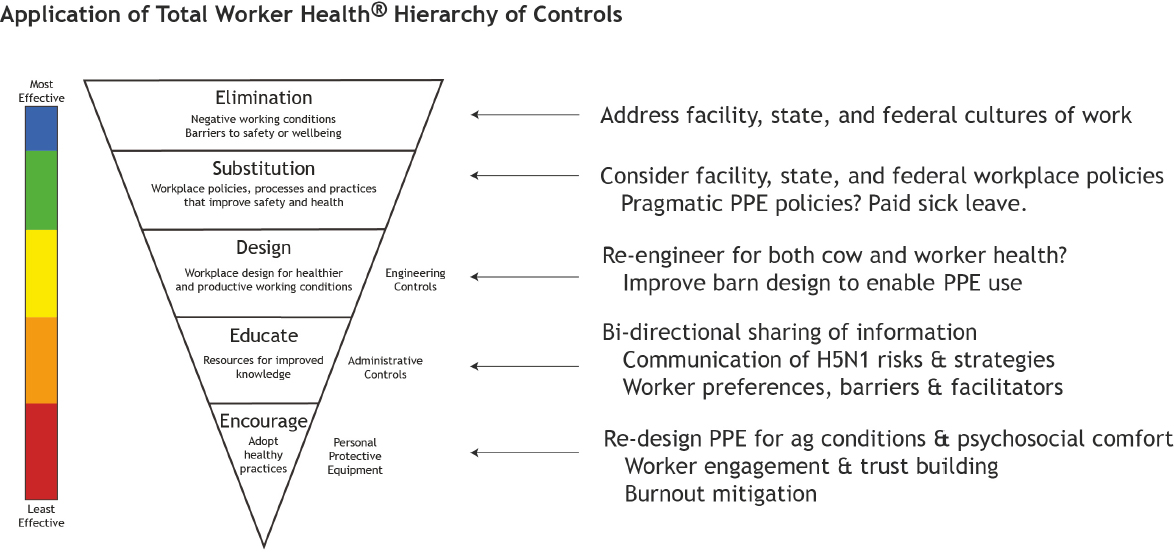
for Occupational Safety and Health (NIOSH) (Anger et al., 2019; NIOSH, 2024). In mapping the two hierarchy frameworks, she outlined considerations for addressing the hierarchy of controls from a TWH perspective as they pertain to PPE in farm settings (see Figure 9-1).
Davis outlined that the TWH hierarchy of controls includes, from most to least effective: elimination, substitution, design, education, and encouragement. Applying this framework to PPE for H5N1, elimination might address factors related to facility, state, and federal cultures of work that deter PPE use. She noted the importance of leadership and modeling in creating a safe work culture. Substitution could involve replacing facility, state, and federal policies with more pragmatic PPE recommendations, and ensuring facilities provide paid sick leave and encourage workers to stay home when sick. Design could entail innovation and re-engineering that supports livestock and worker health. For instance, improving barn design could facilitate PPE use, and providing onsite facilities enables employees to shower before and after shifts and launder their clothing. She remarked that innovations could pertain to engineering controls in the NIOSH hierarchy of controls. For example, the implementation of air jets in milking parlor design or use of negative pressure could affect the experience of wearing PPE or the ease of work, so these should be taken into consideration as part of any re-design process. Additionally, PPE design could interfere with work tasks and generate stress for farmworkers. Davis reported that health care workers have indicated that donning and doffing PPE during the COVID-19 pandemic and H5N1 outbreak interfered with their ability to complete their work, which could have serious ramifications for the health and safety of patients in their care. Education involves bi-directional sharing of information—top down communication of H5N1 risks and strategies to workers, and bottom-up sharing by workers related to their preferences, barriers, and facilitators. Encouragement could involve redesigning PPE to support farmworker psychosocial comfort and engagement, build trust, and mitigate burnout, said Davis.
Both One Health and TWH are holistic approaches that emphasize the importance of systems thinking. The One Health approach considers interconnected human, animal, and environmental factors, and Davis noted that it can be applied in planning PPE logistics and operations. For instance, PPE is primarily for human protection, but it can affect animal health as well. Many farmworkers do not doff their PPE until they return home, creating opportunities to introduce pathogens into the community. Thus, although PPE is designed to enhance safety, it could serve as a fomite in pathogen transmission. Reports of fatal cases of H5N1 in indoor house cats owned by Michigan dairy workers demonstrates this potential (Naraharisetti et al., 2025). In one such case, a cat had direct contact with a worker’s coveralls, contracted H5N1, and died, whereas another cat in the home did not have
NOTE: PPE = personal protective equipment.
