Personal Protective Equipment for Influenza A(H5N1) in High-Risk Farm Settings: Proceedings of a Workshop (2026)
Chapter: 6 Improving Existing Personal Protective Equipment Access and Feasibility of Use
6
Improving Existing Personal Protective Equipment Access and Feasibility of Use
The fifth session of the workshop (1) focused on barriers to personal protective equipment (PPE) access and feasibility of use; (2) examined administrative and engineering efforts to improve PPE distribution, feasibility, and cost; (3) explored alternative respirator designs; and (4) discussed key research needs to evaluate and improve the effectiveness of PPE. Ximena Vergara, chief of the California Department of Public Health (CDPH) Hazard Evaluation System and Information Service and adjunct assistant professor of epidemiology at the University of California, Los Angeles, moderated the session.
ENGAGING WORKERS IN WORKER HEALTH INITIATIVES
Elon Ullman, research scientist and industrial hygienist at CDPH, discussed the roles of relationships and education in addressing barriers to PPE uptake. As part of CDPH’s Influenza A(H5N1) response, Ullman works in areas where respiratory PPE is required under the California Occupational Health and Safety Division Aerosol Transmissible Diseases Standard.1 Additionally, he conducts respirator outreach via the Program for Respirator Outreach, Training, Education, and Community Testing (PROTECT), a program funded by the National Institute for Occupational Safety and Health (NIOSH) and designed to improve education and increase fit testing for workers without respiratory protection programs. Noting that the Health Belief Model can be utilized in understanding why people choose to
___________________
1 California Code of Regulations, Title 8, §5199. Aerosol Transmissible Diseases.
engage in behaviors to improve their health, Ullman suggested that within the context of occupational environments, the employer’s choices should be the focus rather than those of individual employees (Alyafei and Easton-Carr, 2024). Employers bear the responsibility of ensuring their employees are protected from hazards, he added. In making determinations regarding PPE requirements, employers should consider barriers to PPE usage and the susceptibility and severity of the threat in terms of how sick infected workers could become. Ultimately, an employer’s beliefs regarding whether PPE will protect workers from the threat often drives decision-making. Ullman remarked that an employer’s choice to distribute and train employees on PPE can be strengthened by disease outbreak response, advice from family members, and public health messaging.
Barriers to Farmworker Personal Protective Equipment Uptake
Outlining barriers to respiratory protection in farm settings, Ullman noted that supply chain shortages can impede PPE usage. However, California has a sizable state stockpile, and a feature of its H5N1 response is making this stockpile available for distribution to farms, local health jurisdictions, and community-based farmworker organizations. He underscored the value of PPE stockpiles in rapid response during emergency situations. Although PPE for respiratory protection is currently widely available in California via stockpiles and commercial outlets, distribution has posed challenges to the farming industry. California dairy workers are not represented by a union or other centralized organization, and thus CDPH employed a decentralized PPE distribution approach via local health jurisdictions. Ullman highlighted that Western United Dairies, a trade organization representing a majority of dairy owners in western states, partnered with CDPH to serve as a trusted messenger in distributing PPE to dairies.
Despite working relationships between local health departments, community-based organizations, and trade organizations, Ullman explained that relationships between farmers and governments were not well established at the time of H5N1 detection, and the farming community’s perception of the H5N1 threat was disconnected from that of public health. Given that each infection presents an opportunity for the virus to mutate and spread further, the public health sector focused on preventing the spread of H5N1 to mitigate the potential severity of the disease. In contrast, many farmers perceived the risk of H5N1 to be low. Early in the outbreak, many cows were falling ill but only a small number of cases were found in humans, leading many farmers to focus on their herds. Ullman remarked that the dairy industry lacks historical experience with respiratory protection, and most of the employers CDPH contacted had a limited understanding of this PPE. For instance, many people do not understand the
difference between a tight-fitting respirator and a loose-fitting mask. Ullman underscored the role of closing this knowledge gap in increasing adoption of respiratory protection. In addition to limited understanding, the environmental context poses barriers to PPE uptake. The dairy environment is often hot and wet, and dairy work is physically active. These conditions can contribute to heat stress while wearing respirators, said Ullman, and they warrant precautions to keep PPE dry.
