Personal Protective Equipment for Influenza A(H5N1) in High-Risk Farm Settings: Proceedings of a Workshop (2026)
Chapter: 4 Individual Barriers to Personal Protective Equipment Use for H5N1 Infection Control and Prevention in High-Risk Farm Settings
4
Individual Barriers to Personal Protective Equipment Use for H5N1 Infection Control and Prevention in High-Risk Farm Settings
The third session of the workshop featured lived experiences of the challenges of implementing personal protective equipment (PPE) use on farms, explored connections between PPE use and risk perception, and discussed approaches to barriers of effective PPE use. Beth Lipton, Washington State Department of Health, moderated the session. She underscored that despite PPE being the last line of defense between farmworkers and biological hazards, such as Influenza A(H5N1), PPE use in accordance with recommendations has been inconsistent on farms. Green highlighted the value of understanding the challenges and barriers to PPE use and simultaneously supporting farmworkers’ health, dignity, and livelihoods.
INSIGHTS FROM FARMWORKERS AND PRODUCERS
Brent Wilson, owner of Wilson Centennial Farm and member of the Michigan Milk Producers Association (MMPA), offered his experience of an H5N1 outbreak and response as a Michigan dairy farm owner. When H5N1 was detected on his farm in May 2024, the pathogen was traced to another dairy 15 miles away that had recently brought in new cows from the Texas Panhandle. Six miles away, a turkey farm with 10,000 birds tested positive in April 2024. Subsequently, the largest poultry producer in the state, employing over 400 people, detected an outbreak. During a weekly herd health check, the veterinarian asked why farmworkers were feeding two cows via a stomach tube. Wilson told her that the cows had high fevers and were not eating. When the veterinarian replied that she thought they had “bird flu,” (i.e., H5N1) he told her that he was aware but
did not want to report it. Urging him to report, the veterinarian explained that in her clinic of seven colleagues serving approximately 35,000 cows in a 40-mile radius, they estimated that two-thirds of the dairy farms were infected. Reminding Wilson that he collaborates with Michigan State University (MSU) on research projects on bovine leukemia, Johne’s disease, and udder edema, the veterinarian convinced him to allow her to take samples from the animals. The cows did indeed test positive for H5N1.
Wilson then informed his milk buyer, MMPA, about the infection, and they in turn alerted MSU. MSU sent numerous researchers and veterinary students to sample 15 cows across 10 groups of cattle at the farm. Quarantine rules went into effect, prohibiting the sale of beef across state lines and only allowing carcasses to be sold to processors within Michigan. Outlining that high fever, abortion, and somatic cell count mastitis are H5N1 symptoms in cows, Wilson noted that somatic cell count elevated sharply with the outbreak. In years prior, his farm won numerous awards from the National Mastitis Council due to low somatic cell counts. Using the California mastitis test, he routinely samples for somatic cell count for all cows whose milk is deposited in the bulk tank. During the outbreak, he suspected new strains of mastitis, but samples sent to MSU indicated Streptococcus uberis, a common cause of mastitis in dairy cattle. However, Wilson remarked that the 50 percent recovery rate he typically sees with mastitis on his farm did not occur during the outbreak.
In response to H5N1 detection, farmworkers were required to wear gloves while milking cows, said Wilson. He estimated that half of the Spanish-speaking employees at the farm had heard that H5N1 could be contracted from working with cows, with the eyes being particularly vulnerable. Farmworkers were wearing goggles only due to concern about manure, urine, or milk potentially getting in their eyes. Later, Wilson discovered that the virus can be passed through milk, but it is not found in meat nor in manure. His employees now wear gloves and respirators despite the high humidity in the milking parlors. The Centers for Disease Control and Prevention (CDC) sent a team—half of whom were Spanish-speaking—to the large, nearby poultry farm, and they requested that Wilson send as many of his Spanish-speaking employees for testing as possible. Two shifts of workers were given blood tests over the course of 2 days, and Wilson and his workers were relieved to receive negative tests results, given their exposure to sick animals. In addition to testing, the CDC team gave an informational presentation on the need for face shields, gloves, and respirators, and on the proper use of this PPE.