SOURCE: Davis presentation, September 30, 2025. Adapted by M. F. Davis from Anger et al., Effectiveness of Total Worker Health Interventions; in Hudson et al., Total Worker Health, American Psychological Association, 2019.
contact with the coveralls and remained negative. Davis suggested that PPE design and engineering should consider the full value chain, from supply to disposal, to improve the availability and environmental ramifications of equipment.
ROUNDTABLE DISCUSSION
H5N1 Research and Response Priorities
Payne asked about the most pressing initiatives for advising stakeholders about PPE and improving preparedness for H5N1 outbreaks. Peterson emphasized the importance of donning and doffing PPE on the farm and never taking disposable PPE home. During a steady-state scenario, the broiler sector ensures that each farm has its own disposable PPE that does not leave the farm. During an outbreak, all PPE is collected after use and appropriately disposed of, Peterson added. Garrison noted a lack of systematic safety evaluation and epidemiology of airborne transmission. In the absence of fully understanding how H5N1 spreads, determining the most effective ways to protect public health during outbreaks remains challenging. Garrison said that PPE is a routine aspect of biosecurity. Rather than aim for a constant, high level of protection across all scenarios, he contended that the scope and scale of PPE use should be adjusted based on variables such as viral load and operational context of work setting and task. He remarked that improper PPE disposal reflects gaps in planning and systematic communication among individuals involved. Gaps in communication and in scientific data impede effective H5N1 responses, Garrison remarked.
Raudabaugh underscored discussion of a dairy cow H5N1 vaccine, describing it as a rapid and relatively low-cost approach to addressing the virus. She noted that older cows appear more resilient to H5N1, typically surviving infection and returning to pre-infection milk production levels, whereas young cows are more prone to fatality. This suggests that having more immunities may offer benefits in fighting off this new virus. Echoing the importance of donning and doffing PPE onsite, Raudabaugh emphasized the value of adopting PPE protocols, creating donning and doffing stations, and instructing workers to keep all PPE onsite, and she suggests these steps in her communications with dairies. She added that numerous professionals visit farms, such as hoof trimmers and insemination experts, and they may inadvertently traffic fomites between multiple dairies. At the height of the H5N1 outbreak, farms limited visitors to try to reduce transmission risk. Remarking on the One Health approach, she stressed the role that local health departments can play in educational efforts. Raudabaugh suggested that local public health professionals routinely visit dairy farms
to address a range of health issues—such as sexually transmitted infections, reproductive health, and flu vaccine clinics—as a way of reducing educational barriers before an outbreak occurs.
Marshall stated that a local public health professional equipped to make recommendations specifically tailored to each farm would benefit H5N1 response efforts. For example, this person could measure milking parlor airflow and, if the airflow is sufficiently high to dilute the virus, communicate that data indicate that face shields offer adequate protection in this environment. Marshall highlighted areas for additional research related to understanding the risk of H5N1 transmission via aerosolized milk droplets and remarked on the potential value of linking viral load metrics to PPE recommendations. For example, the higher viral load in newly infected cows could necessitate additional PPE, whereas low viral load in milk could indicate that a lower level of PPE is adequate. In this scenario, safety advocates could communicate that the cows are highly infectious for a specific amount of time—thereby necessitating goggles in the short term—but once the viral load decreases, workers can return to wearing safety glasses. Similarly, increased understanding of viral load and risk could inform recommendations in the poultry industry. Marshall maintained that PPE compliance would likely increase if farmworkers were instructed to wear higher levels of PPE for days or weeks rather than for months, and more data could potentially enable such recommendations.
Davis echoed discussion that additional evidence can inform pragmatic policies differentiating between factors within a farm and across an industry. An implementation science approach that engages the participation of farmworkers could improve the feasibility and logistics of safety measures. Trained in Tulare, California, she recounted the vast differences in systems and cultural contexts she experienced when practicing in Pennsylvania Amish and Mennonite dairy farms. Although approaches should be individualized to each farm, approaches created and tested for large-scale freestall facilities may require substantial adjustment for use on smaller dairies with a different barn design. Davis said that understanding how context affects virus transmission and the building of that knowledge into the community interface could fill current gaps. Payne commented on the benefit of research exploring the wearability of PPE. He suggested paying dairy workers to wear various configurations of PPE for one shift, such as an N95®, an elastomeric respirator, an N95® with goggles, and an N95® with a face shield. After the shift, researchers could collect qualitative data from the farmworkers to learn which types of PPE are more readily accepted in farm settings.