Addressing Personal Protective Equipment Uptake Challenges
Ullman stated that addressing barriers to PPE use would benefit from stronger relationships between public health and farms. In California, the utility of the large stockpile of PPE was constrained by its limited distribution, highlighting the importance of trusted distribution networks in providing PPE access to farmworkers. These networks can include local health jurisdictions, community-based organizations, and professional societies. He emphasized that in order for PPE distribution efforts to be successful, the organizations distributing PPE must be trusted by the communities they are distributing to and education should be included as part of the initiative. Workers are unlikely to wear PPE if they do not understand why specific PPE is recommended. Ullman remarked that when trusted industry leaders understand the benefits of PPE, they can disseminate messaging to workers throughout organizations. Acknowledging that heat stress presents a substantial barrier to wearing a tight-fighting N95® or elastomeric respirator in the milking parlor, he highlighted that powered air-purifying respirators are a more comfortable option. These respirators feature a hood and are connected to a filtered fan system housed on a belt. He described how powered air-purifying respirators offer a high level of protection while simultaneously cooling the wearer, and the hood protects the eyes and mouth from splashed milk droplets. In lieu of such respirators, milking parlors should improve cooling mechanisms to enable comfortable use of elastomeric or N95® respirators, Ullman maintained.
The current moment is a critical window between the first wave of H5N1 outbreaks and the potential for another wave, said Ullman. He contended that this is an opportune time to increase education about the potential severity of H5N1 and the importance of control measures—such as respiratory protection and quarantine—to prevent the spread of airborne transmission. Although barriers to PPE use are substantial, they are surmountable, particularly given the relative newness and unfamiliarity of airborne hazards in the dairy industry, he noted. In a context of wildfires and viral outbreaks, respirators are increasingly relevant not only to occupational environments but to society at large, Ullman concluded, adding that both farmworkers and the public need more education about respirators’ purpose and benefits.
ENGAGING PARTNERS IN PPE DISTRIBUTION
Heather Riden, director of outreach at the Western Center for Agricultural Health and Safety (WCAHS) at the University of California, Davis, explored the roles of ongoing partnerships and resource development in training, outreach, and PPE distribution efforts. As one of 12 agricultural centers funded by NIOSH, WCAHS employs a multifaceted, collaborative approach to addressing H5N1 in California. This approach centers on continuous partnership, resource development, training and outreach, and PPE distribution. Riden emphasized that the success of PPE distribution is contingent on other approach components. Trusting, ongoing relationships established and maintained through regular communication allow WCAHS to rapidly engage a network of agricultural partners when important issues arise. She noted that the COVID-19 pandemic spotlighted the value of these partnerships in providing resources and trusted messengers for timely topics. She described how WCAHS collaborates with community-based organizations, employers, employer associations, state agencies, and other groups concerned about safety in the agriculture workplace. These partners guide WCAHS in identifying knowledge gaps and challenges in implementing safe practices. Underscoring the value of bidirectional communication, Riden emphasized communicating the rationale for safety measures while also listening to the challenges workers face in implementing them.
Focusing its research on the fundamentals of H5N1, WCAHS began publishing information about the virus in May 2024, before the first human case was detected in California, said Riden. With the goal of preventing H5N1 transmission in humans, the organization created resources for farmworkers, such as graphics shared on social media. The educational materials—available in both English and Spanish—are tailored to the intended audience to ensure appropriate reading level and content. As outbreaks continued, WCAHS developed resources featuring “frequently asked questions” from their partners. Training and outreach activities have included attending and distributing information and PPE at community events, employer conferences, and sessions for agricultural community members. Virtual events include online H5N1 webinars and monthly meetings that convene promotoras (i.e., community health workers who engage Spanish-speaking communities) and other community members working with farmworker communities across the state, Riden noted.