The outbreak persisted several months after the initial May 2024 detection. Wilson explained that Michigan regulations specify that quarantine remains in place until a farm demonstrates three consecutive negative milk samples. His farm achieved this status in February 2025, enabling the sale
of cows through livestock arenas to resume. Emphasizing how much he values his employees and does not want them to get sick, Wilson stated that PPE use on the farm has increased since the outbreak. Contending with the challenges of H5N1 offered a learning opportunity, said Wilson, and he has shared his experience via talks given to Canadian dairy farmers and at the World Dairy Expo.
RESEARCH-BASED PERSPECTIVES FROM THE FIELD AND PRACTICAL EXPERIENCES FROM RESEARCHERS
H5N1 Occupational Survey Findings
Anabel Rodriguez, assistant professor at Texas A&M University, reviewed preliminary findings from an occupational survey conducted with dairy farmworkers to better understand factors related to H5N1. For the past decade, she has worked in Texas and New Mexico to improve the health, safety, and well-being of dairy employees. Rodriguez underscored that barriers to PPE use at the individual level have important implications for infection control and prevention strategies in high-risk agricultural settings. Moreover, dairy employees are essential workers who play a critical role in food security, economic stability, and, consequently, national security, she emphasized. Thus, protecting farmworkers is both a matter of public health and of strategic importance. A recent study tested 625 dairy farmworkers across Texas, New Mexico, and California for H5N1 seropositivity and administered an occupational survey. Collecting data on occupational characteristics, the survey addressed work schedule, work history, and specific tasks performed, particularly those involving exposure to milk or direct contact with sick cattle. Farmworkers were also questioned about any symptoms experienced at the time of the outbreak and on the day of the survey, exposure to other animals on or off the farm, use of and access to PPE, and any PPE training received. Notably, the survey explored dairy farmworker awareness of bird flu, their perceived knowledge of prevention and transmission, familiarity with health information sources, and vaccination history and willingness to receive a vaccine, Rodriguez outlined.
The occupational data reflected similar demographics to other data Rodriguez and colleagues have collected over the past 10 years. The participating dairy farmworkers were 96 percent Hispanic and 79 percent male, ranging from 18 to 77 years of age. The primary language spoken was Spanish for 76 percent of respondents and Guatemalan K’iche’ for 9 percent.1 Approximately 68 percent lived in a house or trailer, and 23 percent
___________________
1 K’iche’is an Indigenous Mayan language spoken in the highlands of Guatemala and Mexico.
lived in employer-provided housing. The average household size was just under four individuals and ranged from 1–11 persons. Rodriguez emphasized that 39 percent of participants lived with other dairy farmworkers. Data on underlying chronic conditions reflect a “healthy worker bias” in which smaller percentages of the farmworkers had diseases in comparison to the general population, she explained. The survey found that 7 percent had diabetes, 13 percent had hypertension, and 8 percent had hypercholesterolemia, Rodriguez outlined.
Regarding operational characteristics, about 20 percent of the farmworkers surveyed were milkers, 15 percent performed multiple job duties, 7 percent were feeders, and 6 percent were tractor drivers, Rodriguez detailed. On average, the participants had 4 years of experience working on dairy farms and worked 6 10-hour days per week. Approximately 40 percent responded that they worked with sick cattle after H5N1 was detected on the farm, and 31 percent responded that they handled or cared for sick cows or calves. The survey asked farmworkers about symptoms they experienced during the outbreak. Acknowledging the potential for “recall bias” in which participants do not accurately remember past events, Rodriguez highlighted that 36 percent reported having at least one symptom while the cattle were sick.