Nuzzo emphasized research gaps regarding H5N1 and PPE, including questions of epidemiology, risk level, and PPE acceptability. For instance, it is currently unknown whether H5N1 is spreading from infected persons to
their close contacts and whether infected people can be asymptomatic. She underscored the importance of a rapid research network for determining pertinent questions in real time and identifying answers. Highlighting the influence of perceived risk on willingness to accept PPE, she pointed out that perceived risk can change in response to additional information and the perceived trustworthiness of the information. Nuzzo stated that trust can change as an emergency develops, and trust can influence how quickly a system is able to adapt.
Specificity in H5N1 Livestock Response
Noting differences in broiler, layer, and dairy industries, Payne asked about specific needs within each of these sectors. He pointed out that unlike the dairy industry, poultry utilizes depopulation, which entails specific PPE requirements. Raudabaugh highlighted that each dairy is unique in its setup and operations, and therefore tailored approaches are more effective than universal ones. She stated her interest in the concept of retrofitting barns, noting that numerous differences between dairies include type of milking stall, configuration of milking parlor, style of freestall barn, and whether a farm is organic or pasture-based. Raudabaugh pointed out that a few days of intensive outbreak response interventions completely disrupts a dairy’s production and income. During the height of H5N1 dairy farm outbreaks, herd isolation appeared to slow herd-to-herd transmission. Anecdotal data indicates that isolating springers—i.e., cows on the verge of giving birth—and calves for three or more weeks slows H5N1 spread, and Raudabaugh anticipates research findings on this practice.
Preparing for an Evolving Viral Threat
Payne described how H5N1 has spread to wildlife, birds, cows, cats, and humans, but he noted that human infections have thus far been mild. He asked how to best prepare for a zoonotic disease that affects livestock. Davis replied that H5N1 adaptation to human-to-human transmission or greater prevalence in the domestic cat population would necessitate numerous groups not yet involved in the response, such as companion animal veterinarians and animal shelter and control workers. An enormous animal health workforce is not yet included in H5N1 response planning, yet the animal populations they serve could suddenly become affected, she cautioned. Davis suggested that engaging these groups now to establish communication channels and understand the emergent PPE use in their settings would benefit preparedness efforts. Nuzzo stated her concern about the characterization of H5N1 as mild, given that it causes human fatality in other parts of the world and genomic analysis has not explained why.
She described PPE as an important tool, but should the virus become more transmissible to humans, then PPE would not be as beneficial as vaccination. Thus, Nuzzo contended that preparedness efforts should determine the mechanism for developing a vaccine and plan for the administration and tracking of vaccines within the farmworker population.
Raudabaugh described vaccine strategy as the ultimate goal in an H5N1 response. Noting CDPH’s recent success in flu vaccination outreach to farmworkers, she stated that vaccine hesitancy has been substantial in the farmworker community, particularly after the COVID-19 pandemic. Messaging that emphasizes the protective benefits that vaccination extends to family and community members has been effective in shifting farmworker vaccine hesitancy. Similarly, she stated, tying Tamiflu treatment with protecting one’s family has been well received. In addition to applying a family health perspective, CDPH has offered gift cards and other incentives for vaccination. Underscoring the importance of understanding a target audience’s perspective, she remarked that many farmworkers have traumatic vaccination stories. Local public health efforts to build trust with farmworker communities can cultivate the view of local public health as a supportive resource, said Raudabaugh, adding that this dynamic helps to establish synergy between community protection and managing potential zoonotic outbreaks.
Peterson commented that vaccine education and access are extremely important. She described how some people are hesitant to get vaccines and are particularly concerned about mRNA vaccines. Additionally, she emphasized that discussions about H5N1 cases and mortality rates should consider how animals are raised. Peterson stated that the H5N1 mortality rate is higher in Cambodia, where some people allow livestock into their homes, and she contrasted this with the U.S. commercial industry, where birds are housed separately from humans and other animals. Payne noted a dairy worker survey in which a majority of participants indicated their willingness to take a vaccine should one become available and was provided free of charge. He remarked that vaccination could minimize many of the problems associated with H5N1.