Conversations with partners and at outreach events have informed WCAHS about more effective H5N1 communication strategies as well as highlighting various challenges, Riden stated. For instance, the organization worked to assure the general public that their risk for H5N1 was low while simultaneously communicating a higher risk for specific occupational groups. Given that communities are integrated and that many people are
unfamiliar with H5N1, she noted that creating clear, accessible information about varying risk levels can be challenging. Additionally, communicating the importance of the seasonal flu vaccine when a vaccine for H5N1 has not yet been developed poses challenges, and Riden noted they tried to avoid discussing virus reassortment due to the confusion the concept raised. Community outreach highlighted that a number of people living in rural communities have backyard flocks of chickens. Although WCAHS focuses on occupational exposures, she said that recognizing and acknowledging the full range of exposure potential is important in offering responsive education and PPE. Riden added that unpasteurized milk is consumed in some rural communities due to both financial and cultural reasons, and the organization worked to discuss the importance of pasteurization in a respectful manner.
California has a robust supply of PPE, and WCAHS utilized NIOSH funding for distribution, Riden highlighted. The organization mailed large quantities of PPE upon request throughout the state, primarily to central and southern California, with high concentrations of PPE distributed to Fresno County. They also delivered van loads of PPE to numerous community partners’ offices and to community events. Riden emphasized the importance of maintaining positive working relationships with organizations during non-emergency times, as this enables rapid engagement with a network of partners when important issues arise. She added that PPE distribution is most effective when partners are compensated for their time in facilitating the initiative. During times of crisis, community organizations and employers are particularly short on time, and WCAHS eliminated the need for partners to dedicate time to picking up PPE by shipping or personally delivering it to them. Riden underscored the importance of distributing PPE for both occupational and personal use in protecting against as many potential exposure routes as possible. Acknowledging differences in comfort between respirator use indoors and outdoors, she emphasized the importance of listening to employers, producers, and workers who describe challenges or work hazards associated with PPE use.
To improve PPE distribution, Riden highlighted the importance of clearly communicating why, when, and how to use appropriate PPE. In the absence of education, people may be distrustful, disinterested, or unwilling to use PPE. Additionally, workers are eager to know whether outbreaks are occurring at their workplace or in the surrounding area, and this information should accompany the provided PPE, she noted. Riden stated that PPE provision should be free of cost and year-round to allow its use in situations other than the specific public health crisis an organization is managing. For instance, some people in California are not worried about H5N1, but they are contending with wildfire smoke in their region. She maintained that organizations should enable and encourage PPE use for various safety
purposes, and equipment should not be designated to any specific purpose. In describing diverse distribution methods as essential, she remarked that workers receive information and resources from a variety of individuals and groups, and these networks should be utilized. Distribution diversification enables workers who do not receive PPE at their workplace to access it from community organizations or other sources. Moreover, seeing PPE offered at multiple locations emphasizes to workers the importance and legitimacy of PPE, said Riden.
RESEARCH PRIORITIES
Jin Pan, assistant professor of occupational and environmental health at the University of Iowa, reviewed data on improving PPE technologies, accessibility, and feasibility of use. Pan focused on respirators, given that respirators present more challenges for use during farmwork than do gloves, boots, and goggles; additionally, reluctance and low compliance with PPE use is higher for respirators and other respiratory protective devices than for other types of equipment. However, she noted that some of the suggestions and principles that pertain to respirators can also be applied to other types of PPE. Respirators filter out virus with the same mechanisms by which they filter dust and other particles. Respirator performance is partially dependent on particle size, and efficiency is driven by several physical mechanisms. The combinations of filtration mechanisms create varying levels of efficiency for different particle sizes, with minimum efficiency reached for particles 0.1–0.3 µm in diameter (Hinds and Zhu, 2022). This minimum efficiency determines the rating for a respirator and sets the ideal performance of the device when it has a perfect seal. For example, the NIOSH N95® standard requires minimum efficiency to be equal or greater than 95 percent. Pan stated that efforts to increase PPE access and feasibility of use should strive to sacrifice as little efficiency as possible in order to provide adequate protection.
Outlining numerous barriers to PPE accessibility and feasibility of use, Pan highlighted that the expense of providing disposable or reusable respirators to workers can be high. For instance, a single disposable respirator costs as much as a dollar, and the total expense to a farm accumulates rapidly if tens of employees use daily respirator replacements. At an annual cost of thousands of dollars, disposable respirators can pose a considerable financial barrier to small-scale farms. Reusable respirators can also be expensive and require disinfection and cartridge replacement. Pan remarked that these costs may contribute to farm owner hesitancy to distribute respirators to workers, particularly when respirators are recommended outside of active outbreaks as a preventative method for potential disease transmission.