Gauging PPE use and access, the survey asked about habits both before and after the H5N1 outbreak. Rodriguez emphasized that only minimal increases in PPE use occurred after detection. Approximately 26 percent of respondents used some form of PPE during the outbreak. The types of PPE used most often were gloves, rubber boots, pants, and sleeves. Almost 94 percent indicated that they purchased some or all of their PPE independently, and 51 percent replied that employers provided them with some PPE. Rodriguez explained that farms sometimes provide an initial set of PPE and workers are then responsible for replacing it. The survey explored whether farmworkers changed clothing after work, and 65 percent reported going home in their work clothes. Regarding H5N1 awareness and knowledge, 67 percent of participants indicated they had heard of bird flu, but only 38 percent responded that they knew what bird flu was. Although approximately 60 percent of farmworkers reported concern about becoming infected, only 30 percent indicated that they understood how H5N1 is transmitted, and only 34 percent knew how to protect themselves from the virus. When asked about recognizing symptoms of H5N1 in humans and cows, 26 and 23 percent, respectively, responded that they were familiar with the symptoms. About 35 percent of participants reported receiving any type of H5N1 training on the farm. Almost 60 percent of farmworkers surveyed indicated interest in receiving an H5N1 vaccine if one were provided to them free of charge on the farm. Rodriguez highlighted that the respondents that reported concern about becoming infected with H5N1
were more likely to have a history of vaccine uptake than those who indicated they were not concerned about contracting the virus.
H5N1 Community Assessments
Bethany Boggess Alcauter, director of research and public health programs at the National Center for Farmworker Health (NCFH), reviewed preliminary findings from H5N1 community assessments with dairy farmworkers that explored H5N1 knowledge and practices, PPE access and use, barriers to testing, health care access, vaccination rates, and demographics. Working with an established network of community-based organizations, NCFH conducts outreach and education about emerging infectious diseases to farmworkers across the United States. In 2024, NCFH began working with CDC to address H5N1 outbreaks. This effort included outreach via promotores de salud—i.e., community health workers in Spanish-speaking communities—and surveys conducted in several states. In March–September 2025, NCFH selected sites in California, Colorado, and Minnesota, all states with H5N1 outbreaks in cattle, as well as in New York, Vermont, and Washington, three states without detections. They then selected two counties in each of the six states for their survey, Alcauter noted.
The multiphase project relied heavily on community engagement. Alcauter emphasized that in prior cross-sectional surveys with farmworkers, NCFH utilized a rigorous sampling process of random selection from various housing, community, and work sites. However, she described how increased immigration enforcement activities in 2025 necessitated a shift in strategy, leading NCFH to employ a variety of sampling methods. In Vermont, Minnesota, Colorado, and New York, NCFH used referral sampling, relying on partner organizations for initial referrals. They then employed snowball sampling in which referred participants aided in recruiting additional farmworkers. In California and Washington, NCFH utilized random site recruitment at grocery stores, laundromats, and other community locations, in addition to referral and snowball sampling. Eligibility criteria stipulated that participants be 18 years of age or older; not paying other people to work in agriculture, as in the case of employers or contractors; and had worked at least 30 days on a dairy in the selected county since January 1, 2024, Alcauter detailed.
The participants totaled 708 across the 12 selected counties in 6 states. Alcauter explained that the findings are weighted based on the estimated number of dairy workers in each state. The states with H5N1 detections have more cows and more dairy workers, and the data from those states are therefore weighted more heavily. In terms of demographics, 86 percent were male and approximately 83 percent were aged 54 years or younger. Almost 80 percent of participants were born in Mexico, 8 percent
originated in Guatemala, and 7 percent were born in the United States. On average, respondents had 8 years of U.S. work experience across industries and had completed 8 years of schooling. Approximately 15 percent of farmworkers identified as Indigenous, whether racially, ethnically, or as speakers of a Mesoamerican Indigenous language. Farmworkers sampled spoke 21 different languages, most of which were Indigenous languages spoken in Mexico and Guatemala. The languages most spoken were Spanish, English, Zapotec, Mixtec, Tseltal, Tlapanec, and Tojolabal, said Alcauter.
The survey assessed awareness of H5N1 or “bird flu.” Alcauter highlighted that 70 percent of farmworkers in states with H5N1 detections had heard of the virus, in comparison with only 34 percent of workers in states with no detections. Alcauter recalled her pre-survey expectation that more workers would have heard of the virus, particularly in Washington state. About one-quarter of participants were aware that H5N1 can cause illness in humans. Noting that 66 percent of farmworkers had paid sick leave, she described this finding as concerning, given that all the states sampled require businesses with one or more full-time employees to provide paid sick leave. She emphasized that 36 percent of participants indicated having worked while sick, a proportion similar to that of the workers without paid sick leave. Less than half of farmworkers reported having some form of health insurance, with 22 percent covered by public insurance such as Medicaid or Medicare, 13 covered by private insurance plans, and 6 percent unsure of the type of insurance they had, said Alcauter.