Personal Protective Equipment Considerations for Farm Settings
Pointing to a robust body of literature indicating that animals, including cows, recognize faces and bodies, Payne remarked that PPE can affect cows’ facial and body recognition abilities and, in turn, affect their behavior. Raudabaugh underscored that innovation of safety technology should consider the context of working with large animals. Farmworkers are selected for their ability to care for animals, and cows, in turn, care for them, she stated. Any PPE that startles cows and causes them to turn and
run would be problematic on a dairy farm. Cows are able to adapt over time, but many farmworkers would appropriately be hesitant to use PPE that impairs cows’ ability to recognize their faces, said Raudabaugh. Payne asked about other considerations in recommending or distributing PPE to farmworkers. Peterson replied that PPE provision efforts should consider potential latex allergies. Recalling his frustration at being provided with gloves that were too small and routinely tore when he put them on, Payne highlighted the importance of proper fit. Marshall recounted occasions where PPE distributed from stockpiles appeared to be non-preferred items that had previously been passed over, such as goggles that impair peripheral vision. She emphasized that a dairy farm is a dangerous work environment containing large animals, and farmworkers have to be alert to the possibility of being struck by a kicking cow or a swinging gate. Thus, visibility is important in remaining safe in a dairy, and PPE determinations should consider the safety risk that decreased visibility poses to farmworkers, said Marshall.
Confidence and Risk Perception
In response to a question about how to increase confidence in PPE, Nuzzo remarked that confidence is partially related to risk perception and to understanding the intent of PPE. For example, workers may not know whether the PPE is intended to protect them or the operations of the facility. Moreover, PPE recommendations that do not align with a farmworker’s perception of the risk are not likely to drive confidence—a dynamic that also occurs in the general population regarding PPE. Approaches for increasing confidence in PPE include working to ensure alignment between PPE recommendations and people’s understanding of risk, making data-based recommendations, and communicating why a PPE strategy is being promoted and who it is intended to benefit, said Nuzzo.
Role of Milk Sampling in PPE Recommendations
A participant asked whether preclinical diagnosis via milk sampling would aid in timely PPE use. Marshall replied that the California dairy industry includes two million cows, and therefore testing all cows or every bulk milk tank is not feasible. Marshall remarked that an ideal method of milk sampling would entail an inline sampler with the capacity to detect disease, but such technology does not currently exist. Moreover, adoption of such technology would require that it be affordable, scalable, and reliable. Emphasizing the helpfulness of early detection, she explained that much remains unknown about H5N1 transmission. A study conducted substantial and varied sampling efforts across a dairy, yet sampling did not
reveal a pattern suggestive of how the infection reached the farm (Campbell et al., 2025b). Marshall remarked on the challenges associated with conducting such research at a larger scale, particularly because it would need to be carried out in naïve herds, given the immunity that has developed in affected farms. Marshall stated that current methodologies and resources do not support testing at scale. Davis stated that PPE is the last barrier between humans and pathogens, and PPE protocols that continually shift in response to milk samples are likely to cause confusion and interfere with ease of work. However, the development of surveillance strategies that allow for feedback loops within the PPE policy could allow a pragmatic approach. For instance, if specific CT values from bulk tank samples were connected to specific levels of PPE, this could enable more precise recommendations. This framework would require farmworkers to wear high levels of PPE for shorter durations, which could help to mitigate the burnout that often develops in response to PPE and other safety strategies, said Davis.
Take-Home Messages
Payne asked the panelists to offer take-home messages. Nuzzo emphasized the importance of a network capable of rapidly assessing conditions and informing adaptations as a virus evolves, and she discussed advocacy for a government-led effort to establish such a network. Marshall highlighted the importance of collaboration in identifying ways to make daily PPE use more effective and feasible. Peterson noted that the broiler industry has learned much in contending with H5N1, and cross-sector communication could inform responses in sectors not yet as heavily affected. Garrison highlighted the role of real-time epidemiology in identifying how H5N1 is spreading between animals and between farms. The ability to mitigate vectors would decrease emergencies and associated reliance on PPE. Garrison underscored the challenge of making drastic decisions to mitigate transmission in the absence of scientific research that informs which steps are most effective. Raudabaugh remarked on the importance of clearly defined thresholds that indicate when quarantine and PPE are applied. Noting that PPE is a helpful tool, Raudabaugh stated that an effective H5N1 response calls for the more powerful tool of vaccine development.
This page intentionally left blank.