The discomfort of respirators poses a substantial barrier to use on farms, said Pan, explaining that highly efficient respirators can reduce breathing rate and cause heat stress. When farmers experience discomfort while wearing respirators, they often adjust the devices, and this can affect the seal and cause gaps between the respirator and face, thereby potentially compromising the performance of the PPE. Discomfort also likely contributes to low compliance, she added. Moreover, fit testing is not widely practiced among farmworkers, and thus the effectiveness of the respirators cannot be guaranteed. Pan added that fit testing requires training and time as well as an investment in fit testing equipment, which are factors that can be burdensome to farm owners. Additionally, short-term supply shortages sometimes occur, particularly in rural areas, causing a delay between an outbreak and receiving and using the respirators. Pan reiterated that many farmworkers do not wear respirators outside of active disease detection at their worksites.
Research on Extending the Use Life of Disposable Respirators
Pan outlined research findings that can inform efforts to addressing barriers related to respirator cost and supply. Existing methods have demonstrated ability to disinfect used disposable respirators without degrading performance. Typically, people discard disposable respirators on a daily basis. However, a study of disposable respirators produced by 3M found that disinfection with a vaporized 59 percent hydrogen peroxide concentration through 10 disinfection cycles did not degrade device performance compared to an unused respirator (Jatta et al., 2021). In fact, they found that the limiting factor for reusing disposable respirators was not reduced performance but rather the longevity of the devices’ elastic straps. Thus, in the absence of physical damages, including those related to loss of fit due to wear and repeated donning and doffing, disposable respirators could potentially be disinfected and reused without compromising effectiveness as long as the elastic straps function properly. Pan stated that reusing respirators can reduce the annual cost of PPE, although she acknowledged that the idea of disinfecting and reusing respirators may sound intimidating to many farm owners.
Another study from scientists at NIOSH found that use of expired respirators is feasible if the storage conditions are appropriate, Pan highlighted. They collected stockpiled respirators manufactured between 2003 and 2013 and evaluated the devices 5 years later in 2017–2019 (Greenawald et al., 2020). They found that 98 percent of the thousands of 3M expired respirators passed NIOSH standards. This signifies that if respirators are stored properly and not exposed to high heat or relative humidity, they can continue to perform well years beyond their expiration date, she
explained. The use of properly stored expired respirators could reduce cost and waste for distributors and users. Exploring potential prolonged use of respiratory protective devices, Pan conducted a study of disease transmission via respiratory protective devices contaminated by an airborne virus (Pan et al., 2023). Evaluating six types of respiratory protective devices—including N95® respirators, surgical masks, and cloth masks made from polyester, cotton knit, cotton poplin, or a nylon/spandex mix—she contaminated the respiratory protective devices with aerosolized, viable, infectious SARS-CoV-2 and then applied them to artificial skin. She was able to detect infectious virus on the surfaces of the respiratory protective devices and respirators, but not on the artificial skin. Similarly, a 2024 study found that surgical masks contaminated by infectious influenza virus do not transfer viable virus to fingers (Fan et al., 2025). Although they were able to detect viral RNA on the surface of the respiratory protective devices, they could not detect viral RNA nor infectious virus on fingers that palpated the respiratory protective devices. Pan explained that the results of these two studies suggest that people may not have to disinfect respirators—even those contaminated by airborne viruses—to receive protection from the devices. Given that viruses do not easily transfer from respiratory protective devices to skin, reusing a respirator without disinfection constitutes a low risk of contracting infection. Thus, Pan contended that in cases of supply shortages during emergent crises, respirators can be reused without disinfection because the risk of disease transmission by touching contaminated respiratory protective devices is low.