Comparing farmworkers in states with detections and in those without, the assessment examined current rates of PPE usage, Alcauter stated. She clarified that current rates, versus rates at the time of H5N1 detection, were used to avoid recall bias. As shown in Figure 4-1, gloves and rubber boots were the types of PPE most frequently used. In states with H5N1 detections, 84 percent and 77 percent used gloves and rubber boots, respectively. Usage in states without outbreaks was actually higher, at 92 percent for gloves and 89 percent for boots. For all types of PPE recommended by the National Institute for Occupational Safety and Health (NIOSH), rates were higher in states with H5N1 detections. In these states, 35 percent of farmworkers wore N95® respirators, 57 percent used goggles, 57 percent wore coveralls or aprons, 24 percent used head covers, 27 percent used face shields, and 11 percent wore boot covers.
In qualitative interviews, farmworkers reported logistical challenges with using PPE. However, several participants remarked that adjusting to PPE requirements during the COVID-19 pandemic was difficult, but with time, implementing PPE became routine. When asked who is responsible for purchasing PPE, a majority of respondents indicated their employer. For most types of PPE, less than a quarter of participants reported being responsible for buying PPE and three-quarters indicated that their employers
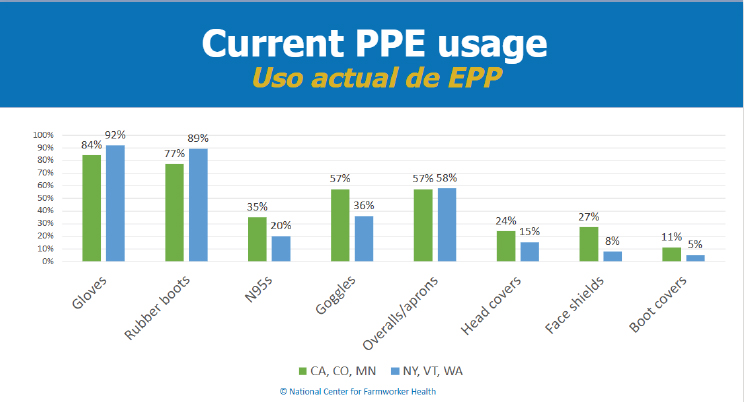
NOTE: PPE = Personal protective equipment.
SOURCE: Alcauter presentation, September 29, 2025; figure courtesy of National Center for Farmworker Health.
provide it. Rubber boots were the outlier, with 72 percent of workers stating that they paid for their boots. In some cases, employers offered a limited amount of PPE and workers were responsible for replacing it. Some farmworkers indicated that they were unable to use employer-provided gloves due to limited size options or lack of latex-alternatives for people with allergies. Describing the finding that a majority of farmworkers have access to employer-provided PPE as promising, Alcauter emphasized that some farms provide little to no PPE to their workers.
PERSONAL PROTECTIVE EQUIPMENT TRAINING AND EDUCATION PROGRAMS
Anna Meyerhoff, senior bilingual agricultural safety and education coordinator at the New York Center for Agricultural Medicine and Health (NYCAMH), provided an overview of barriers to effective use of PPE and outlined methods of addressing these barriers. She explained that agriculture features a diverse workforce, and PPE—particularly respirators—are not designed in a sufficiently wide range of shapes and sizes to accommodate all workers. Rather, PPE tends to fit large, tall men, and many farmworkers do not have this body type. For example, Meyerhoff was on a vegetable farm conducting respirator fit tests, assisting a petite Mexican
woman in trying every N95® option they had, including foldable units. None of the respirators sealed properly to her face, which featured high cheekbones. In addition to challenges in fit, many farmworkers have not been given enough information about how their PPE works or the benefits of wearing it. Comfort issues can arise when wearing PPE for prolonged periods of time. The availability of PPE may be limited by supply chain issues, and farms may have challenges sourcing adequate quantities of PPE to meet the need. Meyerhoff added that the appearance of employer-provided PPE does not always match employee preferences, and she gave the example of a dairy farm that was only able to purchase bright pink gloves for workers in the milking parlor.
Highlighting the influence of perceived risks and rewards, Meyerhoff noted that some farm safety hazards are more apparent than others. For instance, she often conducts fit testing with farmworkers exposed to pesticide or foot bath chemicals. The bright blue of copper sulfate is highly visible, and formaldehyde has a strong smell. Moreover, these substances can cause immediate symptoms such as burning eyes. In contrast, the presence and risk of pathogens may not be as obvious. She underscored that not all employees are aware of zoonoses, and those who are may not perceive the risk of illness to merit the discomfort or annoyance of wearing PPE. Meyerhoff noted that respirators can become uncomfortable to wear in certain conditions or when worn for prolonged periods of time. For instance, when active employees sweat, respirators may slide on their faces. She recalled that wearing an N95® respirator for a 12-hour shift in a health care setting often caused bruising to the bridge of her nose. Similarly, Meyerhoff said that goggles can be large, bulky, and uncomfortable on one’s face. In contrast, smaller, closer fitting, anti-fog goggles with a soft band tend to provide more comfort.
A dedicated, convenient space for storing, donning, and doffing PPE can encourage use, stated Meyerhoff. She recounted farms in which PPE was stored in the employer’s office, accessible only to farmworkers aware of its location and willing to stop work to seek it out. In the absence of designated locations for PPE to be stored after use, it may be misplaced and can also become contaminated. She noted that disposable gloves have ended up in manure systems, causing clogs. In New York, many dairy workers live in employer-provided housing. Although these facilities typically have a mud room or laundry room, employees do not always remove their work clothes before entering their living quarters. In contrast, some sites expect employees to change into uniforms upon arriving at work and doff this clothing before going home. Meyerhoff underscored the importance of providing PPE and making it readily accessible in ensuring that all employees willing to wear PPE are able to do so.
Other challenges to effective PPE use on farms include facial hair, said Meyerhoff. She shared a graphic published by NIOSH that shows dozens of facial hair styles and the corresponding effect on filtering facepiece respirator fit.2 She noted that even people with clean-shaven faces may fail to attain a proper seal due to sideburn length. Additionally, NIOSH has published information about counterfeit respirators that are designed to mimic the appearance of NIOSH-approved products but have not undergone testing and evaluation and may not offer the same level of protection (NIOSH, 2021). Meyerhoff explained that supply chain issues can lead vendors or employers to purchase products from unfamiliar sources. During the COVID-19 pandemic, she witnessed the use of numerous respiratory protection devices that were not NIOSH-approved. Meyerhoff clarified that respirators have two straps that go around the back of the head, and masks with ear loops are not approved respirators.
Meyerhoff outlined training tips that she repeats each time she conducts fit testing. Explaining that a respirator is a large filter that blocks certain particles, she identifies the cartridges and details the protection they offer as well as their limitations. She demonstrates how to inspect the respirator to ensure it is in good working order; how to place it on the face, mold it to the contours of the face, and adjust the straps; and how to determine whether a good seal has been established. Noting the challenge of checking the seal on an N95®, Meyerhoff remarked that this process is more easily observed with an elastomeric respirator because the wearer can see and feel it expanding and collapsing during the positive and negative pressure seal checks. Even in cases where donning, adjusting and seal checks are carefully completed, respirators can shift on the face and lose their seal due to commonplace factors on farms including activity, heat, sweat, talking, and fans blowing. She stated that farmworkers do not want fact sheets, and working directly with people to explain, demonstrate, and repeat the process of proper respirator use is more effective. Having farmworkers explain and demonstrate respirator use to one another or to the trainer is helpful in ensuring understanding. Currently, NYCAMH is involved in a grant-funded project collecting feedback from Spanish-speaking respirator users to gain insight about preferred types of educational materials and formats. Meyerhoff underscored the importance of creating opportunities for farmworkers to ask questions about H5N1 and other topics of concern.