Research on Alternative Respirator Models and Designs
Broadening the choices of respirators available can also increase access, said Pan. During the early stages of the COVID-19 pandemic, researchers exploring alternatives to NIOSH-approved devices, which were in short supply, examined whether internationally certified respirators passed NIOSH standards. A group of scientists at NIOSH evaluated more than 200 brands and models of internationally certified respirators that claim to offer the same level of effectiveness as N95® respirators. They found that approximately 39 percent of the models tested consistently passed the NIOSH N95® standards (Andrews et al., 2021). Additionally, 26 percent of models inconsistently passed the standard, and 35 percent of the models consistently demonstrated a minimum efficiency under 95 percent. Pan emphasized that in the event of a NIOSH respirator shortage during an emergent situation, a data set of international brands and models of respirators that meet NIOSH standards would be valuable in locating appropriate alternatives. Another study evaluated a strategy of utilizing multiple layers of less efficient masks (Chea et al., 2024). During shortages, cloth masks
may be more readily available than respirators and carry a lower price point. Although cloth masks do not perform as well as NIOSH-approved respirators, the study found that the minimum efficiency increased above 80 percent when the layers of cloth masks were doubled. Conceding that the protection offered by double-layer cloth masks is significantly lower than N95® respirators, she remarked that double-layer cloth masks are a potential alternative during respirator shortages in emergent situations. Cloth masks offer the advantages of being easy to wash and reuse, and some people find the soft material more comfortable on the face. However, cloth produces higher resistance to breathing than do filter materials, Pan noted, and cloth masks are not designed to form a seal on the face.
Technology and design can yield alternative respirators, such as three-dimensional (3D) nonproprietary respirators designed to improve fit and comfort while reducing cost, said Pan. Given that cloth masks do not form a seal and may offer less breathability than filter materials, a 3D printed frame that fits around the nose and mouth can improve fit. Pan and colleagues evaluated the cloth mask design with and without the 3D frame, and they found that when printed with rigid material, the frame does not increase the mask’s effectiveness (Tong et al., 2021). However, when the frame is composed of elastomer filaments—yielding flexibility and elasticity to conform to facial structure—it successfully creates a seal against the face and thereby increases the effectiveness of the mask. Pan added that this design makes it possible to add a layer of highly efficient filter material between the two layers of a double-layer cloth mask. The soft cloth is comfortable on the face, the filter material and frame offer protection, and the frame’s flexibility allows adjustment to different facial structures, Pan described.
Additionally, alternative respirator designs include devices in which the entire face piece is 3D printed and features a window into which filter material can be inserted, Pan explained. Research indicates that with proper 3D design and filter materials, 3D printed devices can achieve a minimum efficiency higher than 90 percent (Bezek et al., 2021). She stated that each person’s unique facial structure makes it impossible to design proprietary respirators that perfectly fit all faces. Using 3D printing technology, designers can adapt designs to specific facial types, and users with 3D printing capabilities can tweak facial pieces to fit their faces. In recent years, 3D printer affordability, availability, and reliability have increased, and many facial piece designs are available online to download free of cost, increasing accessibility. She described how these designs stand to reduce the cost of respirators because the 3D-printed facial pieces are reusable; only the insert material requires replacement, and this material costs less than proprietary cartridges for elastomeric respirators. Pan added that making these 3D-printed facial pieces from elastic materials could improve fit on the face.
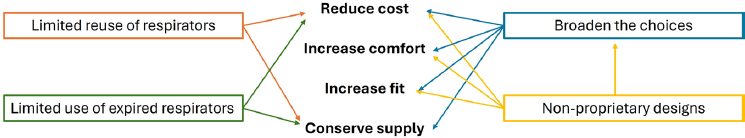
New technologies offer potential in reducing respirator cost, increasing comfort and fit, and conserving respirator supply, said Pan.
Figure 6-1 illustrates how various approaches can have interrelated impacts on cost reduction, increased comfort, increased fit, and conservation of supplies.
DISCUSSION
Testing Expired Respirators
In response to a question about methods of testing the effectiveness of expired respirators, Pan replied that local research institutions or centers equipped with instruments to evaluate respirator performance could test samples from a stockpile of expired respirators to determine whether their performance level had degraded. This practice could avoid wasting functional PPE devices, she added. Maryann D’Alessandro, director of the NIOSH National Personal Protective Technology Laboratory, remarked that many complexities are associated with respirator performance, such as the specific lot that a unit was manufactured in, and she cautioned that any determination about the functionality of expired respirators should extend beyond testing a few samples to include robust study.