Highlighting success stories, Meyerhoff shared bilingual educational materials in comic book format designed for pesticide applicators, dairy
___________________
2 The facial hairstyle and filtering facepiece respirator graphic is available at https://www.cdc.gov/niosh/media/images/2024/12/npptl_info_facialhairstylesandffrs_2017.jpg (accessed October 28, 2025).
farmworkers, and respirator users.3 Farmworkers find these highly visual materials and direct training to be effective methods for learning about proper PPE use, she remarked. Working with small groups, trainers should offer numerous respirator options to ensure that each person finds a model that fits. Emphasizing the importance of engaging farmworkers in PPE decisions, she offered the example of a farm that accomplished consistent uptake of high-visibility vests by all employees. Meyerhoff explained that before directing workers to wear the garments, the employer asked them for their sizes and for their preferences among different options. Engaging workers in the process and soliciting their input achieved better results than efforts she has seen on other farms. Meyerhoff remarked that PPE uptake is facilitated by clearly communicating the purpose of PPE, storing PPE in locations convenient to farmworkers, providing PPE options that are somewhat comfortable to wear, and offering employees the opportunity to ask questions and offer input.
AGRICULTURAL EXTENSION PERSPECTIVE
Gino Lorenzoni, associate professor at the Poultry Science and Avian Health PennState Extension, offered an overview of barriers to disease prevention efforts in Pennsylvania. He noted that avian influenza is found in poultry and dairy livestock as well as in wild birds and mammals. Given the unlikelihood H5N1 will soon disappear, Lorenzoni works to train the diverse poultry community, which is comprised of large poultry operations, mid-sized facilities, and small farms and backyard flocks. Describing large producers as highly organized, he highlighted that multiple teams provide formal training to these operations, and biosecurity plans—a requirement for federal indemnity—are often in place. Although PPE use is often imperfect, these large-scale facilities have a solid awareness of zoonotic risks and the associated need for PPE, he said. In contrast, mid-sized Pennsylvania farms often feature very low PPE use. Numbering in the thousands, these farms pose several training challenges. Extremely limited training resources are not adequate to engage with all farms, particularly given that professionals maintaining biosecurity clearance are limited to visiting no more than two farms per week, he explained. Moreover, some mid-sized farms are run by the Amish community, and abstinence from electronic devices can pose communication challenges. Noting that half of Pennsylvania outbreaks began in backyard flocks, Lorenzoni stated that requirements for backyard flocks in Pennsylvania are minimal and communication with flock owners is low. He added that efforts to educate poultry owners about
___________________
3 These bilingual educational materials are available at https://www.nycamh.org/resources/nycamh-resources/ (accessed October 28, 2025).
biosecurity, PPE, and zoonotic risk often include extensive information and long lists of tasks that can overwhelm owners of mid- and small-size farms.
Lorenzoni emphasized that consistent PPE use is influenced by practicality, cost, comfort across both very high and very low temperatures, and ease of use. He noted that PPE meeting all of these criteria simultaneously does not currently exist and may not be achievable. Lorenzoni posited that H5N1 might be better controlled via a high-risk-based approach. Rather than instruct farmers to consistently implement numerous precautions, trainers could explore lower levels of PPE that offer substantial protection. He suggested looking for steps that protect 99 percent of farmworkers 99 percent of the time. Acknowledging that safety advocates are often reluctant to recommend steps that leave 1 percent of the population unprotected, Lorenzoni remarked that oftentimes the highly comprehensive plans commonly recommended are not adopted. This is particularly true for mid- and small-sized farms, and he submitted that consensus for low-risk activities could yield more amenable recommendations. For instance, safe completion of typical daily farm activities may only require goggles and inexpensive face masks. He pointed out that gloves are commonly recommended, but the likelihood of contracting a virus through intact skin is low. In contrast, activities such as disposing of dead birds may require gloves. Moreover, handwashing facilities are not always available on farms, and providing farmworkers with soap and water could have substantial implications for safety.