Heat Stress Protocols for Respirators in Farm Settings
Vergara asked whether states or NIOSH have developed specific heat stress protocols for H5N1 in dairy and poultry farms, such as rest breaks and cooling measures. Riden noted that WCAHS did not create educational materials related to contending with heat while working in a dairy setting. However, California has indoor and outdoor heat protection standards in place that include elements such as rest, cooling in a location with a temperature lower than the work setting, and drinking water. Underscoring the value of educational materials, policies, and procedures tailored specifically to the work setting, Riden added that worksite considerations should
SOURCE: Pan presentation, September 30, 2025.
factor into the creation of work schedules. Ullman remarked that although many regulations are in place, safety advocates should not assume that all employers and workers are familiar with them. Ullman suggested developing educational materials explaining California’s heat stress standards for indoor and outdoor workers, which could also address potential hazards of control measures and should accompany PPE distributions.
Respirator Evaluation Setting
In response to a question as to whether respirators are ever evaluated in real-world settings, Pan replied that she is not aware of any evaluations performed in the field. In addition to environmental factors such as high humidity, farm activities can create conditions that reduce the performance of respirators. She stated that when work sites conduct Occupational Safety and Health Administration (OSHA) fit testing, this should be performed while simulating work activities to mimic facial changes while working. Acknowledging numerous factors that could potentially change the performance of respirators in the field versus in the laboratory, Pan remarked that this is an area of potential future study. Riden noted that state regulations and recommendations indicate conditions for both voluntary and mandatory use of N95® respirators, emphasizing that these devices should be evaluated in dairies, orchards, and other settings to determine the level of hazard protection that N95® respirators offer in the field.
Alternative Filtration Standards
Given that ASTM International standard F3502 is recognized for protection purposes by the National Fire Protection Association, and that some reusable face coverings meet this standard, a participant asked whether only using standards from specific agencies presents a systemic barrier to PPE use and protection. Ullman noted that the ASTM standard was developed during the COVID-19 pandemic when greater standardization was necessary for respiratory protective devices being worn by the general public. He remarked that in cases where no specific regulation applies, communication with users about the hierarchy of protection of various respiratory protective devices enables them to make informed decisions. For example, some standards may require minimum efficiency of 80 percent protection, whereas an N95® respirator provides 95 percent or above. Ullman underscored that in some cases, regulations such as the California Aerosol
Transmissible Diseases Standard2 and the General Duty Clause3 respiratory protection standards apply, and these standards preclude the use of respiratory protective devices that offer lower levels of protection.
Acceptable Levels of Protection
Vergara asked about balancing ideal levels of PPE protection with alternatives that offer less protection but greater uptake. Ullman replied that given all the barriers to PPE uptake, the use of lower-level PPE is preferable to no use. Acknowledging that various environmental factors and lived experiences pose barriers to compliance with PPE recommendations, he reiterated the importance of communicating the protection levels, feasibility, and legal requirements related to various PPE options. Ullman maintained that communicating scientific data, levels of protection, and recognition of barriers enables users to make fully informed decisions that best suit their lived experiences in their working environments.
Partnerships for PPE Uptake
Vergara asked how state and local agencies can improve working relationships with industry and community groups to increase access and uptake of PPE. Riden emphasized the importance of engaging with groups year-round—during steady state—about topics beyond the improvements that groups need to make. Supporting the needs of communities, employers, and organizations in an attentive, respectful, and responsive manner can foster relationships. She added that groups should be compensated for their efforts, whether in the form of PPE provided at no cost and/or financial compensation for the time and effort contributed to distribution initiatives. Riden stated that these are meaningful approaches to valuing the work of industry and community groups and integrating them into PPE efforts.
___________________
2 California Occupational Health and Safety Division (Cal/OSHA) Aerosol Transmissible Diseases (ATD) Standard, 8 CCR 5199, available at https://www.dir.ca.gov/title8/5199.html (accessed January 7, 2026).
3 29 U.S.C. § 654 Sec.5, available at https://www.osha.gov/laws-regs/oshact/section5-duties (accessed January 7, 2026).