Lorenzoni clarified that high-risk situations, such as active outbreaks, require higher levels of PPE, including properly fitted respirators, goggles, coveralls, hairnets, and boots. Moreover, outbreak response requires well-trained employees wearing full PPE, he added. Describing that some situations involve hundreds of responders, he remarked that screening for susceptibility factors is lacking. Factors that could increase an individual’s susceptibility to viruses include older age, compromised immune system, corticoid treatment, acute or chronic respiratory disease, or testing positive for COVID-19. The likelihood a person will become ill is affected by susceptibility and viral load—i.e., the amount of virus an individual comes into contact with. Lorenzoni suggested that mitigation should involve PPE to minimize viral load and the removal of susceptible individuals from high-risk response teams.
DISCUSSION
Risk Perception and Education Gaps
Lipton asked about the influence of risk perception on PPE use at the individual or farm level and about awareness gaps hindering people from
taking appropriate safety measures. Lorenzoni responded that farmworker education should focus on basic PPE needs and the most effective ways to mitigate virus transmission. Although many modes of transmission are likely at play for H5N1, he stated that they are probably not equally effective. Safety advocates should prioritize measures according to the most likely means of contracting disease, he suggested. For instance, consideration could be given to whether workers would be better protected by wearing respiratory protective devices or by avoiding rubbing their eyes with dirty hands. Control measures that address the most common modes of transmission could offer protection for most people and are more likely to garner adherence than comprehensive measures, said Lorenzoni. Rodriguez commented that people cannot be concerned about an issue until they are aware of it. She recalled that after completing the occupational survey, many farmworkers had questions about H5N1. People’s typical sources of information may not alert them to pathogen risks, Rodriguez emphasized, highlighting the importance of delivering education to employees at their places of work.
Cultivating a Farm Culture of Safety
In response to a question about how to cultivate a culture of safety on farms, Rodriguez noted three organizational levels: owner, middle manager, and farmworkers. Middle managers serve as liaisons between owners and workers, translating urgent issues from the dairy level to the individual level. She described how they often hold “tailgate talks” on the work site in which they convey the importance of PPE and other steps workers can take to protect themselves. Rodriguez contended that middle managers are therefore a resource in disseminating safety messaging from the owner to the workers. Meyerhoff observed that farms that prioritize safety typically integrate safety considerations into all meetings and plans. These farms usually have a safety committee or safety officer, and these individuals ensure that messaging is provided across day and nighttime shifts and in multiple languages. Underscoring the role of owners in shaping work culture, she recounted that employers sometimes introduce her by saying, “This person is here because I want you all to get home safe and healthy.” Such messaging reflects that the values on the farm extend beyond profit, food production, and animal care to include concern for farmworkers. She added that modeling the behaviors one wants to see, such as wearing PPE, is important in encouraging uptake. Soliciting input from farmworkers can aid in addressing issues and concerns, as workers are often good problem solvers with ideas about how to improve procedures. Thus, communication with owners, middle managers, and farmworkers aids in cultivating a culture of safety, said Meyerhoff. She acknowledged that state and federal
policies and market forces are also at play, and these dynamics can affect work culture. Larger farms, such as those subject to Occupational Health and Safety Administration (OSHA) enforcement activities, may have the ability to adopt safety programs that smaller operations might not have the resources to implement.
Addressing Personal Protective Equipment Comfort and Fit
Given that PPE often fails to meet the comfort and aesthetic preferences of workers, Lipton asked how to address the gap between what employees would be willing to wear and PPE that is currently available. Rodriguez highlighted the importance of asking farmworkers for their input on what they like and dislike about different types of PPE. For instance, she observed that workers in Texas and New Mexico milk sheds often wore neck gaiters, and they pulled these over their noses and mouths in dusty conditions and to avoid milk splattering on their skin. She asked them what they preferred about the neck gaiters to N95® respirators. Rodriguez noted this as an example of meeting workers where they are and involving them in the process. Echoing the importance of engaging the end user in communication about a product, Meyerhoff stated that the professionals designing PPE may not be familiar with the activities and preferences of farmworkers or with the agricultural environment. Farmworkers are far less likely to use items that are large and bulky, fog up, or are unflattering than items that fit well, do not hinder work activities, and are stylish. Soliciting farmworker feedback and integrating it into PPE design could improve uptake, Meyerhoff maintained. Moreover, manufacturers should consider diversity in fit and sizing, she added. For instance, many safety glasses are too wide for narrower faces and leave gaps large enough for particle entry. Some respirators do not achieve proper fit with shorter people. Meyerhoff contended that PPE manufacturers should consider the diversity of the agriculture workforce—which features many women and immigrants of varied height and body shape—and offer a range of styles and sizes to accommodate farmworkers.
Respirator Fit Testing Requirements
In response to a question about whether the OSHA requires multiple styles and sizes of respirators and specifies procedures for respirator storage, donning and doffing, and user seal checks, Meyerhoff clarified that many farms are exempt from OSHA regulations due to having a small number of employees. Although these regulations reflect best practices, small operations may not have personnel able to conduct fit testing, she explained. Many people refer to filtering facepiece respirators as “dust masks” and do
not realize that they require fit testing and seal checking. Meyerhoff stated that she must often explains the importance of a respirator seal to people who apply pesticides. Due to the high cost of equipment and limited availability of quantitative fit testing services, some farms purchase qualitative kits that contain hoods, nebulizers, and saccharin solution and/or Bitrex for fit testing their workers. However, these tests are less accurate than quantitative fit tests and are not a good option for people with impaired sense of taste and smell, a condition that has become much more common since the emergence of COVID-19, she noted.
Farmer Reluctance to Report H5N1
Wilson addressed a query about his initial reluctance to report H5N1 after suspecting an outbreak on his farm. He replied that initial detection of H5N1 in cattle occurred at a farm in North Texas, and the outbreak quickly spread, affecting many dairy farmers in Central Michigan. Until the discovery that pasteurization kills H5N1, dairy owners worried that the virus would prevent them from selling milk or cows, he explained, adding that most dairy farmers supplement cash flow with cow sales. Despite the U.S. Department of Agriculture Farm Service Agency instituting a program to pay producers for a certain amount of loss, farmers were fearful of completing government forms, Wilson remarked. The depopulations that took place on nearby turkey and egg farms also contributed to testing reluctance. However, Wilson contacted MMPA and was informed that although buyers were initially concerned about H5N1, they were reassured once they learned that pasteurization kills the virus. Numerous visitors came to his farm to test and conduct research, and much was learned during the first 3 months after H5N1 was detected.
Respiratory Protection Technology
Lipton asked whether the agriculture market is sufficiently large to entice investment in research and development in respiratory protection technology. Wilson remarked that milking parlors are open air and feature exhaust fans for ventilation, and these conditions do not warrant respirators. In contrast, the poultry industry involves confined spaces, making respirator use important, said Wilson. Meyerhoff replied that agriculture as an industry contributes billions of dollars to the New York state economy and its large workforce represents an enormous potential PPE market, particularly when including employees of both livestock and produce operations. However, wide-scale adoption of PPE relies on affordability, she stated. Given the possibility of exposure to dust and particulate, pesticides and footbath chemicals, and pathogens such as H5N1, farms involve numerous
risks that warrant respirator use. Meyerhoff suggested that manufacturers could engage agribusiness or producer groups to explore their level of interest. Lorenzoni remarked that the market is large and will likely continue to grow as animal disease awareness efforts expand.
Elastomeric Respirators
Regarding a question about acceptance rates of elastomeric respirators, Meyerhoff stated that most of the fit testing she performs is on these devices. Both half-face and full-face elastomeric respirators offer the benefit of easily performed seal checks, given that properly-adjusted devices pull on the face during checks. A box of N95® respirators is often used up quickly; however elastomeric respirators are reusable and do not necessarily need to be thrown away after a single use. Meyerhoff explained that in situations where every worker is provided with an elastomeric respirator, a sense of ownership and comfort with the device develops as users become familiar with wearing and caring for them. Noting that wearing an N95® has caused irritation and bruising on her face, she remarked that elastomeric respirators can feel more comfortable and easier to adjust. Commonly worn by farmworkers applying pesticides and working with animal foot baths, workers generally like them, said Meyerhoff, adding that they are a good investment for farms willing to purchase them.
This page intentionally left blank.















